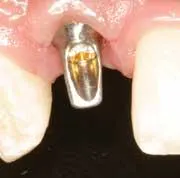
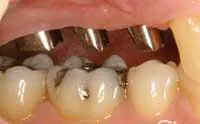
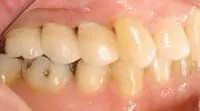
HOW TO PROFIT from... Implants: Who benefits from this treatment?
Do you immediately think of money and a financial gain when people mention the word “profit”? Webster’s New World Dictionary does not mention “financial gain obtained from the use of capital, or net income” as the first description of profit. The dictionary initially defines profit as “advantage; gain; benefit.” So, what benefits might we expect as we make implant-restorative dentistry a component of our practices?
Rule 1: Know your patients.
The replacement of missing teeth with implants should properly be considered complex treatment, and I believe most doctors would agree that it is wise to know the individual you are working with before complex treatment begins. While deep relationships cannot develop when we provide emergency care, once the emergency treatment has been delivered, the opportunity then exists for the doctor and the doctor’s team to learn more about the patient.
Every doctor progresses at his or her own pace, but understanding the patient’s needs and wants, discovering what the patient values in life, and developing a trusting relationship is necessary to be successful in treating complex situations. Once a trusting relationship has been established with the patient, then benefits will become apparent.
A satisfied patient will become the source of great joy to the doctor and the staff as they celebrate the completion of the implant-restorative treatment. The satisfied patient will most certainly refer new patients to the practice and profits abound in the form of 1) optimum comfort, function, and appearance for the patient, 2) patient confidence as they refer their friends and colleagues to your office, 3) increased professional prestige for the doctor and staff, and 4) financial gain for the practice as implant-related services increase.
Rule 2: The relationship between the restorative specialist and surgical specialist should be collaborative.
If the restorative doctor is not surgically minded, then relationships with surgeons will benefit as an increased number of patients are referred to the surgeons. As restorative and surgical specialists collaborate on behalf of the patients they serve, they will develop trust and confidence in one another and their desire to treat increasingly complex conditions will grow. Once again, patients profit as they gain the ability to function with comfort and confidence. Their self-esteem profits, as their appearance is more to their liking.
Rule 3: Before you begin, know yourself and obtain the requisite skills.
Depending upon the doctor’s temperament and style, there are numerous ways in which profit can be realized with implant-restorative treatment. Are you new to the profession with time available to spend on laboratory procedures? Are you a “controlling” person who likes to influence as many phases of treatment as possible? While in the office, do you prefer to spend the maximum time available with patients? Do you entrust the fabrication of all components of the implant-supported restoration to the laboratory specialist? Each of these individuals can develop systems that will ensure financial profitability and emotional satisfaction for the dentist as well as physical and emotional benefit to the patient.
Whether a doctor is new to implant/restorative dentistry or an experienced veteran, establishing efficient, simplified systems will improve the profitability of this phase of restorative dentistry. Initially, a doctor should become knowledgeable with the products and armamentarium of one or two implant companies. Developing familiarity with a system will take place after participating in a surgical or restorative hands-on course. Obtaining product catalogs and manuals and becoming comfortable with individual components will permit the doctor to work efficiently and confidently when the patient is in the chair. Knowledge of impression or indexing techniques, proper attachment of components to the implants, verification of fit, and an understanding of restoration placement procedures (cement-retained vs. screw-retained) will give the doctor and his or her team the skills to complete cases with confidence.
While individual situations exist that might require a certain treatment approach, developing a philosophy of treatment that can be shared with staff and surgeons will permit the doctor to develop a focused, efficient approach to implant-restorative dentistry. All crowns need to be secured to the implant or an abutment, so do you prefer a cementing or a screw-retained technique? Pick one technique and stay with it to the greatest extent possible, remembering that there will be cases that might require a different approach. Do you prefer to have some control over the abutment fabrication, or are you willing to defer all decision-making to the laboratory specialist? If you have time available during your day or are willing to complete laboratory procedures on days when patients are not in the office, are you eager to modify titanium abutments? Once you develop a philosophy of treatment, then it will be easier to establish systems.
Consider this philosophy of practice for implant-restorative dentistry:
Our aim is to provide our patients with implant-supported restorations that restore the function, comfort, and appearance of the tooth it replaces.
We will treatment-plan the case with the surgeon using appropriate imaging information and diagnostic models mounted on an articulator.
We will communicate to our patients the benefit of the recommended treatment, the possible complications that might be experienced, the expected time to complete the treatment, and the anticipated fee for the restorative treatment.
Once a philosophy of practice has been developed and a relationship with the surgeon who will be placing the implants has been established, then becoming familiar with at least one implant system will be necessary. Completing a technique course and developing an understanding of techniques and components by reading company manuals and newsletters will permit you to be as efficient as possible when the patient is in your treatment suite.
Initially, the doctor will need the following materials from the implant company to complete a single-tooth, implant-supported restoration:
1 Impression coping - there are at least three styles to consider:
a. A pick-up coping is screwed onto the implant and an impression tray with an opening cut into the tray above your coping. The screw, or guide pin, that holds the coping in place protrudes through the impression material and is unscrewed once the material has set. The tray is removed from the mouth and the coping remains in the impression.
b. A transfer coping is screwed onto the implant and an impression is taken just as it would be for a tooth-supported crown. Following the setting of the impression, the transfer coping is removed from the implant and placed back into the impression.
c.An indexing coping is secured onto the implant. Its position in the mouth can be registered by luting the coping to an acrylic or composite template that fits over the neighboring teeth or by flowing a firm bite-registration material over the occlusal surfaces of the proximal teeth and around the coping. The index is then transferred to a study model.
2 Implant analogs are secured onto the impression copings before the impressions are poured with the appropriate stone or before the index is set into the study model. Ordering two analogs for each implant is wise when the doctor is first becoming involved with implant-restorative dentistry. Analogs are small and, when dropped, seem to easily disappear. Considering the minimal cost of analogs, it makes sense to develop an inventory of components that will be of use for future cases.
3 Screwdrivers will be necessary to engage healing abutments, guide pins, and screws. Drivers are available with hex, square, or “star” shaped heads. The drivers are available with a short or long shank. Oftentimes the long shank is too difficult to use in the posterior of the mouth, and with anterior teeth there frequently is not enough space between teeth for the short-shank driver to engage the screw. Thus, both drivers should be purchased.
4 Torque drivers are crucial to properly complete the restorative treatment. The abutment screws are designed to be tightened to an optimal torque of up to 35 Ncm, and hand-tightening a screw can only achieve approximately 10 Ncm of torque. Therefore, if the doctor does not wish to purchase a torque driver initially, then once the abutment is seated, the surgeon must torque the abutment screw.
For the doctor who has enough time or prefers to control procedures:
Once the impression has been taken, the lab analog will be attached to the impression coping. If the occlusal platform of the implant is placed subgingivally, then it is wise to place a soft-tissue mimicking material around the analog and impression coping. This material is important when developing emergence profiles of the crown. Once the mimic material is set, then the stone is poured into the impression.
Stock titanium abutments can be purchased that are either straight or angled, with collars that might extend to 5 mm in height. Modification of the abutment is necessary to fit the patient’s edentulous site. Brasseler and Axis manufacture a variety of titanium-cutting burs. A Brasseler H351 FSQ bur or an Axis UC129GTI bur will shape the titanium without the spectacular sparking seen with diamond burs. The doctor will develop axial inclination, occlusal clearance, and subgingival margin placement. The abutment is polished beautifully to a smooth finish with a white rubber wheel.
The optimal gingival placement of the margin is 1 mm buccally and .75 mm interproximally. Naturally, this may vary depending upon the thickness and translucency of the gingival as well as the position of the patient’s lip. Ceramic abutments are available for use wherever esthetics demand them.
For the doctor who prefers fabrication of abutment by laboratory specialist or by using CAD-CAM technology:
The laboratory specialist can fabricate abutments either by modification of a titanium abutment or by casting a custom abutment such as a UCLA abutment. The doctor needs only to provide an impression of the implant to the laboratory. The crowns are fabricated on the abutment and the doctor commits a minimum amount of chair time to the patient.
Computer-aided design and manufacturing procedures can provide state-of-the-art abutments to the doctor. An emerging technique developed by 3i requires only an impression of the patient’s arch while the healing abutment is in place. The coronal surface of the healing abutment is coded with notches and grooves that are unique to the diameter, emergence profile, and height of the abutment. It also indicates whether the implant has an external hex or an internal connection. The impression is sent to a laboratory that is capable of reading the impression and an abutment is manufactured.
Zimmer Dental uses a CAD-CAM procedure where customized abutments can be created with optimal parallelism and margin placement. Abutments for single or multiple implant situations can be created. Multiple abutments can be created for each implant, so fixed provisional restorations can be cemented into the patient’s mouth while the laboratory specialist fabricates the final restorations on another set of exact duplicates of the original abutments.
Back to the beginning ...
A well thought-out philosophy of treatment and protocol provide for profitable implant-restorative dentistry. Know yourself, your skills, and your patient. Aim to develop this profitable treatment modality in your own practice. Set about selecting and developing your systems and skills. If you are working with a surgical specialist, develop a collaborative relationship. The rest will follow.
Implant-restorative dentistry does provide profit, or benefit, to doctor and patient alike. The patient receives a restoration that should provide improved comfort, function, and esthetics for many years. A likely outcome for the patient is increased confidence, self-esteem, and an inclination to be an ambassador for comprehensive dentistry. Implant-restorative dentistry will enhance relationships with patients and all of the doctors involved with the case. If the restorative specialist develops a philosophy of implant treatment as well as a protocol to complete implant cases efficiently, then a financial profit will become a much-desired benefit for the doctor.
John F. Davis, DDS, graduated from the Loyola University School of Dentistry in 1976, and has a restorative practice in Park Ridge, Ill. Dr. Davis has served on the visiting faculty of The Pankey Institute since 1992. He is affiliated with the American Dental Society, Illinois Dental Society, Chicago Dental Society, AGD, and American Equilibration Society, and is a fellow of the AGD. Reach him at [email protected].