The economics of implants
Jeffrey Ganeles, DMD, FACD,
Frederic J. Norkin, DMD, and
Julio Sekler, DMD, MMSc
Implant dentistry is rapidly becoming a preferred mode of permanent-tooth replacement for many patients in clinical situations. Increasingly, patients demand implant-supported restorations in lieu of fixed or removable partial dentures. Yet there is still a gap between the numbers of implant procedures performed in the United States and the number of teeth to be replaced. In a May 2002 Dental Economics article, author Jeffrey Ganeles, DMD, discussed economic and professional issues that address trends toward implant dentistry. Factors identified to permit and encourage this shift include:
• personal confidence and successful experiences of the dentist with implant dentistry, creating a positive belief in the process;
• an ability to communicate to patients the benefits of implant dentistry;
• reduction or elimination of complications, warranty work, and problem solving using appropriate planning, accurate surgical procedures, and efficient laboratory techniques;
• application of evidence-based decision-making principles to treatment planning and patient education; and
• an ability to profitably deliver implant dentistry at similar or better margins than conventional alternatives.
Despite logical and economic arguments for implant dentistry, a common concern for patients and dentists is the anticipation that implant dentistry will be a time-consuming, drawn-out process. The belief stems from professional education traditions. Classically, dentists were taught that osseointegration — the biological connection between living bone and dental implants — required three to nine months of stress-free healing. Other requisite conditions specified in the 1980s and early 1990s included submucosal healing, surgical placement in a sterile operating-room environment, and lack of radiographs during healing.
Osseointegration is critical
While it is still accepted that the biological process of osseointegration is fundamental for predictable implant dentistry, the conditions to achieve it have been more finely elucidated through scientific investigations. Non-submerged healing is equally predictable to submerged techniques with many implant manufacturers highlighting this approach. Surgical procedures overwhelmingly are performed in aseptic dental offices without sacrificing implant predictability, rather than in hospital operating rooms. Radiographs are routinely taken during all phases of implant healing without measurable impact to implant success.
Most important for decision making and patient management, osseointegration of dental implants relies less on calendar-dependent healing time than on specific conditions. These factors include patients' bone volume and density, specific implant surface chemistry and texture, implant stability, and force application during early healing. Dental and orthopedic scientific literature confirm metallic implants can achieve osseointegration while in function as long as strict surgical guidelines, material specifications, and stability criteria are met. Recognition of these properties has stimulated hundreds of scientific articles published in refereed journals documenting clinical and histological success of accelerated-loading protocols for dental implants.
Following the process of evidence-based decision making, several professional organizations convened consensus conferences to summarize the literature on early and immediate loading. These groups include the International Team for Implantology in Gstaad, Switzerland, and the American Academy of Implant Dentistry in Hollywood, Fla., both in 2003, and the Sociedad Espanola de Implantes World Congress in Barcelona, Spain, in 2002. These groups have published or will publish their conclusions and recommendations based on their own criteria and review of literature to serve as foundations for evidence-based decision making for practitioners.
Early and immediate loading
Definitions for loading protocols generally have been agreed upon among the groups for immediate, early, and conventional time frames. Immediate loading, or restoration, is placement of a restoration — permanent or provisional — on an implant within 48 to 72 hours of surgical implant placement. Conventional loading is the placement of restorations after the traditional three- to six-month integration period. Early loading is any healing time interval between immediate and conventional periods. It is not within the scope of this article to review conclusions and recommendations from these conferences, but it should be sufficient to indicate substantial evidence suggests all loading protocols may be predictable under certain circumstances. Different implant manufacturers and designs present different types and quantities of data for clinical situations that may not be compared easily or generalized beyond tested conditions. One manufacturer's implant should be assumed to behave differently than another's until they are specifically tested and evaluated.
Several implant manufacturers also have achieved U.S. Food and Drug Administration clearance for claiming reduced-healing times for their implants. These include The Straumann Company, Nobel Biocare, and Implant Innovations, Inc. who have permission to market their implants for early and immediate restoration and loading.
Clinical implications
The practical implications for patients, dentists, and dental care delivery systems are profound for shortened healing times with predictable results. For patients, the prospect of having immediate tooth replacement satisfies the need to finish treatment faster. Fewer appointments or shorter waiting times create less intrusion on patients' personal and work schedules. Most often, provisional restorations are placed directly on dental implants, eliminating different kinds of fixed or removable provisional restorations. In larger conventional cases where removable dentures were used for provisional restorations, a significant number of appointments would be anticipated to adjust the provisional restoration following implant surgery. These time-consuming adjustments are virtually eliminated with immediate loading procedures.
Highlighting this observation of time efficiency in Clinical Implant Dentistry and Related Research in May 2003, Chee and Jivraj from the University Southern California School of Dentistry compared two groups of seven patients who were treated with either conventional or immediate loading protocols for full-mandibular restorations. They noted a 100 percent success rate of implants and restorations in both groups. Significantly, the immediately loaded group spent one long appointment to achieve their results, while the conventional group took 38 visits. Asking a patient to take a day out of his or her schedule to reconstruct dentition is more feasible than requiring a person to commit to a seemingly unending series of 38 appointments. This is particularly true for busy patients with business, occupational, family, or travel commitments that could preclude accepting long, time-consuming courses of treatment. Many patients who require extensive treatment often develop their problems specifically because they are anxious or phobic about dental procedures. Being able to condense treatment into a single or limited-number of discreet appointments is often better tolerated by tense patients as the dentist can effectively address the psychological obstacles with effective anxiolytic pharmaceuticals or other techniques.
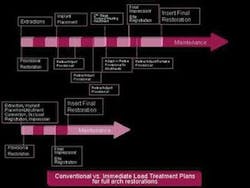
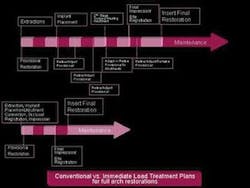
Figure 1
Figure 1 illustrates an approximation of time efficiency from our private practice environment. The immediate load protocol allows for a bulk of work to be accomplished early in treatment, shortening the time needed for rehabilitation. Accomplishing extractions, implant placement, abutment connection, and provisionalization in a single visit, the final healing process is initiated on day zero. Following a healing period of two to three months, the implants are osseointegrated, the soft-tissue complex developed, and the patient returned to the restorative dentist for final impressions and restoration. In this example, a rehabilitation can be accomplished four to seven months faster than conventional protocols.
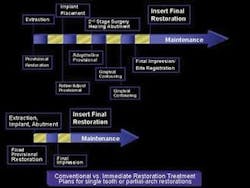
Figure 2
Figure 2 shows a similar comparison for a single-tooth or partial-arch clinical situation. Again, dramatic chair time and overall treatment-time reduction is evident.
Dental practices benefit from the altered time dynamics of immediate loading or restoration procedures. Most dentists would agree it is easier and more desirable to treat a single patient for several hours, rather than having a turnstile office with dozens of short visits. Providing fewer, longer appointments lessens office traffic, administrative work, set-up and clean-up of treatment rooms, use of disposable items, and generally reduces overhead costs.
Other clinical advantages of immediately loaded or restored implants are evident. In the aesthetic zone, placing an accurately contoured provisional restoration at the time of tooth extraction may retain gingival anatomy. Papilla preservation, often critical for optimal aesthetics, is far more effective than difficult, technique-sensitive reconstruction techniques. Using these techniques ideally eliminates the future need for time-consuming, inefficient, and often uncompensated gingival-aesthetic contouring.
Immediately loaded or restored implant procedures alter the usual workflow of both the surgical and restorative dentists and their staffs. Many different protocols have been described to provide these services to patients. Some require surgeons to perform some restorative procedures, while other techniques require restorative dentists to assume early post-surgical care of patients. Dental technicians need to become more intimately integrated into treatment through pre-surgical preparation and short-deadline delivery of accurate provisional restorations. Regardless of the specific techniques used, new stresses are placed on the delivery systems with the need to fully integrate surgical and restorative aspects of treatment.
For every patient who is treated, the therapeutic team should address the following issues to clarify workflow and responsibilities:
• When is the provisional to be delivered?
Day of surgery or day after? Office- or laboratory-processed provisional restoration?
• Who will deliver the provisional?
Restorative dentist or surgeon?
•Comfort level of surgeon with restorative procedures such as impressions, occlusal adjustment?
• Comfort level of restorative dentist manipulating surgical site such as re-suturing wounds or impression taking in edematous or bleeding sites?
•Whose time is used most efficiently?
Surgeon performing restorative procedures? Restorative dentist manipulating implants in recent surgical site? Both doctors present together for combined procedure? Dental technician, assistant, or dentist fabricating immediate provisional restoration?
•Who will take responsibility for complications?
There are no right or wrong answers to the previous questions as each patient will have different demands and expectations, and each therapeutic team will have their own capabilities and comfort zones.
In our practice, we have evolved with a dental technician to provide the majority of the provisional restorations for patients receiving immediately loaded or restored implants. Our job is to provide the finished surgical product of healed, integrated implants for the restorative dentists to finish.
In developing expertise and experience, we have gained significant efficiency in creating and controlling provisional restorations. Diagnostic and preparatory work is performed in conjunction with restorative doctors and laboratory technicians to use their expertise and insight and maintain the team concept of treatment. Once implants are adequately healed, patients are referred back to their dentists to finesse provisional restorations and complete. This division of labor defines our surgical group's responsibility for complications during the critical, early-healing phase of treatment, giving restorative dentists and patients confidence in our recommendations.
Predictable results
Most publications that discuss immediate and early loading and restoration of dental implants demonstrate success rates similar to or better than conventional loading protocols. Nevertheless, this can be a misleading statistical phenomenon. Most publications are written by experienced, highly skilled practitioners working under tightly controlled clinical conditions on few implants or patients. Often their success rates exemplify the optimal results attainable.
Successfully providing these kinds of services to patients in routine practice requires adherence to protocols and attention to details. These types of procedures are among the most demanding and meticulous types of dental implant services with the least margin for error.
Surgical procedures must be precise, occlusal control must be exact, and restorations must be highly refined in a compressed time frame. Each member of the therapeutic team must be fully aware, skilled, and coordinated into his or her specific treatment role.
For dentists beginning to provide immediate loading or restoration of dental implants, it is important to have successful outcomes immediately. Appropriate case selection can dramatically enhance success rates. One of the most empowering, reassuring messages patients receive from doctors is confidence in the proposed treatment. This is particularly important with expensive and new techniques.
The most predictable immediate loading/restoration cases (in descending order) include full-arch mandibular cases, single anterior teeth, partial-arch tooth replacement, and full maxillary arch cases.
Failure with these kinds of procedures is increased because of their potential complexity. Similarly, the consequences for failure are magnified as compared with conventional treatment protocols because of heightened patient expectations and the frequent lack of backup provisional restorations or secondary treatment plans.
Profitability
The equation of larger cases, time efficiency, meticulous planning, and precision techniques can equal increased profitability compared with conventional implant dentistry. Prerequisites such as professional and staff training, preparation, and coordination are optimal. Once a system is functioning, treatment planning and case transitioning become easier and more efficient than conventional implant dentistry.
Despite reduced treatment time, the value of the service is significantly greater than conventional procedures. Dentists could legitimately charge a premium as compensation for taking less patient time, requiring additional preparation, and placing higher stress and higher demands on the therapeutic team. Alternatively, dentists could conclude these services adequately increase their efficiency and hourly profitability without charging additional fees.
Another benefit is that once implants have successfully survived the immediate provisional restoration, there is almost never a late failing implant to cause a remake. Instead, dentists restore "tested and proven" implants. Our practice has observed that some restorative dentists reduce their fees because of reduction in time, complexity, and risk of late failure that accompany completion of these cases.
Marketing opportunity
Incorporating immediate loading and restoration of dental implants benefits the marketing program of a practice. It defines the office as providing cutting edge, patient-oriented treatment. Providing these services shows that the dentist and staff are listening to patient desires and finding new methods to meet those demands predictably, scientifically, and safely.
Eliminating treatment obstacles such as time, anxiety, and unpredictability permits patients to accept treatment proposals for necessary and elective procedures. When presented with desirable, comprehensive treatment proposals, patients often find methods to afford the large expense. Financing options can be justified by the lifespan of the proposed restorations, measured in decades instead of a few years.
Several corporations publicize the desirability and tap the market for immediate loading and restoration of dental implants. Numerous protected names for the procedures have been registered with the U.S. Patent and Trademark Office including TeethToday, Teeth Now, Teeth in an Hour, and Teeth in a Day. In addition, these procedures have been featured on television with patients on ABC's "Extreme Makeover." Numerous stories on the procedures have appeared in local television news, magazines, newspapers, and other media. Practices that feed into this activity will benefit with streams of motivated, financially capable patients who have tolerated inadequate restorations or avoided treatment in the past.
Highest form of aesthetics — tooth replacement
Americans are impatient by nature, goal-oriented, and aesthetically driven. In the last decades, implant dentistry opened new options in tooth replacement, restoring dental integrity, and self-confident smiles. Safely and predictably implementing faster, more-efficient techniques to deliver these results meets patients' desires and needs. Dentists who can achieve these objectives will benefit in growing demand for their services, greater office productivity, greater patient satisfaction, and greater professional accomplishment.