Ask Dr. Christensen
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an e-mail to [email protected].
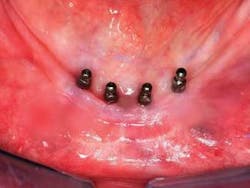
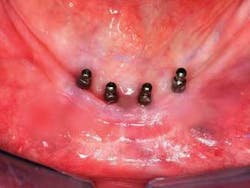
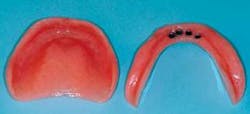
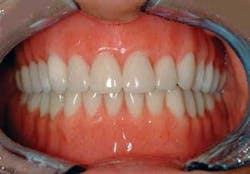
Q I am interested in small-diameter implants because I have been told that they can be loaded immediately after placement. Is that correct?A Many patients have inadequate bone present for standard diameter implants and will not accept grafting procedures. A viable alternative, the small diameter implant, is continuing to receive wider use and acceptance.Small-diameter implants (SDIs), “mini” implants, or narrow-body implants are usually described as being less than 3 mm in diameter. Most of them being used today are about 1.8 to 2.4 mm in diameter. These small-diameter implants have been used for many years as provisional support for prostheses, while standard 4 mm-diameter implants were integrating into the bone. Since the late 1990s, many dentists have been using them for long-term support of both fi xed and removable prostheses. IMTEC Corporation received FDA approval for long-term use of its mini implant in 1999. Several companies are now promoting small-diameter implants for long-term use. If adequate bone is present, many of the mini implants can be placed without making a fl ap. However, in some situations, a flap procedure must be accomplished to allow vision of the bone morphology and adequate placement of the implant.
Yes, these small-diameter implants can be loaded as soon as they are placed. Unlike conventional-diameter, root-form implants that are nearly 4 mm in diameter and require a hole nearly the size of the implant for insertion, the current generation of small-diameter implants are much like a screw for a hardwood board. A small, narrow-diameter osteotomy is made in the bone about one-third to one-half the anticipated depth of the mini implant, and the smalldiameter implant is screwed into the bone. The bone is expanded and widened by the implant as it cuts its way deeper than the original osteotomy site. The result is a very stable small implant immediately on placement.
Clinical success continues to be acknowledged with immediately loaded, small-diameter implants, and research is generally positive concerning this concept.
One of our newest videos, #V2317 “Mini Implants For Your Practice,” shows placing and restoring small-diameter implants for removable and fi xed prostheses. Implementation of this concept into your practice will expand prosthodontic services for your patients. For more information, contact Practical Clinical Courses at (800) 223-6569, or visit www.pccdental.com.
There is no question that making a fi xed prosthesis and cementing it with provisional cement to an implant and a natural tooth is asking for trouble. I learned this as I had some very expensive failures about 15 years ago. Provisional cement is weak and often breaks loose, allowing the natural tooth to intrude into the bone. I have observed natural teeth intrude up to one-half inch after breaking loose from the abutment crown. This intrusion requires only a few months and usually requires removal of the affected tooth and a new, more extensive restoration.
Another technique has also given me signifi cant trouble. Early in the history of root-form implants, some clinicians suggested placing precision attachments or keyways between teeth and implants. This sounded like a logical concept. Again, I have had natural teeth intrude up to one half inch when keyways were placed between implants and natural teeth. The only solution to such a problem is usually extraction of the natural tooth.
There are situations where natural teeth and implants need to be connected because of inadequate bone in potential pontic areas, or to avoid placing more implants for financial reasons.
The following technique is successful if carried out exactly as outlined below. For our example, I will assume that one natural tooth is being connected to one implant, with one missing tooth being replaced with a pontic: