Ask Dr. Christensen
Gordon J. Christensen, DDS, MSD, PhD
Ceramic restoration cementation
Q I’ve heard various opinions on the best cements and cementing techniques to use with the numerous all-ceramic restorations now being promoted. Some are saying to bond every type of all-ceramic restoration, and others are using popular resin-modified glass ionomers or other cements. What are the most appropriate cements for these restorations?
A Your question is loaded with various additional questions, such as which all-ceramic crowns are best, when should they be used, should they replace porcelain-fused-to-metal, has there been adequate in-vitro and in-vivo research on these restorations, and more.
In my answer, I will assume that you feel the crowns are acceptable from a research aspect, and that you are using them in your practice. At this point, I will candidly state that more research and clinical observation is desirable on most of the new tooth-colored indirect restorations.
I will concentrate on the most acceptable cements and cementation techniques for various types of restorations, as well as the relative ease of removing restorations when it is necessary to replace them.
Tooth preparation desensitization before cementation
Numerous methods for desensitizing tooth preparations have been suggested. The Clinicians Report in-depth research division (TRAC) has shown that two 1-minute applications of glutaraldehyde solution (Gluma from Heraeus, G5 from Clinician’s Choice, MicroPrime from Danville, or Glu/Sense from Centrix) not only desensitize dentin surfaces, they also kill the organisms on the tooth preparation. I suggest this technique to reduce or eliminate tooth sensitivity before use of any current cement described below.
Types of currently popular tooth-colored indirect restorations
At least some of the following types of tooth-colored indirect restorations are currently being used in most practices. Porcelain-fused-to-metal is included, since it is still a viable and commonly used restoration:
• Porcelain-fused-to-metal (PFM) — These restorations have served patients well for over 50 years. Their breakage rates are relatively low, and their predictability is good, especially for single units. However, their replacement with all-ceramic restorations has been prompted by frequent loss of superficial characterizing stains from consuming acidic foods and beverages, as well as display of unsightly margins when gingiva recedes. Properly fabricated, these restorations are strong and relatively long lasting. They can be cemented with any cement the practitioner chooses. In North America, the most commonly used cement for PFM restorations is resin-modified glass ionomer, which allows easy restoration removal when necessary.
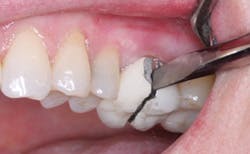
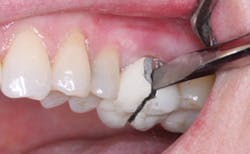
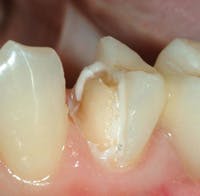
• Zirconia-based and full-zirconia restorations (Figs. 1 and 2)
Full-zirconia restorations are remarkably strong. They are being placed in significant and increasing numbers with near unanimous clinical success and patient satisfaction. They are rapidly becoming one of the most used types of tooth-colored indirect restorations for both single and multiple tooth indications. Because of their high strength, full-zirconia restorations may be cemented with any cement of the practitioner’s choice. I suggest resin-modified glass ionomer cement to take advantage of fluoride release, bond to tooth structure, good expansion and contraction characteristics, and moderate strength, which allow easy removal when necessary. After an unpredictable introduction of zirconia-based restorations because of superficial veneer ceramic chipping and cracking, the veneering materials for zirconia-based restorations have been modified and are becoming more predictable for both single and multiple-tooth connected restorations.
They can be cemented with any cement. I suggest resin-modified glass ionomer for the same reasons as full-zirconia restorations.
Removing either full-zirconia or zirconia-based restorations is moderately to extremely difficult depending on the thickness of the zirconia. This is one of the most significant reasons that a cement of only moderate strength, such as resin-modified glass ionomer, should be used. Research in our group, Clinicians Report, has shown that such cement is adequate for routine use with zirconia restorations. Removal often requires wearing out several diamond burs for even a single crown, using copious water spray, and a light, intermittent, sawing action.
• Lithium disilicate (IPS e. max)
These popular, tooth-colored, monolithic restorations for single-tooth restorations are strong and growing in acceptance. Depending on the size and type of the tooth-colored IPS e.max restoration, I suggest different cementation techniques.
If the restoration replaces only a part of the coronal portion of the tooth, such as an onlay, the retention offered by the configuration of the tooth preparation is usually minimal, and strong cement is indicated. In such situations, I suggest selectively acid etching the enamel areas only, placing the two 1-minute applications of glutaraldehyde, sucking off the remaining glutaraldehyde, placing a self-etch primer on the tooth preparation, and cementing with a resin cement such as Ivoclar Multilink Automix or Kuraray Clearfil Esthetic Resin Cement.
Other popular self-etch-containing resin cements for these situations are 3M ESPE RelyX Unicem 2 and Kerr Maxcem Elite. Use of either of these eliminates the need for a separate application of self-etch primer. This selective etch concept reduces or eliminates postoperative tooth sensitivity, which is a frequent complaint with this type of partial coronal tooth structure restoration.
If the IPS e.max restoration is a full crown, and the tooth preparation has acceptable retentive characteristics, I suggest using resin-modified glass ionomer cement to allow easier removal of the restoration if necessary. Removal of IPS e.max restorations is moderately to extremely difficult, which is one of the major reasons for using moderate strength cement for full-crown tooth restorations.
• Other less frequently used tooth-colored indirect restorations
Other restoration types, such as leucite reinforced ceramic (example – IPS Empress), feldspathic ceramic, polymer and aluminous ceramics, are best cemented with strong resin cement as suggested for onlays in the previous section. I suggest the following procedure:
- Sandblast or hydrofluoric acid etch the internal of the restoration.
- Place silane on the internal of the restoration.
- Selectively acid etch the tooth preparation enamel.
- Accomplish two 1-minute applications of glutaraldehyde.
- (If using self-etching resin cement, omit this step.) Place self-etch bonding material on the entire preparation surface, including the total-etched portion.
- Seat the restoration with resin cement as described previously.
None of the materials in this section are difficult to remove. The suggestion to use resin cement is primarily related to the relative weakness of the restorations when compared to the other tooth-colored restorations described.
In conclusion, for my cementation suggestions, the cement for any situation is related to numerous factors, including need for restoration strength enhancement, potential for postoperative tooth sensitivity, color of cement if using a very translucent restoration, and ease of removal when necessary. Use good judgment on each type of restoration.
Our course, “Faster, Easier, Higher Quality Dentistry” is the most useful course offered by Practical Clinical Courses. I teach this fast-paced and exciting course, identifying the 10 most successful clinical techniques and the most successful materials for typical general practices. Our next dates for the course are June 21-22 in Provo, Utah. Also, our DVD “Complex Oral Rehabilitation” (V1934) shows cementation technique in detail, as well as all other aspects of full-mouth rehabilitation. For more information, contact PCC at (800) 223-6569 or visit the website at www.pccdental.com.
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an email to [email protected].
Gordon Christensen, DDS, MSD, PhD, is a practicing prosthodontist in Provo, Utah. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of CLINICIANS REPORT (formerly Clinical Research Associates).
Past DE Issues