Crown, onlay, or direct restoration?
A reader questions the number of dental crowns being placed on teeth that seem to be sound enough to have received tooth-colored direct restorations. Dr. Gordon Christensen offers his advice and discusses the merits of various methods of restoration for a particular case.
Q:
My question is related to something that frustrates me very frequently. It appears to me that for either esthetic or financial reasons, many dentists are placing crowns on teeth that seem to be sound enough to have received tooth-colored direct restorations. When does a tooth actually need a crown?
A:
I have observed the same problem. Even more ridiculous, I recently heard a nationally known dental speaker advocate crowns to his audience for every tooth that has had an amalgam in it. That statement is absurd to me. Is it related to an overt desire for better esthetics, or is it a devious way to make more revenue? In my opinion, far too many crowns are being done at this time.
My experience placing all types of restorations and observing them in all types of patients who have every level of oral hygiene goes back several decades. In my brief answer to you, I will relate my observations on tens of thousands of crowns and other restorations.
When is a crown indicated for a tooth?
There are two major considerations for placing a crown. Is the crown indicated because of esthetic or functional reasons?
If teeth are impaired esthetically, and the patient has a sincere desire to look more acceptable, the alternatives are bleaching (whitening), crowns, or veneers. If the teeth are acceptable functionally and only defective from an esthetic standpoint, bleaching or veneers are indicated. Bleaching is by far the best and least aggressive choice if that procedure is feasible.
If the lingual or occlusal surfaces are intact, the teeth are anterior teeth, the occlusion is not abusive, and caries is not a major problem, then veneers are the best solution. They can also be the best solution on some premolar teeth that are not in heavy occlusion.
If the teeth are either functionally unacceptable and/or both functionally and esthetically unacceptable, crowns are indicated.
When are teeth functionally unacceptable?
Extractions and resultant extrusion that requires the rebuilding of occlusion classify teeth as functionally unacceptable. A research project studying this concept would be practically impossible, since every clinical situation is somewhat different. What are some of the clinical situations that can necessitate crowns to rebuild new tooth contours, adequate esthetics, and occlusion? A few include:
- Biocorrosion and major loss of tooth structure caused by GERD or bulimia
- Caries causing significant tooth destruction
- Occlusal wear related to bruxism or clenching
- Inadequate ability for orthodontic tooth movement to produce adequate occlusion or appearance
- Movement of teeth due to periodontal disease, causing need for tooth rebuilding and recontouring
- Iatrogenic previous dentistry necessitating tooth rebuilding
- Endodontic access removing a major portion of the tooth
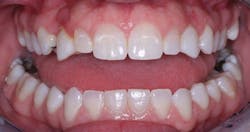
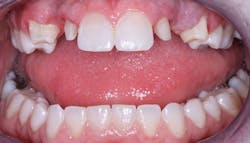
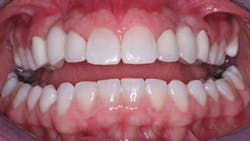
All of the above situations and many more necessitate tooth reshaping and rebuilding to establish adequate occlusal function and esthetics. Crowns are the obvious solution, assuming the patient has the financial resources to have the treatment accomplished (figures 1-3).
What are characteristics of a single tooth that necessitates a crown restoration?
I will omit the esthetic reasons and emphasize the functional and strength reasons for a single tooth crown restoration. It is interesting to note that large laboratories we work with report that 90% of the crowns they make are single crowns.
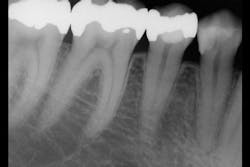
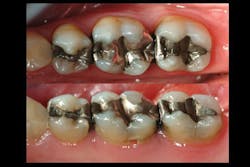
Observe Figures 4 and 5 for the following discussion:
The first molar has a painful, cracked distolingual cusp and lingual caries. Should the amalgam restoration be removed and another intracoronal restoration placed? I see this procedure routinely suggested by some clinicians who promote bonding of the remaining tooth structure to the subsequent direct or indirect restoration. My long-term clinical experience and in vitro research at Clinicians Report Foundation refute that recommendation. Such restorations are only a fraction as strong as a virgin tooth, and I strongly suggest that this procedure eventually results in a doomed restoration and tooth. When more than one-half of the cusp-tip to cusp-tip tooth structure is removed, the tooth has minimal strength remaining and a full-crown or onlay covering all of the remaining cusps is indicated.
Observe the second premolar. It has a deep base in it, but only minimal removal of tooth structure in the isthmus area. If this amalgam were to be replaced with another restoration, what would be appropriate?
- An intracoronal resin-based composite restoration would provide acceptable strength, assuming proper acid-etching of the remaining enamel walls is accomplished. Our in vitro research estimates that such a restoration is about 60% as strong as a virgin tooth.
- Is amalgam indicated? Apparently many dentists believe it is. A recent Clinicians Report Foundation survey of thousands of mostly North American dentists showed that 60% of them were placing amalgam up to 10% of the time. Personally, I have not placed an amalgam for many years and find that the following procedure satisfies the intracoronal restoration need for such a tooth. If the box form is deep, place resin-modified glass ionomer, such as 3M Ketac Nano, GC Fuji II LC, or Riva Light Cure HV (high viscosity) in the apical one-third of the box form, cure it, and place composite for the remainder of the restoration.
- How about an indirect inlay in this tooth? My clinical experience says no. Having placed many inlays and onlays on such teeth over several decades, there is no question as to which type of restoration fails most. Many of the inlays fail within a few years, while the onlays have far fewer failures. Should one cusp be left standing, bonded to an indirect restoration? Our research shows the restoration with a cusp standing alone is significantly weaker than a virgin tooth.
- What about an onlay on this tooth? If both cusps are covered with an onlay material such as IPS e.max, the strength has been shown scientifically to be greater than a virgin tooth. If cusps are left standing alone, the strength is far less than a virgin tooth. Except in rare cases, do not leave cusps standing alone, even though many clinicians promote this concept. If you want longevity for the restoration, cover the cusps.
- Is a crown indicated? For some of you who do not place onlays, a crown is a good choice. However, an onlay preserves the facial and lingual surfaces of the tooth, along with the original color of the tooth. Learn to do onlays. They can by beautiful, conservative restorations.
- In my opinion, if the second premolar restoration needed to be replaced, a well-placed resin-based composite would serve this patient for many years.
Now, observe the second molar. It is still serving well with a 20-year old amalgam in it. If it required replacement for some reason, the same rationale as described for the second premolar is acceptable. However, unless the patient does not desire to remove the amalgam, leave it for another many years. If the patient is concerned about the alleged challenges with amalgam, provide information about the amalgam controversy and let the patient be involved in the decision. The international research on large amalgam restorations shows about twice the longevity of composite in such sized restorations.
Summary
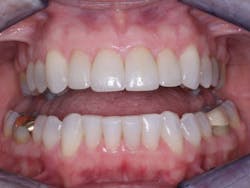
Making the decision whether to place an intracoronal restoration, an inlay, an onlay, or a crown is not a difficult one. The decision is made by considering the patient’s overall systemic and oral health characteristics, esthetic desires, and specific tooth characteristics. Currently available crowns are superb when done properly (figure 6); just don’t do them before they are indicated.
Gordon J. Christensen, DDS, MSD, PhD, is a practicing prosthodontist in Provo, Utah. He is the founder and CEO of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is cofounder (with his wife, Dr. Rella Christensen) and CEO of Clinicians Report (formerly Clinical Research Associates).
About the Author

Gordon J. Christensen, DDS, PhD, MSD
Gordon J. Christensen, DDS, PhD, MSD, is founder and CEO of Practical Clinical Courses and cofounder of Clinicians Report. His wife, Rella Christensen, PhD, is the cofounder. PCC is an international dental continuing education organization founded in 1981. Dr. Christensen is a practicing prosthodontist in Provo, Utah.