CBCT: The virtual surgery in endodontic diagnosis
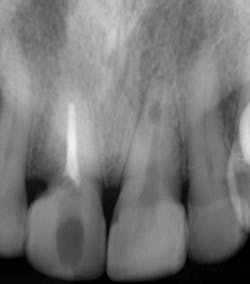
Fig. 1 — Preoperative radiograph demonstrating an internal resorptive defect in the apical third of the root in tooth No. 9. Note the cervical resorptive lesion in tooth No. 8.
It has been 20 years since the surgical operating microscope (SOM) made its debut in the endodontic armamentarium. At the time it was greeted with the same skepticism and misgivings that heralded the introduction of this instrument into the neurosurgical arena. Seasoned surgeons scoffed at the insinuation that their performance could be enhanced with improved magnification and illumination, and resisted accepting the new technology. It took the younger residents to embrace this new concept, having been introduced to it during their training. The residents then became the new mentors to the next generation of neurosurgeons.
This pathway to acceptance of the SOM in endodontics mirrored neurosurgery. What was once thought of as a “very expensive video camera” has now proven itself indispensible in contemporary practice.
The increase in magnification revealed a dimension that both awed and humbled the most experienced practitioner, and raised expectations as to what could now be achieved via conservative treatments. The only shortcoming to this process was the reliance on a two-dimensional image to formulate a three-dimensional treatment plan.
Often the patient’s complaint and presentation were not matched with the appropriate radiographic representation, confounding the diagnosis and complicating subsequent treatment decisions. In extreme instances, invasive procedures were employed to “explore,” via direct visualization, the areas in question in the hope of discovering the definitive etiology.
These earlier units produced a large field of view (FOV) and a low-resolution scan, but contemporary models offer a smaller FOV (as small as 50 mm x 38 mm) with slice thicknesses of .076µ. Unlike their medical CT counterparts, CBCT volumes are isotropic or cuboidal, enabling accurate rendering and measurement algorithms.
The most pivotal feature, however, is the ability to render a perspective view of an area of concern from three main directions and, through axes alterations, an infinite number of diagnostic views. This technology allows us to perform “Virtual Surgery”© on the displayed image, narrowing our focus and streamlining the decision tree for diagnosis and treatment. The feasibility of a re-treatment is more accurately ascertained without the invasiveness of clinical disassembly, sparing both the patient and practitioner undue time and expense.
Pathology not readily apparent on conventional radiographs is defined with remarkable clarity because its presence is not camouflaged by bone thickness or overlying structures. A recent study reported that the CBCT showed 34% more lesions than conventional radiographs of the same site. Incipient disturbances in the periodontal ligament space can often be demonstrated because the slice thicknesses are one-half the dimension of the PDL (0.2 mm).
This aspect is instrumental in diagnosing vertical root fractures where the fracture line cannot be visualized, but its distinctive disruption of the ligament space is glaringly apparent. Additional applications include, but are not limited to:
- Diagnosis and assessment of iatrogenic complications — i.e., missed canal(s), perforations, separated instruments.
- Diagnosis and management of dentoalveolar traumatic injuries, especially root and alveolar process fractures.
- Localization, differentiation, and assessment of root resorptive processes.
- Assessment of root numbers, locations, and curvatures.
- Diagnosis of lesions of nonendodontic origin.
- Presurgical case assessment and planning.
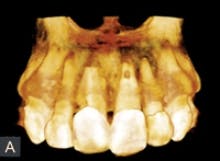
Fig. 3 — This 3-D rendered model is a representation of the bone loss and extent of the apical resorption in tooth No. 9. Note also the cervical root resorption of tooth No. 8.
It is nonparallel and diverse, unlike the medical CT, and is subject to adverse absorption and bending effects on the rendered image. This is of particular interest when assessing the integration of implants, where two closely placed fixtures may appear to have no bone between them. On a grander scale, fixed prosthetics will produce a sunburst or streaking effect at the level of the metal undercasting, again due to the scattering of the radiographic beam.
Finally, the spatial resolution of CBCT images at 0.4 mm to 0.076 mm (1.25 to 6.5 line pairs/mm) is inferior to conventional film-based (20 line pairs/mm) or digital (8 to 20 line pairs/mm). So although the technology has some advantages over the conventional radiographs, at this time it is not considered a reasonable or prudent substitute.
The hallmark of intelligent people is to never make the same mistake twice. When presenting this technology to my colleagues, I often wonder if we, as a specialty, will again postpone our acceptance of this valuable tool that seems tailor-made for our particular field. I believe I received my answer at a course on advanced cone beam navigation I recently attended; the majority of the attendee doctors were endodontists!.
Stephen P. Niemczyk, DMD, is the past director of the undergraduate and graduate endodontic programs at the University of Pennsylvania, and is currently the director of endodontic microsurgery at Harvard University and Albert Einstein MC. He is the founder of Endodontic Microsurgical Innovations, and is in full-time practice in Drexel Hill, Pa. He can be reached by email at [email protected]
Past DE Issues