HOW TO PROFIT from... Implants: The behavioral challenge
When many of us began doing implants, our biggest hurdle was the learning curve. Today we are more knowledgeable, but there is a lot to learn. Examples include planning, osseous considerations, sequencing, provisionalization, impressioning, bite registration, size of restoration, and splinting options. Dentists must master all these hurdles as the complexity progresses from a single posterior tooth to multiple posterior teeth, to a single anterior tooth to multiple anterior teeth, to a full arch and finally to two full arches. We’re thankful the learning curve for these is short. And we now have cumulative knowledge and hardware support that were unavailable a decade ago.
Now implants can provide profit potential in restorative dentistry. Most of the time - when properly planned - everything goes better with implants than with teeth. Impressions are easier, preparations are almost nonexistent, and some laboratory procedures are simpler with the analogues and waxing copings of many of the systems. My labs charge the same price for implant and tooth crowns when I provide the components.
I remember when I first got involved with external hex implants and the only connections were with screw-retained “parts.” I showed Dr. Irwin Becker, education chairman at The Pankey Institute, an articulator with all of the analogues, abutments, and screws. We talked about how much it reminded us of the toy erector sets of our youth. He said to me, “Someone is going to make it so that we can someday treat implants like teeth, with existing crown and bridge procedures.” Irwin, you were right.
Our challenge
If the greatest challenge today isn’t the profitability of implants or the mastery of technology, what is? For many, it is the change to interactive communication - the way we listen and converse with patients in hopes of moving them toward case acceptance. For this reason, I will attempt to plant some thoughts that could grow into successful, proactive behaviors.
My typical patient who benefits from implant restorations has heard that implants aren’t always successful. Achieving implants isn’t well understood by most patients, who are already concerned about the pain, time, and cost of implants. The old fear factor acts as an obstacle to opportunity for predictable, optimal results.
At The Pankey Institute, we focus on successful behaviors to build trust and overcome fear. These behaviors can become second nature with proactive practice and help implant candidates select the optimal dentistry they deserve.
Beginning conversations
Years ago, when Dr. L.D. Pankey gave his philosophy seminars, he told dentists about his habit of helping patients understand the status of their dental conditions on a time line. He used to say, “You have a chronological age, and you have a dental age, and the two can be independent.” He explained that each person is a youth, adult, or elder chronologically but can be any of the three in a dental sense, depending on oral health. Then he related what was going on in a patient’s mouth to what was going on in his or her whole body, explaining that dental health is a barometer to general health. Knowing what we do about the link between periodontal disease and medical conditions, I’m amazed that he spoke of this with his patients as early as the 1940s.
I look to the past because the concepts Dr. Pankey conveyed to his patients are timeless and have helped me win case acceptance many times. He thought that if you had all your teeth and your gums were in good condition with a good bite, you were in the youthful third of the continuum. Those falling into this third could be those with deciduous teeth, mixed dentition, or a full complement of properly meeting, permanent teeth.
If you had unrestored decay, the beginnings of periodontal disease, or both, you were in the adult phase. Once you lost your first tooth, you crossed over the middle age in the adult phase and could never regain youthfulness - although you could get to young adulthood by taking care of any periodontal disease and having a fixed bridge to replace the missing tooth.
More unrestored or missing teeth, progressing periodontal disease, or both led to later adulthood. With the first edentulous posterior quadrant (where there were no remaining molars), you entered the elder phase of dental age. Progressive tooth loss and possible restoration with free-end saddle partial dentures led to what Dr. Pankey called later elderhood. He called complete edentulism “dental death.”
I remember hearing him say, “Once you lose your first tooth, you can never cross back over the line.” He illustrated this to patients by drawing a rectangle separated into three parts. He broke down the compartments further into the aforementioned parts. Then he made a powerful gesture. He took his pencil and illustrated where each patient was on this continuum dentally and related it to the patient’s chronological age. He said something such as, “Mrs. Debakiay, you are an adult woman of 57, and isn’t it nice that your dental condition is of someone who would be a young adult!” Or if the situation warranted, he pointed out that although the patient was a young adult, his or her dentition was that of a middle-aged or elder person.
Back then - just as today - people wanted to be more youthful. With the advent of root-form implants, you can regain youthfulness after losing teeth. Although Dr. Pankey never saw the successes of today’s dental implants, he did see the beginning of implants and looked forward to optimally replacing natural teeth. Using his timeless model of dental age vs. chronological age, we can help patients understand their dental ages, then share with them the opportunity to return from dental death or old adulthood back to dental youthfulness using today’s methods and materials.
We’ve even begun to feel confident in recommending that when there are questionable teeth in the way - ones that may jeopardize the success of a restoration - they should be extracted in favor of an implant that would provide a better prognosis. This concept should be likened to and understood as efficaciously as strategic extractions of periodontally hopeless teeth.
Once a dentist becomes familiar with implants and uses them as a regular part of the armamentarium in restorative dentistry, it is difficult to harness his or her enthusiasm. Schedule time for a pre-clinical experience prior to each clinical exam. During the pre-clinical interview, spend a few minutes getting to know each other. As you ask questions and try to understand the patient’s expectations, you’re doing most of the listening. Don’t forget to ask one of the most important questions: “How do you feel about a removable replacement for your missing teeth?” The answer often leads directly to a conversation about the success of implant restorations, and you can dispel misconceptions that implants aren’t predictable or fully successful.
Earning the patient’s trust
When discussing optimal treatment during phases of treatment - and even after completing treatment - remind patients about their oral conditions prior to restoration. Provide them with photos. Reviewing before and after photos at the completion of treatment is a time for celebration.
We make a complete set of intraoral photographs during the clinical phase of the patient’s initial visit. It builds a sense of choice and responsibility within the patient when I request his or her permission to make the photographs as well as necessary radiographs and appropriate diagnostic models during the clinical-exam phase. During the imaging and impression process, I explain the utility of these items in diagnosing and planning treatment. I let the patient know I’ll study the images and models and thoughtfully prepare my findings prior to our meeting again to discuss treatment options. I also tell them that I might discuss my findings with specialists prior to our meeting. I routinely defer giving any diagnosis until I have had time to study patients’ situations.
During the subsequent treatment conference visit, my patient learns that we have scheduled ample time for discussion and treatment options. It is most helpful and in the patient’s best interest to explain all procedures so the patient knows what will be done if he or she chooses the treatment. It is also best to discuss how long the restorative process will take, costs, and how the patient will likely feel after each procedure. Failure to have a conversation about these things upfront commonly results in the patient going home with hanging questions, and this slows the decision process.
Then, if warranted, I ask my patient for permission to arrange an examination and consultation with one or more specialists before we develop a definitive plan. When appropriate, I arrange for my patient and myself to meet with my specialists. A comfortable arrangement usually can be found for all involved, and this increases the trust and comfort level of the patient facing interdisciplinary treatment. In addition, an interdisciplinary meeting with the patient usually removes any remaining emotional obstacle to treatment.
The virtue of patience
Many times it takes patients months to work through what is most appropriate for them. What is your role? It isn’t to shrug your shoulders and mutter, “Not going to happen.”
The patient’s implant restoration decision involves his or her understanding of the restorative process, trust in the dentist and any specialists involved in the process, desire for the benefits to be gained, and understanding of the alternatives and comparative potential downsides of them. Oftentimes, financial planning is a part of the process, and most likely, so is overcoming emotional obstacles such as dental anxiety. Over time and with your guidance, the patient should rationally decide that the benefits outweigh the costs, including any potential health risks and discomfort.
Profiting from implant dentistry requires educating the patient - sometimes more than once - staying in relationship with the patient, and engaging the patient in multiple conferences on the subject if needed. Create opportunities for conversation. Invite the patient to talk about feelings relative to the treatment decision.
Then, listen actively for signs of what more information or assurance the patient needs to work through the decision. Encourage the patient to restate what you said to ensure he or she understands everything correctly. Allow the patient to grow in trust and acceptance of what is in his or her best interest while you remain concerned about his or her oral health. Be patient. Remember, these are complex issues to a patient and the patient’s need to sleep on it or request more information isn’t a “no,” only a “not yet.”
The right choices
Today’s dental consumers are much more educated as a result of greater access to information, as well as their seemingly greater desire to attain or maintain maximum health. They have input from friends, lay magazines, the Internet, and direct marketing by many health care product manufacturers. They speak openly and often with one another about their treatment options. They are more likely than not to be aware of the options available to them and to want multiple opinions.
Only through a thorough discovery process involving them can we assist them in obtaining desired outcomes with appropriate means. Each person who comes to us has chosen us. They come to us with individual lives, temperaments, and objectives (which they might or might not have well defined). By careful investigation of the existing conditions and by a clear explanation of these, we facilitate optimal choices.
Longevity and stability have been cornerstones of what I try to provide with my dentistry. I first heard of these two goals from Dr. Peter Dawson in his Concepts of Complete Dentistry courses in the 1970s. When incorporated appropriately into comprehensive care, implants are integral parts of restorative dentistry that allow for a level of success that, in many cases, could not be reached otherwise.
When my father was still in business, he displayed a sign over the entryway that said, “Through these doors pass the finest people on Earth - my customers.” When I advise my patients and assist them with their treatment decisions, I remember that sign. The one person I’m helping at the moment is the most important person at that moment and deserves the best dentistry has to offer. Today, the best that restorative dentistry has to offer includes consideration and utilization of implants.
Barry S. Segal, DDS, is a restorative dentist who treats implants in Aventura, Fla. He is on the visiting faculty of The Pankey Institute, a member of the American Academy of Restorative Dentistry and American Academy of Fixed Prosthodontics, and a Fellow of the American College of Dentists and International College of Dentists. Reach him at (305) 933-9911.
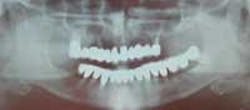
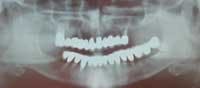
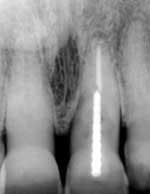
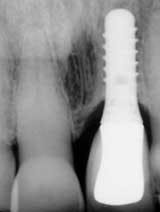
REVIEWING case photos and radiographs …
… communicates how far patients have come with implant TREATMENT.
Radiograph of 71-year-old woman before and after implant restoration
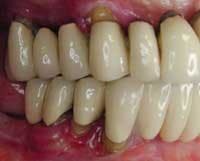
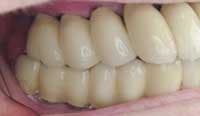
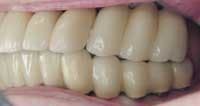
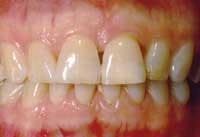
Photos of same woman before treatment
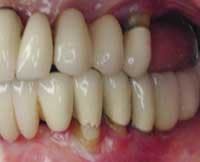
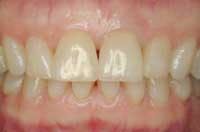
Photos of same woman after implant restoration
The case above is an excellent example in which someone who experiences continued periodontal breakdown around teeth despite treatment will fare better with implants and resist problems with future decay. Dr. Andrew Alpert of Aventura, Fla., placed the implants.
To help a patient understand the benefits of implant restoration, show before and after images of another patient and talk about the stability and improved esthetics achieved.
null
Before and after photos of the same patient.
Functional stability, health, and youthful appearance were achieved with the single implant.
The surgeon who placed the implant is Dr. Leonard Garfinkel of Aventura, Fla.