Ask Dr. Christensen
Gordon J. Christensen, DDS, MSD, PhD
Q The use of implants in the anterior portion of the mouth has been a wonderful concept for the profession and the patients we serve. When the implants are placed in optimum locations, I have no difficulty making the prosthesis or crowns adequate from an esthetic standpoint. However, I frequently find that the esthetic appearance of crowns and/or fixed prostheses is compromised due to the lack of adequate gingival tissue around the implants to simulate normal anatomy when the patient smiles. Even more frequently, I find that the inadequate angulation of the potential implant abutments makes esthetic restoration of the implants almost impossible. What do you suggest for these cases?A I regularly hear questions such as yours. In my opinion, it is one of the frustrating outcomes often related to one practitioner placing the implants and another one restoring the implants. When an experienced practitioner accomplishes both implant placement and restoration, he or she can decide to graft or not graft bone or soft tissue before the implants are placed, thus reducing the occurrence of this unfortunate situation. Nevertheless, it still occurs on a routine basis.In situations where the implants have been placed and the gingival tissue coverage is inadequate for optimum esthetic appearance, or where the implants are at difficult angles, I have a few suggestions for you.
The first thing I would do is give the patient a hand mirror and have the person hold it at arm’s length. Have the patient smile as high as is possible. Note the display of teeth, implants, and gingival tissues. I suggest taking a photo or making a drawing to record the location of the lips in relation to the teeth, implants, and gingival tissues.
Now, have the patient speak several sentences that have an “s” sound in them. This will display the teeth, implants, and gingiva on the mandibular arch. Complete your drawing or take another photo, showing the location of the lips in relation to the teeth, implants, and gingiva on the mandibular arch during speech. The older the patient, the greater his or her teeth, implants, and gingiva on the lower arch will display during speech.
There are only a few alternatives for patients with the challenges you described, and often patients do not want any of them.
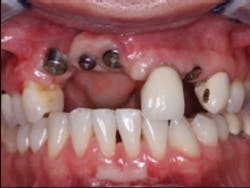
FIG. 1 — Referred patient upon entry into our prosthodontic practice.
Most often, the defects are on the maxillary arch. If the patient does not smile high enough to show the normal location of the gingival tissues, the restorative options are better. However, some patients will not accept the display of unesthetic restorations, even though they do not show the unesthetic portion of their restorations during normal smiling or talking.
The same treatment planning approach is also an appropriate suggestion while planning for restorations on the mandibular arch. Fortunately, some patients will accept a normal looking smile and the normal appearance of the lower restoration during speech without complaining about the unesthetic restorations that show when the lips are stretched away from the prosthesis or crowns.
I suggest simulating the completed esthetic situation you expect to be present in the specific situation either with wax in the mouth or on a model of the patient’s mouth. Computer simulation is also an excellent way to show the patient what to expect, but only a few dentists have this capability in their practices. Let the patient see the potential restorative situation and discuss it with you. This conversation will help you make a decision about the restorative treatment.
One of the alternatives for this dilemma is to graft bone and/or soft tissue into the defective areas around the implants. However, after the implants have been placed, grafting is far more difficult and unpredictable than grafting before the implants were placed. Ideally, grafting should be accomplished before implant placement.
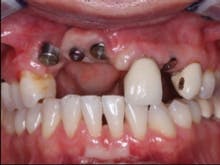
FIG. 2 — Impression copings in place showing lack of adequate gingiva and bone, as well as difficult angulation of implant placement.
FIG. 3 — Custom “open” tray made from DENTSPLY Triad light-curing material.
Grafting may not be a viable alternative because of the complexity and unpredictability of the grafting, the patient’s lack of acceptance of the grafting, or the patient’s inability to pay for another surgical procedure.
I will use a recent case, which has the conditions you described, to show my suggestions to you. A competent surgical specialist who had very few optimum clinical conditions present when placing the implants sent me this case (Fig. 1).
In my opinion, when the implants have been placed in positions that make the prosthodontic treatment difficult, custom abutments are almost always necessary (Fig. 2). As you observe the angulation of the impression copings, it is evident that the implants are approximately 45 degrees from optimum placement angulation. The practitioner placing these implants had to either place them at the angulations that are evident, or graft significant bone into the potential implant locations before placing the implants. I feel that the decision not to graft was appropriate, assuming that the lab technician making the prosthesis is highly competent. This much angulation deviation often makes splinting the crowns together the most advisable treatment, since forces on the implants will be at angles not in line with the long axis of the implants, and any additional strength that can be obtained in the prosthesis is certainly advisable.
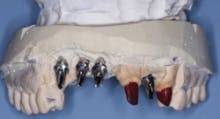
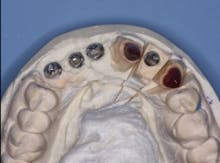
FIG. 4 — Custom cast abutments showing compensation for difficult angulation of implant placement.
Using a custom impression tray is the most appropriate method for cases as difficult as the one shown (Fig. 3). Stock trays compromise the practitioner’s ability to make an optimum impression in such situations. I prefer to use light curing tray material. Such material allows the fabrication of any desired tray configuration. An “open” tray design allows the unscrewing of the impression copings before removing the impression from the mouth, optimizing the accuracy of the impression.
FIG. 5 — Incisal view showing proper angulation of abutments.
Fig. 4 shows the parallelism of the three custom cast metal abutments on the patient’s maxillary right anterior area. These three abutments will be splinted together with a three-unit prosthesis. The prosthesis will be cemented with provisional cement (Premier Implant Cement). The cement will be placed only on the most apical third of each abutment when they are cemented to allow subsequent removal of the prosthesis in the event of loose screws or other challenges. Designing abutments to allow space for an optimum esthetic result demands communication between the dentist and lab technician. Fig. 5 demonstrates the homogeneous potential thickness of the subsequent restorations to be placed.
FIG. 6 — Abutments in the mouth.
The abutments shown in the mouth make clear the significant bone loss in this patient and demonstrate the inadvisability of attempting to graft bone in the patient after the implants have been placed (Fig. 6). Could grafting have been done before the implants were placed or at the same time the implants were placed? That is difficult to determine at this time, but it can easily be noted that if grafting had been done, it would have required a large amount of bone. If socket grafting had been done when the teeth were originally extracted, would the defect have been as large? It is impossible to determine, but socket grafting usually minimizes bone loss during healing.
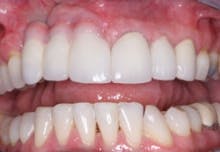
FIG. 7 — Finished restorative treatment.
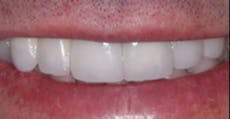
When the lips of this patient are retracted, the esthetic result is unacceptable (Fig. 7). However, when the patient smiles as high as he can, the result is optimal, and he is very satisfied with his treatment (Fig. 8).
FIG. 8 — Retracted lips and patient’s smile.
In summary, each case is different. If a significant bone defect is present when implants are being considered, and the patient will accept grafting, that procedure is advisable. If the smile line or display of mandibular teeth or crowns is not objectionable, placement of gingival colored ceramic on the prosthesis can be a highly acceptable and predictable technique.
Dr. Christensen is a practicing prosthodontist in Provo, Utah. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of CLINICIANS REPORT (formerly Clinical Research Associates).
We have some excellent educational materials that are directly related to this topic, and they will help you make decisions when implants are placed at difficult angles and bone and gingiva are inadequate.
Video 4350, Socket Preservation and Bone Grafting, shows how truly simple bone preservation can be when simple, easily placed materials are used.
Video 4346, Easy Crown Lengthening, shows how to reposition gingival tissues when more restoration retention is needed or unesthetic gingival conditions exist.
Our courses, Rehabilitative Dentistry and Occlusion, and Successful, Real-World Practice – Fixed Prosthodontics, discuss and demonstrate many clinical situations similar to the one described in this article, and simplify this seemingly difficult procedure. Go to www.pccdental.com or call (800) 223-6569 for information.
Past DE Issues