Aligner-based orthodontic therapy: A powerful adjunct to contemporary restorative practice
ByForoud Hakim, DDS, MBA
The impact of clear-aligner-based orthodontic therapies on the dental marketplace and the oral health of patients is no longer a subject for debate. Much of the early stigmas and concerns about these therapies-including boundaries between specialists and general practitioners, efficacy, predictability, scope of treatment complexity, and delivery-have faded.
As of 2013, Align Technologies (Invisalign) reported treatment of 11% of the total annual 2.6 million relevant orthodontic cases initiated globally. With well-established market leaders such as Align, and competitors that are gaining traction and market share such as ClearCorrect, it's apparent that aligner-based orthodontics will continue to be an integral part of the dental practice landscape.
As a private practitioner who is involved with both dental education and continuing education, I have witnessed the beneficial impact of the integration of clear-aligner-based orthodontic therapy in a variety of practice settings. These benefits fall into two categories: those that improve patient care and those that improve practice productivity.
Patient care benefits
1. Access and exposure to possible treatment
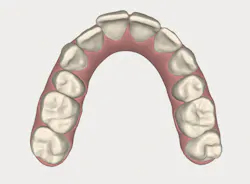
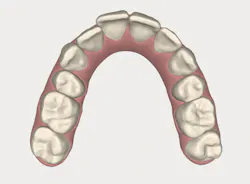
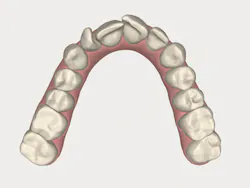
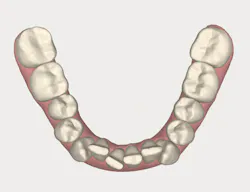
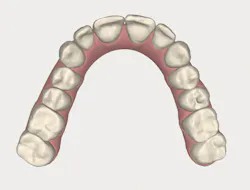
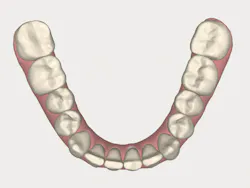
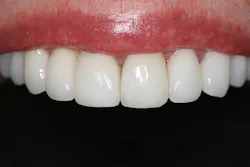
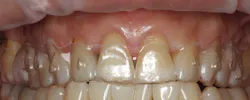
With an expanded workforce of practitioners-including specialists and generalists-there is an increased likelihood that the beneficial impact of alignment on oral health and ultimately, systemic health, will be presented to a patient who is a candidate for care. Figures 1 and 2 show a simple before-and-after simulation for enabling the patient to visualize recovery from anterior crowding (whether primary or relapsed).
Figure 1
Figure 2
2. Value-added features
While patients often pursue orthodontic alignment to improve their smile esthetics, they will also reap oral health benefits. Value-added benefits include oral hygiene access, periodontal health, and occlusal and masticatory function. In other words, patients who are seeking dessert dentistry unwittingly get their vegetables as well.
3. Optimized prosthetic outcomes
We all know that many patients who present for functional, esthetic, or combination restorative treatments would have improved outcomes if we could just move or unscramble their teeth into a better arch position. However, we also find that most adults are resistant to undergoing preprosthetic orthodontic treatment with traditional bracket-and-wire hardware. Their reasons include the perceived stigma of the esthetic setback from a mouthful of metal, the increased time for treatment completion, discomfort, oral hygiene challenges, and disruption to social activities.
Since clear aligners are nearly undetectable, have only a small learning curve, and can be removed for hygiene access and social events, many of the barriers to acceptance are eliminated. Most importantly, optimizing alignment prior to restorative dentistry generally results in reduced preparation, conservation of tooth structure, reduced incidence of endodontic complication, better esthetic outcomes, and lasting dentistry.
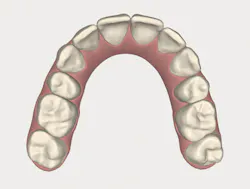
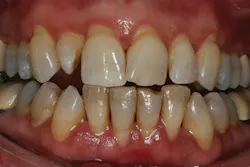
A complex example of a preprosthetic orthodontic case is seen in figures 3, 4, and 5. In this case, the severely crowded dental arches posed a significant challenge for functional and esthetic rehabilitation. Not only was the feasibility of successful "restorative-only" treatment in doubt, but attempting such treatment would have undoubtedly led to overly aggressive preparation of all of the teeth, devitalization of several teeth via prophylactic endodontic procedures, and a guarded long-term prognosis for case success and survival.
Figure 3
Figure 4
Figure 5
Figures 6 and 7 show the preprosthetic tooth movements after 18 months of aligner therapy, and figures 8 and 9 show the final rehabilitation. It is noteworthy that restorative treatment only spanned through the bicuspids, with only a few of the teeth relegated to full-crown preparations due to preexisting restorations. The majority of the teeth were restored with ceramic veneers and partial veneers. Happily, the patient reports 100% tooth vitality at the four-year mark with no endodontics initiated at the preparation phase.
Figure 6
Figure 7
Figure 8
Figure 9
Practice productivity benefits
1. Revenue impact
With simple orthodontic case fees typically ranging from $2,000 to $4,000, and with comprehensive cases ranging from $4,000 to $6,500 in most markets, these services have the potential to augment a practice's annual production dramatically. Furthermore, as seen in the preprosthetic case (figures 3-9), empowering patients to accept a more ideal approach toward restorative treatment can be the difference between cases that should and shouldn't be treated. Further, patients who are made aware of the expanded possibilities for better health and esthetics through treatment become more aware of their dental needs and are more likely to pursue both needed and elective dentistry in the future.
2. Marketing and referrals
Given my personal experience, many patients who are profoundly affected by positive outcomes experience the overwhelming sentiment that their dental practitioner is vested in their health and well-being. As a result, they often become zealots for new-patient referrals, which makes them a powerful internal marketing force.
3. Predictable outcomes
Anyone in private practice knows that efficiency and reliability directly impact the bottom line. Having to redo a failed procedure of any kind is a drain on chairtime, overhead, productivity, and patient confidence and satisfaction. Clear-aligner-based orthodontics is predictable treatment-largely due to automated case selection and treatment-planning protocols that are driven by highly developed software platforms.
Despite this, delivery, execution, and treatment chaperoning still fall on the shoulders of the practitioner. Since aligner-based orthodontic treatment is most often driven by firmly bonded composite highlights on involved teeth, known as "attachments," having the right products for these can further improve efficiency and predictability.
Like most practitioners, I've experienced the burden of trying to add the best consumable products to my practice inventory with financial savvy. I am not a big fan of purchasing expensive dental products, gadgets, or equipment unless there is a clear link to both improved patient care and increased ROI. In my practice, I have had great success using Voco's Futurabond U universal adhesive and GrandioSO Heavy Flow flowable resin composite as the primary materials for attachment delivery.
The nice thing about Futurabond U is that it is, in fact, universal. Due to the ever-evolving world of adhesives, doctors have historically had a tendency to inventory more than one type of dental adhesive. For a while, this was necessary since many good adhesive systems also had their limitations, such as acid etching, sensitivity challenges, or missing ingredients for dual-phase curing and adhesion to all substrates. Futurabond U is a product that can satisfy all of a practice's adhesive demands. Its universality equates to reduction in inventory, standardization of clinical procedures, and simplification for staff-all of which lead to a better bottom line.
Similarly, GrandioSO Heavy Flow composite has many applications in clinical practice (beyond attachment delivery): small-cavity and pit-and-fissure restorations, repairs, splinting, lining of larger cavities, Class III and V restorations, and veneer cementation. Essentially, it's useful anywhere that a highly filled and less runny flowable composite is desirable.
Figures 10 through 14 show sequential steps to accomplish the delivery of attachments for a clinical case.
Figure 10 shows the template try-in to verify fit and accuracy, and more importantly, to identify the general location of each attachment across the facial surface of the given teeth. (Nos. 6 and 7 are shown in macro-photography for instruction.)
Figure 10
Figure 11 shows conditioning of the enamel with 37% phosphoric acid after nonfluoridated pumice scouring (for 20 seconds). Note that the etchant is not placed indiscriminately across the tooth but is placed in the appropriate attachment zones.
Figure 11
Figure 12 shows the application of Futurabond U to the involved surfaces, per the manufacturer's instructions, followed by thinning with an air stream.
Figure 12
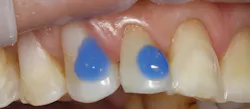
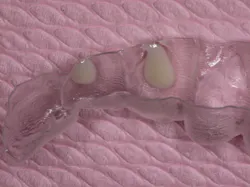
Figure 13 shows a section of the attachment template that was already preloaded with an appropriate shade and volume of GrandioSO Heavy Flow resin composite. The benefit of GrandioSO Heavy Flow is that it has the viscosity to stay in place without running out of the reservoir, yet it can also wet and adapt to the enamel wall seamlessly when the template is seated. For sequencing and delivery ease, the template is always loaded prior to the preparation of the tooth surface so that focus can remain on isolation once the intraoral steps are initiated. Experience also helps in determining the precise amount of resin to load into each reservoir, which ensures a complete attachment profile while avoiding excessive flash, saving time during finishing.
Figure 13
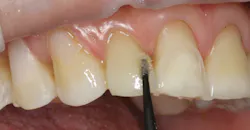
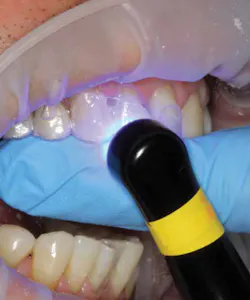
Figure 14 shows the template in place while the resin is light-cured. It's important to note that, while the majority of attachments are typically applied to enamel surfaces, there are exceptions. At times, a gingivally oriented attachment may be bonded at least partially to dentin, or a ceramic crown may be involved. Another benefit of Futurabond U is its excellent ability to bond to all natural tooth surfaces as well as ceramic and zirconia.
Figure 14
Conclusion
Aligner-based orthodontic therapy will be a mainstay in contemporary practice for the foreseeable future. When used to its fullest capacity, it can be a tremendous adjunct to both patient care and practice productivity. Like all other aspects of practice, efficiency and predictability are paramount to optimizing ROI. Nothing is more frustrating than having to repeatedly reapply lost attachments. Not only that, reapplication can cause patients to lose confidence and become less compliant. It is my hope that this article will expose readers to a new paradigm in adjunctive therapy and that it will serve as a reference for predictable, step-by-step attachment delivery.
Foroud Hakim, DDS, MBA, is a 1991 graduate of the University of the Pacific Arthur A. Dugoni School of Dentistry. He is in private practice in Northern California, and he also serves as clinical vice chair of reconstructive dental sciences at the University of the Pacific. He is a member of Catapult Group and Catapult Elite, the industry's preeminent speakers bureau.