Composite restorations — fast, easy, and effective!
By Ara Nazarian, DDS
For more on this topic, go to www.dentaleconomics.com and search using the following key words: remineralization, composite restorations, metal-free dentistry, minimally invasive, adhesive restorations, prevention, wet bonding, Dr. Ara Nazarian.
During the past 50 years, we have seen a dramatic progression in dentistry as phosphoric acid has improved adhesion to enamel. In fact, the first dental adhesives bonded resins to enamel only, with little or no dentin adhesion. Subsequent generations of dental adhesives have significantly increased bond strength to dentin and the sealing of dentin margins while retaining a strong bond to enamel. Advancements in composite technology as well have enabled dentists to offer patients esthetic restorations that will last. With more demand for metal-free dentistry coming from our patients, the use of dental resins as cements or direct restorations will continue to increase.
Today, restorative dentistry emphasizes minimally invasive approaches. This encompasses prevention, remineralization, and when needed, adhesive restorations. These approaches decrease the chance for subsequent adverse outcomes, including advancement of tooth decay, pulpal involvement, and tooth fracture.
Decay is the process or result of demineralization (softening) of an area of dental tissue, which creates a decayed lesion on the tooth. The process of restoring decay begins with an analysis of the decayed lesions, taking into consideration their location and severity, with particular regard to the state of reversibility.
Reversible decay is referred to as noncavitated decay, where healing is possible by the hardening process of remineralization. When a cavity forms from excessive demineralization, the decay has reached the point of no return — tooth structure has been lost, and the decay is permanent or nonreversible.
In this situation of cavitated decay, the cavity will need to be filled to restore the tooth. Minimal intervention dentistry focuses on filling only these regions, removing as little of the tooth structure as possible. Classifications of the location and severity of decay are made in order to establish guidelines for suitable treatment. This article will discuss the use of composites with the advances in technology — without sacrificing durability or longevity — in a conservative approach to tooth restoration.
History
There has been an evolution the past 45 years in the development of dental bonding systems with variations in chemistry, application, mechanism, techniques, and effectiveness. We will quickly review dental adhesives according to a series of generations to understand the general characteristics of each group.
The first and second generation bonding agents used during the 1960s and ’70s did not recommend etching the dentin and relied on adhesion to the attached smear layer. The weak bond strength (2MPa-6MPa) to the smear layer still allowed dentin leakage with clinical margin stain.
The third generation systems of the 1980s introduced acid etching of dentin and a separate primer designed to penetrate into the dentin tubules as a method to increase bond strength. These systems increased the bond strength to dentin (12MPa-15MPa) and decreased dentin margin failure. However, with time, margin staining caused clinical failure.
The fourth generation adhesive systems of the early 1990s used chemistry that penetrated etched and decalcified dentin tubules and dentin substrate, forming a “hybrid” layer of collagen and resin. Fusayama and Nakabayashi described the penetration of resin into dentin to give high bond strengths and a dentin seal.
Dr. Kanca introduced the idea of “wet bonding” with these systems. Some of the products in this category include All-Bond 2 (Bisco), OptiBond FL (Kerr), and Adper Scotchbond Multipurpose (3M ESPE). These bonding agent systems have the longest track record as far as research goes, and they perform well clinically.
In fact, OptiBond FL, an 18-year-old product, received Product of the Year from Reality magazine. The bond strengths for these fourth generation adhesives were in the low to mid 20MPa range, and they significantly reduced margin leakage compared to earlier systems.
This system was very technique sensitive and required a very exacting technique of controlled etching, with acid on enamel and dentin followed by two or more components on both enamel and dentin. Because of the complexity with multiple bottles and steps, dentists began requesting a simplified adhesive system.
The fifth generation bonding systems introduced in the mid 1990s combined the primer and adhesive in one bottle while still maintaining high bond strengths. Some of the products in this category include Excite (Ivoclar Vivadent), OptiBond Solo Plus (Kerr), Prime and Bond NT (Dentsply), and Adper Singlebond (3M ESPE).
Unit-dose packaging introduced during the fifth generation bonding agents provided fresh chemistry for each procedure. Controlled etching, surface wetness, and resin placement continued to be a clinical challenge for some clinicians.
The sixth generation bonding systems introduced in the late 1990s and early 2000s, also known as the “self-etching primers,” were a dramatic leap forward in technology. The separate acid etching step was eliminated by incorporating an acidic primer, which was placed on the enamel and dentin after tooth preparation.
Several variations involved either mixing the acidic primer and adhesive before placement on the dentin and enamel, or leaving the primer on the tooth and then placing the adhesive over the primer. Some products in this class are Clearfil SF Bond (Kuraray), Simplicity (Apex), and Adper Prompt L-Pop (3M ESPE).
These systems were also reported to reduce the incidence of post-treatment sensitivity found in previous systems. However, the bond strength to dentin and enamel is lower than the fourth and fifth generation systems.
The seventh generation bonding systems are the “all-in-one” adhesives that combine etch, prime, and bond in a solution. Seventh generation bonding systems were introduced in late 2002.
Laboratory studies show that the bond strengths and margin sealing are equal to the sixth generation systems. Some of the products in this category include I-Bond (Heraeus), Xeno (Dentsply), G-Bond (GC), Complete (Cosmedent), and OptiBond All-In-One (Kerr).
Case Presentation
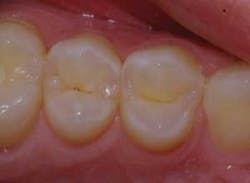
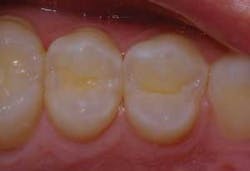
A patient presented for her cleaning and examination appointment concerned about a dark spot in the upper right quadrant and some sensitivity to sweets. Upon clinical examination, it was evident that tooth No. 4 might have some decay.
Upon closer examination and probing with an explorer, as well as confirmation with the DIAGNOdent (Kavo), the patient was informed that she did indeed have an occlusal cavity (Fig. 1).
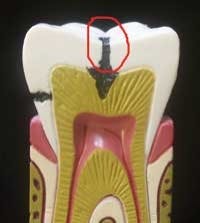
Once I captured the images of the occlusal cavity with my intraoral camera (RF Systems), I described theThe first segment of DemoDent (Fig. 2) can be used to illustrate occlusal and interproximal caries in a virgin tooth. Recession of gingival tissues is found on the reverse side of this segment. Also, the tooth can be removed to illustrate the socket and root structure. We used this section of the model in the following manner.
“There are three layers in a tooth as illustrated in this model. The white is the enamel, the yellow is the dentin, and the pink is the nerve. Your cavity is in the biting surface of the tooth, where food and debris collect.
When the cavity is in the enamel (white layer) you usually do not have any pain or sensitivity. In fact, by catching the cavity early, we can clean it out without the need for anesthetic.
Once the cavity has gone through the enamel and into the dentin (yellow layer), it spreads much more quickly. Patients may experience some sensitivity to hot, cold, and sweets, depending on how deep it has extended.
Once the cavity gets into the nerve (pink layer), patients experience constant throbbing pain. We want to prevent this by stopping the cavity as soon as possible.”
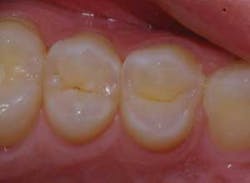
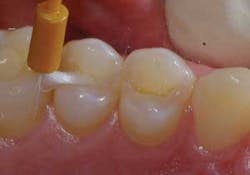
The occlusal contacts were initially recorded to help guide placement of the composite material (to avoid areas of centric contacts). An appropriate shade (B1) was then chosen and a small diamond bur (Axis) was used to initially remove the decay (Fig. 3).
The preparation was further extended to remove any staining or remaining decay in the occlusal grooves (Fig. 4). Using the provided microbrush, the Vertise Flow (Kerr Corporation) material was brushed with moderate pressure onto the prepared tooth structure for 15 to 20 seconds to obtain a thin layer (this initial layer should be no more than 0.5 mm) (Fig. 5).
The material was then light cured for 20 seconds with the Demi (Kerr Corporation) curing light. After lining the cavity wall and beveled area with Vertise Flow (Kerr Corporation), the restoration was built up with more composite material in increments of 2 mm or less and light cured for an additional 20 seconds.
Vertise Flow (Kerr Corporation) has a relatively low modulus and acts as an elastic gradient between the dentin and the stiffer microhybrid, thus moderating polymerization shrinkage stress at the margins. Its low viscosity also wets the internal surfaces of the prepared cavity and helps ensure a well-adapted first layer without fear of overetching.
Fig. 5: Application of Vertise Flow on tooth preparation
This self-adhering, flowable composite technology eliminates the need for a separate bonding application step with composites for direct restorative procedures. I have personally found that this product simplifies the direct restorative procedure by incorporating the bonding agent into the flowable, and offers high bond strength, high mechanical strength, and other physical attributes comparable to traditional flowable composites.
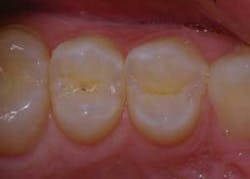
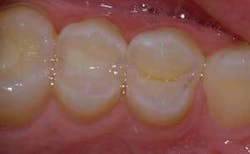
Once the restoration was filled and cured, it was shaped, trimmed, and finished using a fine diamond (Axis). The occlusion was checked and verified to make sure there were no interferences in lateral and protrusive movements (Fig. 6).
Fig. 6: Postoperative view of composite restorations
Clinicians today have a variety of esthetic and functional materials to choose from when they need to perform restorative dentistry. As dentists, we are always looking for something quick and simple to use, yet very effective. Vertise Flow self-adhering composite offers some great benefits, whether it is used as the main adhesive flowable or as an adjunctive bonding agent.
Additional indications for which I have used Vertise Flow include: repair of enamel defects, repair of porcelain restorations, blocking of undercuts, minor occlusal build-ups in nonstress-bearing areas, and incisal abrasions.
Ara Nazarian, DDS, maintains a private practice in Troy, Mich., with an emphasis on comprehensive and restorative care. He has conducted lectures and hands-on workshops on esthetic materials and techniques in the U.S., Europe, New Zealand, and Australia. Dr. Nazarian can be reached at www.aranazariandds.com or (248) 457-0500.