Ask Dr. Christensen
by Gordon J. Christensen
For more on this topic, go to www.dentaleconomics.com and search using the following key words: automixing devices, Pentamix™, topical fluorides, VarnishAmerica™, Flor-Opal, Prevident®, MI Paste.
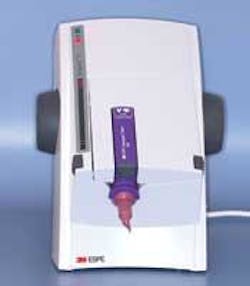
Q The trend in impression dispensing and mixing appears to be the use of automixing devices. However, I am satisfied with my standard syringe mixing gun. Why should I change to an automixing device? Do these machines offer me any real advantages?- Consistency of impression material mixes. Because the automixing machine mixes the same each time, the homogeneity of mixes is consistent.
- Infection control is simple. It is easy to place an infection-control wrap or a piece of household Saran wrap on the activating button of the device, and avoid the infection control challenges encountered with the almost never disinfected syringe mixing devices.
- Minimal waste. The waste observed with automixing devices can be minimal. The device is purged slightly to ensure a homogeneous mix when the mixing tip is placed on the device, and just the amount of material left in the mixing tip is thrown away with the used mixing tip.
- Minimal storage need. If using one centrally located device, an automixer can hold enough material to fulfill the needs of multiple impressions. The operatories are no longer cluttered with tubes and impression material mixing guns.
- Ease of training staff to mix impressions. New staff people can easily be trained to use the devices and educated about the various clinical techniques used in the office and the types of materials necessary for specific needs.
As with any technique, there are some disadvantages. Those disadvantages, in my opinion, include:
- Purchase of the mixing device. When the overall cost of making impressions is considered, this is not a significant disadvantage in light of the advantages of the technique.
- Size of the device. These devices take up a significant amount of space, and if you prefer to have one in every operatory, this is can be objectionable.
- Learning to use the concept. This is not a significant disadvantage, but you and your staff will require a few impressions to become competent with automixing devices.
- Changing to a new impression material brand. This may or may not be a challenge. Most companies that you are currently using have material packages that fit into the Pentamix. However, the best results will be achieved if you use the impression material from the company making the automixing device.
In summary, the machine automixing concept is here to stay. Seldom do I find a practitioner who has changed to machine automixing who wants to go back to one of the other methods. The advantages are relatively obvious.
For more information on this subject and how to make nearly foolproof impressions, see our newest Video, V1931, "Predictable Fixed and Removable Prosthodontic Impressions." For more information, contact Practical Clinical Courses at (800) 223-6569, or visit our Web site at www.pccdental.com
Q I have been using topical fluoride applications for my patients every six months since I started practicing many years ago. I have heard that the effectiveness of these bi-yearly applications is under question, and I am wondering if I should change to another preventive method for both children and adults. What is your suggestion on the most adequate preventive methods available today?A Preventive methods are in a state of flux at the moment. There are several different preventive methods that are being promoted, and it is difficult to determine which one would be best for your patients, and which you can best use in your practice. I will discuss a few of the most popular methods and compare them for you.1.23% acidulated sodium fluoride
Topical application of 1.23% acidulated sodium fluoride has been used for decades. It is well-known to patients and accepted by them. The technique is easily delegated to dental hygienists, and it is not significantly undesirable for patients. Most children tolerate it quite well. However, the effectiveness of routine topical fluoride applications is under question in relation to other preventive methods. There is no question that topical application of these gels, foams, and liquids can increase fluoride in the surfaces of the teeth. Research has been conducted on this concept of fluoride application since the 1960s. Minimal reductions in dental caries have been reported in many clinical studies. However, the period of time before the fluoride level in the superficial tooth structure stays high is short, and six months pass before the fluoride is applied again, minimizing the effectiveness of the technique.
Five percent sodium fluoride
Five percent sodium fluoride varnishes are very popular. The concept has been promoted for many years, but only in recent years have they become used more frequently. Many researchers and organizations are recommending fluoride varnishes for both children and adults instead of the long-used topical acidulated sodium fluoride applications.
Popular, effective brands are VarnishAmerica™ from Medical Products Laboratories™ and Flor-Opal from Ultradent. These products contain nearly 23,000 ppm of fluoride, and their effectiveness is supported in the dental research literature. Although application of these products is relatively easy, some brands are objectionable to patients because of the rough feeling of the varnish on tooth surfaces and the unsightly appearance of some brands. Fortunately, the varnishes wear off the tooth surfaces in a short time. For patients with minimal dental caries needs, the currently most popular and recommended treatment is 5% sodium fluoride varnish applied during routine recall appointments.
You can easily identify the many patients in your practice who need caries preventive treatments stronger than conventional topical fluoride or fluoride varnish. For stronger preventive therapy, there is a controversy about whether to use 1.1% neutral sodium fluoride containing 5,000 ppm fluoride (the most popular of which is PreviDent® from Colgate®) or remineralizing pastes (the most popular of which is MI Paste from GC America). More data is needed to compare these two methods, but I will give you with my observations and current opinions on their comparative use.
1.1% neutral sodium fluoride
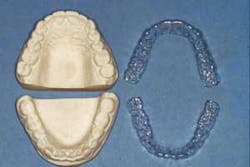
For several decades, 1.1% neutral sodium fluoride, 5000 ppm fluoride as a brush-on, or used in trays (see Figure 2), has been used effectively for several decades for extreme caries potential patients, such as radiation therapy patients. I have used it on many potential high caries patients with successful reduction of caries and/or elimination of new caries. Positive research is replete on the effectiveness of this concept, especially when applied daily in trays for five minutes. It is still my first choice for patients with a high potential for developing caries.
Calcium phosphate and fluoride
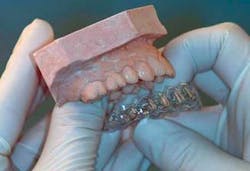
However, amorphous calcium phosphate, augmented with nearly 1,000 ppm fluoride (MI paste from GC America) is growing in popularity and research support.This material may be used in trays (Figures 3 and 4) or merely rubbed on the surface of the teeth. The longer the material stays on the teeth within reason, the better the result. At least a few minutes of application should be used. The material is not objectionable for patients. Some dentists are using 5,000 ppm fluoride in trays for two or three months, followed by use of MI paste after that time. Other clinicians are using the reverse order, and still others are using one or the other technique only. The choice is up to you until more comparative research is available.
Dr. Christensen is a practicing prosthodontist in Provo, Utah, and Dean of the Scottsdale Center for Dentistry. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of Clinicians Report (formerly Clinical Research Associates), which since 1976 has conducted research in all areas of dentistry and publishes its findings to the dental profession in the "Gordon J. Christensen Clinicians Report" monthly newsletter. He is an adjunct professor at Brigham Young University and the University of Utah. Dr. Christensen has educational videos and hands-on courses on the above topics available through Practical Clinical Courses. Call (800) 223-6569 or (801) 226-6569.