Ask Dr. Christensen
by Gordon J. Christensen, DDS, MSD, PhD
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an e-mail to [email protected].
For more on this topic, go to www.dentaleconomics.com and search using the following key words: endodontics, posts, tensile load, occlusion, crown-down concept, bruxism, partial dentures, tooth structure, Dr. Gordon Christensen.
Q There seems to be a significant amount of disagreement on when to place a post in an endodontically treated tooth, or even if a post should be placed at all. Further controversy centers around what type of post should be used when it is indicated. What are your opinions on this subject based on your experience?A Many teeth are treated endodontically, and judgments are often difficult to make relative to placing or not placing posts. As with almost any subject, I could list studies to support both sides of the question. Therefore, I will attempt to answer your question based not only on the myriad, mostly in-vitro, research projects, but on my own experience as a prosthodontist. I have placed thousands of units of crowns and fixed prostheses, and I have seen successes and failures of post placements.Most of the research projects on posts in endodontically treated teeth have been done in a laboratory where the investigators consider the amount of remaining tooth structure and the resistance of the post to tensile load intended to pull the post out of the tooth. In my opinion, these studies are interesting and somewhat useful; however, they address only some of the challenges faced with endodontically treated teeth.
In this column, I will discuss the need for posts based not only on the amount of tooth remaining in the endodontically treated tooth, but also on the type of occlusion, occlusal pathologic conditions present, expected load during chewing, and other factors. Some readers will disagree with my suggestions; however, my clinical experience has shown some endodontically treated teeth with significant tooth structure remaining break off at the gum line when subjected to significant occlusal load.
This discussion assumes that a minimal access hole has been cut in the tooth for endodontic treatment. It all assumes that the “crown-down” concept has not been done to an extreme, as this removes a significant amount of root structure, leaving less tooth structure than desirable.
Each individual factor must be considered with the other factors discussed to make a legitimate decision about whether or not to place a post in an endodontically treated tooth.
Amount of tooth structure remaining
Most studies have dealt with the characteristics of the endodontically treated tooth and have not considered other factors. The consensus of research opinion, combined with my own opinions, concludes with the following observations:
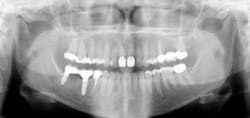
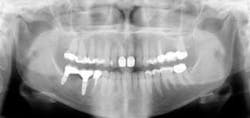
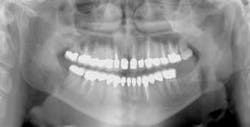
The preceding characteristics are often negated when some other conditions are considered. The factors described in the following discussion may override apparently adequate tooth structure remaining and indicate post placement is required (see Figs. 1 and 2).
Canine rise present
If the tooth is a posterior tooth in a patient with a canine rise present and if one-half or more of the coronal tooth structure is remaining, a post is not indicated. In such situations, the canine tooth assumes the lateral forces of occlusion and forces were applied in a straight-down vertical direction to the endodontically treated tooth.
If the endodontically treated tooth is the canine — and that tooth assumes the lateral load of the occlusion alone — my opinion is that a post is indicated in almost any situation, regardless of the amount of remaining tooth structure.
Incisal guidance present
Almost all people have incisal guidance in their occlusal movements. If the anterior endodontically treated tooth is in a full complement of anterior teeth, has minimal tooth structure removed, and the endo access hole is the only missing tooth structure, a post is not indicated because all of the anterior teeth share the incising load.
If the endodontically treated tooth is an anterior tooth which, as determined by appropriate occlusal evaluating methods, assumes a significant amount of the anterior forces when the patient moves the jaw into an incising position and a significant portion of the coronal tooth structure is missing, that tooth should probably have a post.
If several anterior teeth are missing and the endodontically treated tooth is one of the only remaining teeth assuming forces in the incising position, it should have a post. There are only a few clinical situations in which the anterior teeth do not have significant lateral forces when incising. An example is a Class III, end-to-end, occlusal relationship. In these situations, the forces are primarily in a vertical direction and posts are usually unnecessary depending on the amount of tooth structure remaining.
Group function occlusion
In the minority of patients, especially elderly ones, most or all of the teeth occlude when the patient moves the mandible into a lateral position. In such patients, the occlusal load is directed in a lateral location when they chew. I suggest that unless most of the coronal tooth structure is remaining in an endodontically treated tooth, a post should be placed.
Bruxers
A significant portion of adults have a bruxing habit. It has been estimated to affect at least one-third of the population. These people have enormous lateral forces on their teeth. Unless the endodontically treated teeth have most of the coronal tooth structure remaining, I suggest that posts are indicated.
Abutments for fixed partial dentures
In strength tests we have accomplished on extracted endodontically treated teeth, the lateral forces required to break the coronal portion of teeth from the root portions vary significantly between teeth with posts and teeth without posts. The teeth with posts are much stronger when subjected to lateral forces.
Teeth used as fixed partial denture abutments are required to support the forces of occlusion not only for themselves, but also for the missing teeth replaced by pontics. In my opinion, when an endodontically treated tooth is serving as an abutment for a fixed partial denture, it should have a post.
The fixed partial denture situation brings up another clinical dilemma. If a vital abutment tooth has only a small amount of tooth structure remaining, should it be treated endodontically and receive a post, or should it be left alive, built up with adhesives, potentially pins, and build-up materials?
My experience and research have shown that a properly endodontically treated tooth with minimal coronal tooth structure remaining will serve more effectively as an abutment than the same vital tooth with just a build-up in it.
Removable partial denture abutments
The occlusal stress and forces on removable partial denture abutments require optimum strength. In my opinion, placement of posts in such endodontically treated teeth is an appropriate treatment.
What type of post is best?
The post concept has evolved from custom-cast posts to prefabricated stainless steel posts, to titanium or titanium alloy posts, to fiber-reinforced resin-based composites.
Currently in the U.S., fiber-reinforced resin-based composite posts are used by the majority of dentists. The advantages of these posts are well known. The primary advantage is the flexibility of the posts, which reduces vertical cracking of the endodontically treated tooth in the event of a blow to the tooth or aggressive chewing. These posts can be placed easily and rapidly.
If post removal is needed, these posts can be removed easily with a tapered diamond bur. It appears that until better types of posts are developed, the fiber-reinforced resin-based composite post will be the favored one.
Another complication!
You may be doing your own endodontic therapy, controlling the size of the access hole and the amount of “crown down” tooth-cutting. If so, don't overdo the “ice cream cone” shaping of the root canal(s).
Often, the opening is so large into the pulp chamber that the canals that build up the tooth with a post and core still create a very weak restoration. Leave as much tooth structure as possible.
The preceding information has been a long answer to your multifaceted question. However, the question is not a simple one, nor is it really proven by the literature.
In summary, there are numerous factors relating to the need for a post other than the amount of tooth structure remaining. I hope that my blending of research with clinical observations has been useful for you.
Two of our PCC videos that relate directly to your question are:
V1931 — “Complex Oral Rehabilitation”
V1908 — “The Best Posts, Cores, and Build-Up Techniques”
For more information, visit online at www.pccdental.com or call (800) 223-6569.
Dr. Christensen is a practicing prosthodontist in Provo, Utah, and dean of the Scottsdale Center for Dentistry. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of CLINICIANS REPORT (formerly Clinical Research Associates), which since 1976 has conducted research in all areas of dentistry.