A time to rebuild and a time to forsake
Timothy M. Bizga, DDS, FAGD
At some point, you’ve likely encountered the saying “cut and run.” The saying has its origins in nautical vernacular, with a meaning similar to the phrase “bail out.” It was used in times of imminent danger, when the captain of a ship would make the difficult, irreversible decision to cut away the anchor. The order to cut and run was never given lightly; it meant that the situation was perilous, the future was uncertain, and no other solution existed.
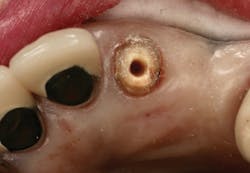
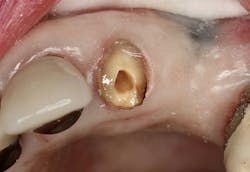
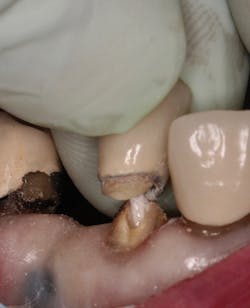
Figure 1: Occlusal image of finished root canal prep after gutta-percha removal
We as dentists must also navigate uncertain conditions chairside. We face difficult decisions when we perform new patient exams. When looking at each tooth we must ask, “What should I do here? Should I monitor or refurbish? Repair or rebuild? Replace or forsake?” We must decide, “Should I get involved here, or should I cut and run?”
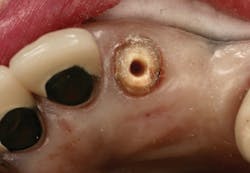
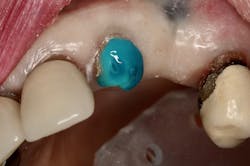
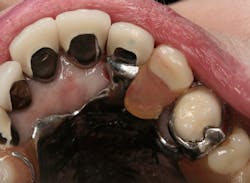
Figure 2: Intaglio surface of existing PFM retrofit preparation
Sometimes this process is black and white. Other times it’s a vast sea of gray. We are often confronted with endless no-win scenarios, ones that have a reverberating and lasting effect on our patients’ well-being. What helps to focus the mind and streamline the decision-making process is a simple question to ask: “Will this procedure leave my patient better off than when I found him/her?”
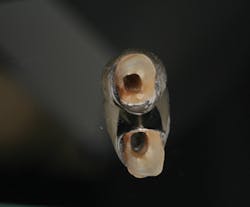
Figure 3: Rebilda Post GT system
The decision to rebuild or forsake is often associated with endodontically treated teeth. We know today that long-term success rates for endodontically treated teeth hinge on the type, timing, and quality of our restorations.1 And while tradition has solidified the belief that all endodontically treated teeth need posts prior to placement of final restorations,2 more recent studies have shown that the likelihood of survival for pulpless teeth is directly related to the quality and quantity of remaining tooth structure.3,4 As a result, dentists have embraced new approaches to these situations. For example, clinicians have begun to favor bonded restorative options that offer advantages that conventional modalities cannot.5
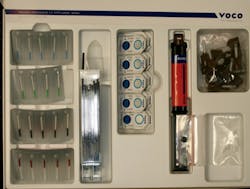
Figure 4: Rebilda Post
The philosophy of how torestore endodontically treated teeth and the criteria for post placement have changed. We must unlearn what we have learned. We understand today that fewer posts are indicated, and the ones that are placed should be smaller. Let us look at a case study that demonstrates this point.
Case study
An 80-year-old female patient presented for emergency treatment. Her health history was noted to be unremarkable apart from taking a low-dose aspirin as recommended by her primary care physician. The reason for her visit was that tooth No. 10, which had been previously restored with a porcelain-fused-to-metal (PFM) crown, was horizontally fractured off just below the finished margins of the crown preparation. The patient reported that it happened while eating. To complicate matters, No. 10’s crown had provided a necessary lingual rest and guide plane for retention of her existing Kennedy Class IIImaxillary partial. The patient expressed the desire to save the tooth if possible to avoid having to “scrap an otherwise good-fitting and functioning partial.”
Figure 5: Post bundle
Several restorative options were considered. The patient elected to have the tooth rebuilt in an attempt to preserve the existing partial and minimize cost.
The plan was to restore No. 10 as follows:
- Endodontically treat No. 10 due to exposure of a calcified pulp chamber
- Preserve the existing tooth structure to reduce further weakening to the root system
- Retrofit and bond the existing crown to the root using a post system
Figure 6: Dry fit post try-in
The root canal on No. 10 was completed using the WaveOne Gold system (Dentsply Sirona). Upon completed obturation, care was taken to remove only excess gutta percha from the canal using a warmed endodontic plugger. Removal extended approximately 4 mm to 5 mm into the canal space (figure 1).
The intaglio surface of the PFM crown contained the preexisting dentin core preparation. The decision was made to prepare the surface to receive the intraoral portion of the post rather than completely remove the remaining dentin (figure 2). This was done to facilitate a smooth retrofit between the remaining root structure and intaglio crown surface as well as to maximize bonding surface area between segments.
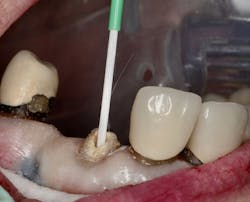
Figure 7: Acid total-etch treatment of tooth No. 10
For this case, the Rebilda Post GT System (Voco) was used (figures 3 and 4). The material consists of a series of fine glass fiber–reinforced posts that are bundled together inside a color-coded sleeve. As these posts were cemented, the sleeve was removed prior to light polymerization of the core material. This allowed the spreading out of the fibers within the core material as the case demanded (figure 5). Green-sleeve posts, which bundle nine fine posts that are 1.2 mm in diameter collectively, were selected. They were tried in to verify a passive fit (figure 6).
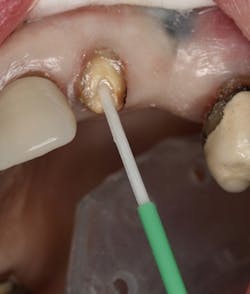
Figure 8: Adhesive application
A total-etch technique was used on the remaining root (figure 7). Futurabond U (Voco) adhesive was applied to the canal space and left uncured (figure 8). RebildaDC (Voco)core build-up material/cement was injected into the canal only. A green-sleeve bundle of fine glass fiber–reinforced posts was prepared and inserted into the canal (figure 9). This decision was made to inversely spread the posts within the canal space to maximize retention and add strength to the core within the root. (For clarity, I have demonstrated this distribution pattern in Figure 10 using plastic straws and a glass.) The materials were then uniformly cured according to manufacturer’s specifications using a Valo Grand(Ultradent Products) curing light (figure 11).
Figure 9: Post placed into
uncured Rebilda DC
The excess of the posts was trimmed without water, and the existing crown was then tried in to verify precise fit (figure 12). Once passive fit over the cut post bundle was verified, the intaglio surface of the crown was acid-etched, rinsed, and dried.
Figure 10: Straw simulation of inverse post distributions within tooth
FuturabondUadhesive was applied and cured. The intaglio surface of the crown was filled with Rebilda DC cement, which was also used to “buttercoat” the root surface and cut the post bundle. The two segments were then joined and resin-bonded together by using a curing light and waiting the manufacturer-specified time for the dual-cure polymerization reaction to complete (figure 13). The excess cement was removed and the margins checked for any gaps.
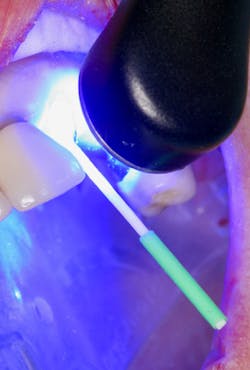
Figure 11: Curing step using Valo Grand
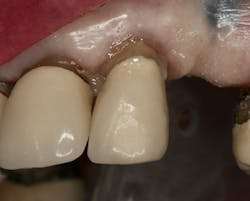
The existing partial was then tried in to verify proper relation to rest seats and guide planes (figure 14).
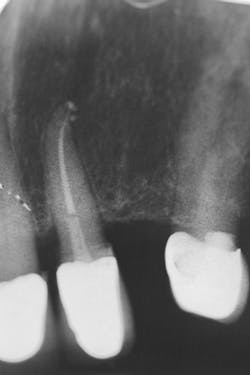
A final x-ray was taken for records (figure 15). The post was homogeneously connected, ran between the existing root and the newly reattached PFM crown, and provided for a strong rebuild.
Figure 12: Try-in of PFM crown retrofit after posts were cut to desired length
Conclusion
The purpose of a post is to keep the core in place, especially against compressive strength, and to distribute stress along the long axis of the tooth.6,7 The ideal post needs to be elastic enough to follow the natural flexural movements of the tooth structure.
Figure 13: Crown seat resin-bonding together the two segments (root and crown)
Glass-fiber posts have been shown in laboratory tests to exhibit a modulus of elasticity that is extremely similar to that of natural dentin.8 In my opinion, this key physical property makes glass-fiber posts the best option for retention of a core in endodontically treated teeth that require post placement.
Figure 14: Flush and precise fit with existing partial
Whether treating routine cases or atypical ones, the toughest decisions are the permanent ones. When faced with the decision to rebuild or forsake, having more options affords us more opportunities to rebuild and better serve our patients.
Figure 15: Final x-ray
References
1. Eliyas S, Jalili J, Martin N. Restoration of the root canal treated tooth. Brit Dent J. 2015;218(2):53-62.
2. Weine FS. Endodontic Therapy. 2nd ed. St. Louis, MO: C.V. Mosby Co.; 1976.
3. Assif D, Gorfil C. Biomechanical considerations in restoring endodontically treated teeth. J Prosthet Dent. 1994;71(6):565-567.
4. Gutmann JL. The dentin-root complex: anatomic and biologic considerations in restoring endodontically treated teeth. J Prosthet Dent. 1992;67(4):458-467.
5. Sorrentino R, Monticelli F, Goracci C, Zarone F, Tay FR, Ferrari M. Effect of post and core restorations on the resistance to fracture of endodontically treated maxillary premolars in different restorative systems. Am J Dent. 2007;20(4):269-274.
6. Guzy GE, Nicholls JI. In vitro comparison of intact endodontically treated teeth with and without endo-post reinforcement. J Prosthet Dent. 1979;42(1):39-44.
7. Asmussen E, Peutzfeldt A, Heitmann T. Stiffness, elastic limit, and strength of newer types of endodontic posts. J Dent. 1999;27(4):275-278.
8. Maceri F, Martignoni M, Vairo G. Optimal mechanical design of anatomical post-systems for endodontic restoration. Comput Methods Biomech Biomed Engin. 2009;129(1):59-71.
Timothy M. BizgA, DDS, FAGD, received his dental degree from the University of Michigan School of Dentistry. He is a former chairside assistant and lab technician, giving him a unique perspective in his understanding of dentistry. He practices today as a general dentist in Cleveland, Ohio.
Disclosure: Dr. Bizga received compensation from Voco for the authoring of the article.