Implant stability prior to loading implant overdentures
Stability is the key to implant success. Initial mechanical stability is critical,1 and it is followed by all-important biologic stability, or osseointegration. Mechanical and biologic stability are closely related: a secure primary stability leads to a predictable secondary stability.2 For these reasons, it is paramount to know both the extent of initial stability and the point at which the bone has recovered from surgery and begun to heal. The information obtained from an Osstell IDx—specifically the implant stability quotient (ISQ)—can be used to accurately determine stability at the time of placement and later when a decision is being made whether or not to proceed with the restoration. In my own practice, this information is invaluable, as no two patients have the same bone quality, and no two patients heal at the same rate.
Primary stability
Primary stability can be determined by either torque value or evaluation of the ISQ, with ISQ being a more accurate predictor.3 The literature defines primary stability as 30 N/cm of torque. This refers to final seating torque, as opposed to insertion torque. There are many factors that affect torque, from the local environment of the osteotomy, to surgical protocol, to the micro- and macrostructure of the implant itself.
Primary stability is paramount during the healing process. It must be sufficient to enable the implant to resist micromovement until sufficient biologic stability, or secondary stability, is adequately established.4
Lateral and shearing movement between the implant and the surrounding bone must be kept below 150 microns to ensure that osseointegration occurs, rather than soft-tissue encapsulation and ultimate failure. Torque does not measure lateral stability, which is a useful indicator of successful treatment outcomes.5
The timeline of integration
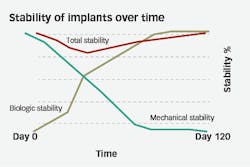
At initial insertion, implant stability comes entirely from the mechanical lock of implant in bone. This is contributed to by both the macrostructure of the implant and the quality of bone surrounding it. As time goes on, as long as the mechanical stability is not exceeded, the body will lay down bone through osteoblastic migration and bone maturation until the implant is stabilized and locked into place by the biological healing process, or osseointegration (figure 1). On average, integration takes three to four months to occur. However, this is just an average, with some patients integrating much faster and some taking much longer.
Figure 1: Mechanical versus biologic importance
The Osstell IDx
Because the torque value that is read on a wrench at placement does not take into account side-to-side shearing movements, another method must be used to ascertain the effect of mechanical stability of the implant and the quality of bone surrounding it. This is where resonance frequency analysis (RFA) technology provided by the Osstell IDx comes into play.
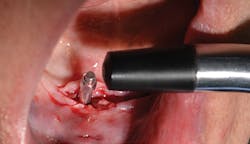
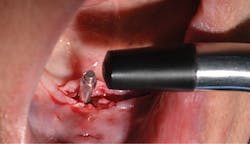
Figure 2: Smart peg and wand of IDx
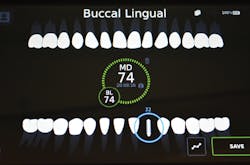
Figure 3: Screen of Osstell IDx with ISQ value
The device works as follows: An aluminum Smart Peg that has a magnet imbedded on top of it is inserted into the internal connection of an implant. Then, the wand or transducer of the IDx unit is brought into proximity of the peg (figure 2). The wand emits a magnetic frequency that vibrates the peg. The wand then picks up the returned frequency and converts it into an ISQ number (figure 3). The ISQ scale runs from 0–100. The more stable an implant, the higher the frequency and therefore the higher the ISQ number.
A simple way to conceptualize this process is to think of a metal pole driven into loose sand at the beach. If you hit the pole with a hammer, it will likely make a dull thud. This is because the sand does not afford much resistance to the pole being moved. The pole is analogous to the implant, and the sand is the surrounding bone. However, if you were to dig a hole in the sand, fill it with cement, put the pole in, and let the cement set, the pole would have a high frequency reverberation when hit with the hammer.
According to Osstell and the vast bank of clinical data it has compiled, an ISQ of 55–60 is considered primary stability.6 An ISQ of 70 is considered stable enough to load (figure 4).6
Figure 4: Clinical recommendations by Osstell
Case study
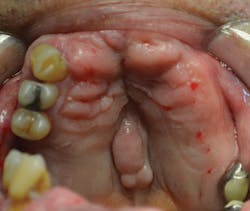
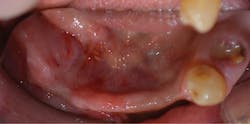
A healthy 72-year-old patient presented with failing dentition and maxillary and mandibular removable partial dentures (figures 5–7). After discussing treatment alternatives, it was decided to extract the remaining teeth and place four implants each in the maxilla and mandible to retain overdentures.
Figure 5: Intraoral maxilla pre-op
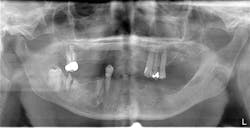
Figure 6: Pre-op panorex
Figure 7: Intraoral mandible pre-op
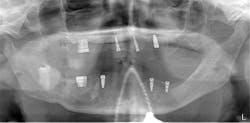
After the fabrication of full upper and lower immediate dentures, the patient underwent extraction of the remaining teeth and the placement of eight immediate dental implants (Hahn Tapered Implants, Glidewell; figure 8).
At the time of placement, ISQ readings were taken. Though the primary stability was high in these implants, the decision to allow them to integrate prior to loading was made, as each individual implant would be subjected to forces and they were not splinted. After insertion, 3-mm healing abutments were placed on all the implants except tooth No. 3, as that implant had a much lower initial stability reading. On the lower arch, 3 mm healing abutments were placed on all implants except for No. 22 due to stability. The dentures were relieved and delivered to the patient.
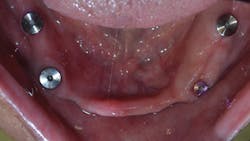
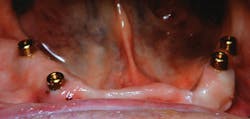
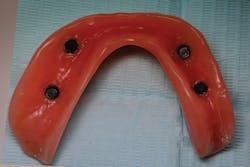
At one month, ISQ readings were taken of all the implants except No. 3. The lower arch showed the soft tissue healing at that time (figure 9). At 2.5 months, readings were taken again, and it was indicated that the mandibular arch had integrated and was ready for final attachment via locator attachments (Zest; figures 10 and 11). The maxillary implants were continuing to show progress, but not to the point where predictable loading was possible. Because the maxillary denture was stable (as most are), this was not an issue. The patient greatly appreciated the completion of the mandibular overdenture, which was very mobile and bothersome.
Figure 8: Post-op panorex
Figure 10: Locator abutments placed
At 13 weeks, the maxillary implants were again tested, and they showed adequate stability to load (figure 12). The implant in the No. 3 position was exposed and ISQ-tested at this time. A 3 mm healing abutment was placed, and the soft tissue was allowed to heal for two weeks (figure 13) prior to placing final abutments and retrofitting the maxillary denture with locator housings.
Figure 11: Retrofit of mandibular denture
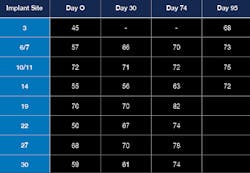
Figure 12: ISQ readings over time
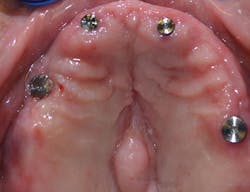
Figure 13: Maxillary arch with healing abutments
Conclusion
This patient demonstrated how different areas of the mouth had different rates of osseointegration. The restoring doctor was able to treat this patient in the most expedient and predictable manner.
The utilization of RFA technology, such as Osstell’s, is an important aspect of my practice. I test every implant I place at insertion and retest periodically throughout the healing process. It does not matter if it is a single unit, multiple unit, or a full-mouth fixed case.
This type of testing is also extremely important in overdenture cases, where a few implants must resist the movement and forces generated by a full arch of teeth. The majority of lateral and anterior-posterior movements ideally should be resisted by the hard and soft tissue by a well-made overdenture, but the reality is that the implants that are meant to just retain the denture will experience some load in both these directions.
In my opinion, as practitioners we should not put every patient into the same box. Why make a patient wait a generalized, prescribed time period, when they may integrate their implants at a faster pace? Conversely, why make the mistake of possibly loading any implant at the “magic four-month” time period, even though they may not have completely integrated? We do not use one-size-fits-all crowns, or say every patient will heal from an extraction in four weeks. Why assume every patient will integrate at the same rate? The bottom line is they do not. There is now a way to know when they are predictably ready to move on to the completion of their treatment. This is not only best treatment for your patients, but best practice for your office.
References
1. Schlesinger CD. Predictable immediate implant stabilization and restoration. Implant Adv Clin Dent. 2013;5:17-24.
2. Atsumi M, Park SH, Wang HL. Methods used to assess implant stability: Current status. Int J Oral Maxillofac Implants. 2007;22:743-754.
3. Schlesinger C. Torque vs. RFA in implant placement. Implant Practice US. August/September 2016.
4. Garber DA, Salama H, Salama MA. Two-stage versus one-stage—is there really a controversy? J Periodontol. 2001;72:417-421.
5. Swami V, Vijayaraghavan V. Current trends to measure implant stability. J Indian Prosthodont Soc. 2016;16(2):124-130.
6. Gahleitner A, Monov G. Assessment of bone quality: Techniques, procedures, and limitations. In: Watzek G ed. Implants in Qualitatively Compromised Bone. Chicago, Illinois: Quintessence, 2004:55-56.
Charles D. Schlesinger, DDS, FICOI, is a dental-implant educator who has lectured internationally for the past 11 years. In 2016, Dr. Schlesinger founded the CD Schlesinger Group LLC. The company strives to provide the very best in dental education, hands-on mentoring, and clinical support. He continues to provide comprehensive implant care to patients in a private practice setting in Albuquerque, New Mexico.