To bulk fill or not to bulk fill ... that is the question
Joyce Bassett, DDS, FAACD, FAGD
Direct composite restorations are the most requested and performed dental procedures. Class II posterior composites are the number one restoration dentists place. Bicuspids and molar treatments account for more than 70% of all direct restorations placed, but they generate only minimal revenue for practices.1 The average fee accepted by insurance companies for a Class II composite is $195. It takes substantial time to isolate, prepare, remove old resin and decay, bond, matrix, incrementally place the composite, cure, finish, and polish.2 If done properly, these restorations are the most demanding restorations we create. Where can we save time without compromising long-term predictability?
The incremental placement technique has been the gold standard for posterior universal composite placement. This technique carefully places and cures multiple layers of composite in 2 mm increments to minimize shrinkage stress and ensure adequate depth of cure.3 This technique, if done properly, is arduous, time-consuming, and-despite our efforts-we may still see shrinkage, gap formation, craze lines, and microleakage. How many of us are performing this technique in 2 mm increments?
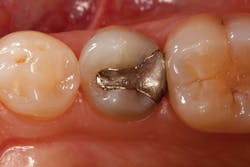
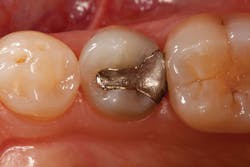
Figure 1: Pre-op amalgam with marginal leakage
Decreasing the insertion and polymerization time can simplify this procedure, improve chairside efficiency, and increase profits. Manufacturers have realized these problems and developed a more advanced dental composite designed specifically for posterior use. This composite allows a dentist to place larger increments of composites in a single application, rather than placing tedious layers and curing in small 2 mm increments. So what is the hesitation in making the switch? Many dentists are worried that the composite is not fully cured, especially in the deeper part of the proximal box. Can we believe the manufacturers?
Let's go to the independent researchers-Clinicians Report (Christensen), Dental Advisor, Reality, and the ADA. Hardness has been shown to correlate with polymerization.4 Researchers measure the hardness at the bottom of the box, then they measure the hardness at the top of the box. If it is at 80% (bottom to top depth to cure ratio), it is cured. Christensen's Clinicians Report5 confirmed hardness results at 6 mm for Kerr SonicFill to 4 mm for Tetric EvoCeram (Ivoclar) and Venus Bulk Fill (Heraeus Kulzer).
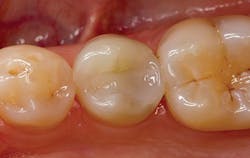
Figure 2: Post-op photo courtesy of Ron Jackson displaying five years of clinical success
All composites shrink; the material and placement technique must account for the polymerization shrinkage stress on the bonded interface. If it is excessive, then debonding or cuspal flexure will occur. It has been reported that avoiding bonding to opposing walls of the restorations all at once can mitigate shrinkage stress (the incremental technique). The most current literature shows that bulk filling with these revolutionary bulk-fill composites does produce lower shrinkage stress than the traditional universal composites placed in oblique layers.6
There are two categories of bulk fills. Low viscosity flowables (e.g., Surefil SDR Flow, Dentsply Caulk; 3M ESPE Filtek Bulk Fill Flowable Restorative, Voco X-tra Base, Heraeus Kulzer Venus Bulk Fill), and high viscosity restorative (e.g., Ivoclar Vivadent Tetric EvoCeram Bulk Fill and Voco X-tra Fil and Kerr SonicFill).
A low-viscosity flowable is placed in the bottom of the preparation as a dentin replacement base and then a second increment of composite is placed as enamel on the top layer. Two layers are placed and cured.
The high-viscosity restoratives are strong, but they do not adapt to the cavity walls, so it may be wise to place a low-viscosity composite or a resin ionomer liner to achieve intimate adaptation to the gingival and pulpal floors.7 Again, two layers are placed and cured.
One exception is Kerr's SonicFill. It is the only sonic-activated, single-step, bulk-fill composite that starts out as a low-viscosity composite. The handpiece is activated, liquefaction occurs, the viscosity drops, and optimal cavity adaption occurs, much like a true flowable. The cavity is filled in seconds; the composite goes through a phase change and it is transformed to a high-viscosity composite.
The Journal of the American Dental Association reports that 37% of our restorations are not fully cured.8 Undercured composites will display cracks, fractures, poor crosslinking, and color instability. Christensen reports that most curing lights are inadequate and delivered around 512mW/cm2.
A high-output LED light (1000mW/cm2) with a powerful collimated (directed, not scattered) beam is a requirement when curing these bulk-fill composites. The lights should be regularly checked for consistent output. There is an enormous difference between the clinical outcomes associated with a 500-watt light versus a 1000-watt light.
Increasing the curing time increases the bond strength. Since there is a distance between the light tip and the deeper placed composite, it is recommended to final cure the composite 10 seconds from the occlusal, 10 seconds from the buccal, and 10 seconds from the lingual.
Are dentists hesitant, since we have not seen long-term clinical performance? Split-mouth studies, where one quadrant is restored with universal composite (Kerr Premise) using the layering technique and the contralateral quadrant is restored with bulk fill (Kerr SonicFill) were evaluated. There were no clinical differences between the two materials and techniques at the two-year postoperative evaluations.9 Clinical cases have been documented showing five-year postoperative outcomes with Kerr SonicFill (figures 1-2).
Dentists are conscientious, work really hard, and take a lot of time to perform first-rate, predictable restorations. At the end of the month, we evaluate our profits and losses, and the overhead can be strangulating. Make the change with these innovative materials and technology, and you will save time and money. I predict that the incremental technique will be antiquated and invalid in two years. Bulk fill is the answer.
References
1. Clinicians Report. April 2014;7(4).
2. Nash R. Patient demand is increasing for posterior aesthetics. Dent Today. 2010;29:74, 76, 78-79.
3. Cheung GS. Reducing marginal leakage of posterior composite resin restorations: A review of clinical techniques. J Prosthet Dent. 1990;63(3):286-288.
4. Bouschlicher MR, Rueggeberg FA, Wilson BM. Correlation of bottom-to-top surface microhardness and conversion ratios of various resin composite compositions. Oper Dent. 2004; 29(6):698-704.
5. Christensen GJ. Clinicians Report. Jan 2012;5(1).
6. Tiba A, Zeller GG, Estrich CG, Hong A. A laboratory evaluation of bulk-fill versus traditional multi-increment-fill resin-based composites. J Am Dent Assoc. 2013 Oct;144(10):1182-1183.
7. Jackson RD. Posterior composites and the new bulk-fill materials. Inside Dentistry. 2014;10(8):68-75.
8. Fan PL. Curing-light intensity and depth of cure of resin-based composites tested according to international standard. JADA. 2002;133(4):429-434.
9. Ernst CP, Willershausen B, et al. Clinical study on SonicFill in posterior teeth, Final report after two years; comparison to baseline, 3-, 6- months and one year. Johannes Gutenberg University. Mainz, Germany. Am J Dent. 2012 Jun;25(3):131-135.
Joyce Bassett, DDS, FAACD, FAGD, is the president and an accredited fellow of the American Academy of Cosmetic Dentistry. She is an associate member of the American Academy of Esthetic Dentistry, a KOIS mentor, an active member in the Academy of Fixed Prosthodontics, and a fellow in the Academy of General Dentistry. She was voted top 5 female CE educators, and is a national lecturer and a published author. Contact Dr. Bassett by phone at (480) 367-8889, email [email protected], or visit www.drbassett.com.