Zirconia and lithium disilicate restorations versus PFM
Gordon J. Christensen, DDS, MSD, PhD
Q:
My dental laboratory technicians are trying to convince me to switch from placing mostly porcelain-fused-to-metal (PFM) restorations to using full zirconia or lithium disilicate restorations. I have placed many of each type, and so far I feel relatively good about both types of restorations. I am concerned about the long-term reliability of zirconia and lithium disilicate. Should I be concerned, or have these materials been proven long enough for acceptance?
A:
Dental practitioners are rapidly changing from PFM to zirconia and lithium disilicate. This change has been one of the fastest and most complete technique changes in the history of modern dentistry. But the change has taken place faster than the necessary research to support it could be accomplished.
My answer will include my opinions based on Clinicians Report Foundation's 10-year clinical research on the subject, my personal observations as a practicing prosthodontist, and the experiences of the many dentists I encounter around the world each week.
The long-term usefulness of both zirconia and lithium disilicate restorations is yet unknown. On the other hand, PFM has been used successfully for nearly 60 years (figures 1-3). Millions of restorations have been placed globally. The success of PFM is well documented, with major advantages.
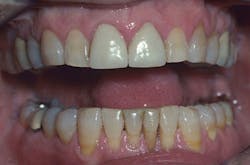
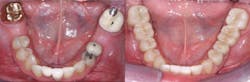
Figure 1: Patient with need for complete restorative rehabilitation
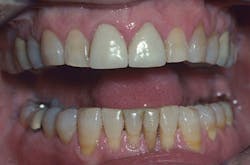
Figure 2: The patient in figure 1 was rehabilitated using PFM crowns and fixed prostheses. High noble metal was used as the base for the restorations.
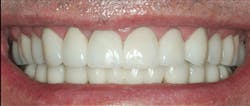
Figure 3: The patient shown in figures 1 and 2 at 20 years of service. One tooth (mandibular left first molar) had the need for endodontic treatment and was eventually extracted. There were cracks and chips in several of the posterior PFM crowns. However, PFM can serve very well, and most dentists know how to use it properly. It is a known procedure and should still be used in situations where it is indicated.
Consider these PFM characteristics with the characteristics you have observed with full zirconia and lithium disilicate:
• Strength for most clinical situations in all areas of the mouth.
• Proven history of clinical adequacy and success.
• Predictability. Clinical research has shown that most single PFM crowns will serve well for many years, and that three-unit PFM fixed prostheses are relatively long-term restorations if done well.
• Relatively good esthetics, at least for several years. Glaze and stain fired on to the superficial surfaces of PFM crowns gradually wear off after a few years. This leaves some of the restorations rough and off color, depending on the quality of the laboratory work on the restorations.
• Precision attachments are possible. Although this is not a frequently occurring need, it is not yet possible with the other two materials.
• Long-span fixed prostheses are well proven. Currently, full zirconia long- span fixed prostheses are being promoted. They are serving well at this early time, but more research is needed for verification of this use.
Current use of full zirconia restorations
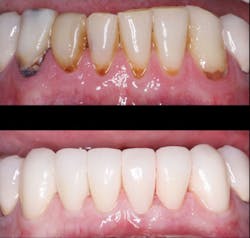
Full zirconia restorations are currently and rapidly monopolizing the full crown marketplace in most US locations, and many dentists are using them as their primary restoration when full crowns are indicated (figure 4).
Dental laboratories can make these restorations inexpensively and easily, allowing them to provide the crowns to dentists at a very low cost. Additionally, if dentists scan the tooth preparations instead of making conventional impressions, they may receive up to a 25% cost reduction from many laboratories.
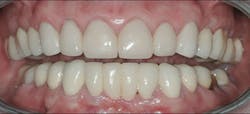
Figure 4: Full zirconia three-unit, fixed partial dentures serving for three years. Research is rapidly showing the good serviceability of these restorations, and their esthetic characteristics are improving.
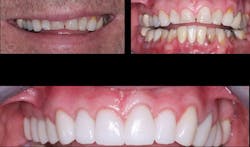
Figure 5: Lithium disilicate restorations are currently the most popular anterior single-unit crowns. They are beautiful and show promise for very good long-term service.
Figure 6: Lithium disilicate restorations are remarkably lifelike, simulating natural teeth nearly exactly.
When full zirconia crowns were introduced, many dentists did not feel they were acceptable from an esthetic standpoint. The esthetic result of full zirconia restorations is rapidly improving, as most zirconia companies and the dental laboratories working with them are changing the zirconia formulation to meet the esthetic demands of dentists and patients. These changes in the zirconia formulations are reducing the strength of the material. This reduction appears to be acceptable clinically, at least for single crowns, since the altered formulations are still several times stronger than other types of ceramic crowns. The acceptability of the altered zirconia formulations for fixed prostheses is yet to be proven.
Dentists are pleased with the soft-tissue response to full zirconia restorations. Many comment that patients who have serious soft-tissue irritation with metal or PFM restorations have a complete reversal of the soft-tissue challenge, often within just a few days after placing zirconia crowns.
The threat of the dreaded "phase change" exhibited with zirconia used in hip prostheses at about seven years of use has not been observed with zirconia used in the mouth, either as crowns or dental implants. However, full zirconia crowns have been used for only about five years. Researchers considering this alleged challenge, and major laboratories that have made millions of full zirconia restorations, feel confident that phase change reverting the zirconia back to an earlier degenerating stage will not occur in the mouth. There are two more years of use before we will begin to see if full zirconia is susceptible to this challenge.
In summary, dentists are using full zirconia restorations to a significant degree, their esthetic qualities are improving, they are not failing as much as other restorations over the five years they've been used in dentistry, they are extremely promising, and dentists and researchers are optimistic about them (figure 5).
I predict zirconia restorations in their coming iterations will gradually dominate the market. In the meantime, don't throw away PFM.
Current use of lithium disilicate
These restorations, which have been in clinical use for about 10 years, have been the solution for esthetic restorations for single crowns, veneers, onlays, and inlays. They have nearly eliminated use of other previously popular ceramic restorations when an excellent esthetic result is necessary. Use of lithium disilicate for fixed prostheses has been somewhat problematic, and most dental labs do not recommend this material for multiple-unit fixed restorations.
Since the advent of the esthetic improvement in full zirconia restorations, some labs are recommending full zirconia for molar teeth, and lithium disilicate for the premolars and anterior teeth. Undoubtedly such recommendations will increase rapidly as zirconia becomes more esthetically acceptable.
There is no doubt, as I poll the many audiences to which I speak, that there is significantly more breakage in service for single-unit lithium disilicate crowns than observed with full zirconia.
In summary of the current state of lithium disilicate restorations, they are beautiful, often rivaling the beauty of natural teeth. They are serving well as single crowns but not as well as full zirconia, they are not indicated for fixed prostheses, and patients highly appreciate them.
I predict that lithium disilicate will continue to be the major esthetic material for single crowns, onlays, veneers, and inlays for the short-term future. But I see numerous new similar materials under development that will challenge this material in the future (figure 6).
Summary
Full zirconia and lithium restorations are the fastest growing new concept in the profession. There is enough medium-term longevity information and research available to conclude that they are working better than any other full-ceramic restoration of the past. I would not hesitate to use either of them with confidence, but I would not throw away PFM yet.
Gordon J. Christensen, DDS, MSD, PhD, is a practicing prosthodontist in Provo, Utah. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Dr. Rella Christensen) and CEO of Clinicians Report (formerly Clinical Research Associates).