Minimally invasive thin veneers: Esthetics and longevity
Ross W. Nash, DDS
Debra Engelhardt-Nash
In 1997, I placed eight porcelain laminate veneers for a young woman who wanted lighter teeth without whitening procedures. Her oral health was excellent, and I was able to use thin veneers bonded to enamel on minimally prepared teeth to achieve her goal. Vita shade A1 was chosen by the patient in 1997. She was excellent with her home care and made nearly all of her recare appointments during the following years.
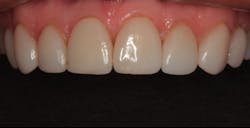
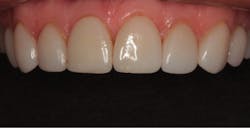
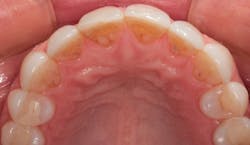
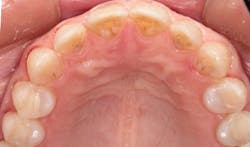
In 2016, she decided that she wanted to replace her veneers with the new bleach-shaded materials available today. In Figure 1, you can see her veneers as they appeared after nineteen years. Note the excellent tissue health and minimal tissue recession. There was a small fracture in the disto-incisal corner of the right central incisor. The incisal view at this date can be seen in Figure 2.
The process
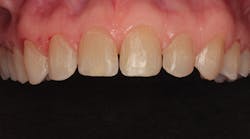
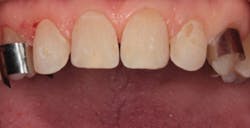
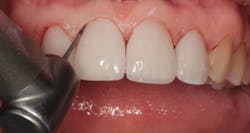
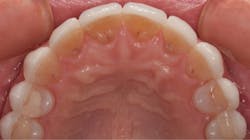
By carefully removing the veneers with fine diamond burs in a high-speed handpiece with water spray, I was able to minimize additional tooth structure removal, and no anesthetic was needed. Figure 3 shows the facial view after removal of the veneers. The incisal view can be seen in Figure 4. The patient decided that she wanted two additional veneers for her second premolars. Final impressions were taken, as well as a facebow record and occlusal registration. The patient chose Vita OM2 bleach shade as her desired color.
Figure 1: The patient’s porcelain laminate veneers placed in 1997 as seen in 2016
Figure 2: Incisal view of the patient’s porcelain laminate veneers placed in 1997 as seen in 2016
Figure 3: Facial view after removal of the veneers
Figure 4: Incisal view after removal of the veneers
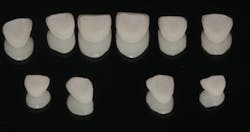
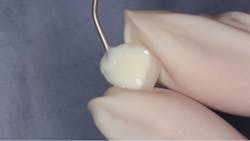
At dental laboratory, ten IPS e.max laminate veneers (Ivoclar Vivadent) were fabricated. They can be seen in Figure 5 photographed on a mirror surface. Notice the internal etched surfaces. As you can see in Figure 6, the veneers are very thin (approximately 0.3 mm).
Figure 5: IPS e.max laminate veneers after fabrication
Figure 6: Side view of an IPS e.max laminate veneer
The cementation procedure
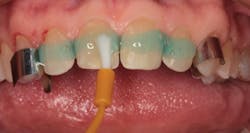
The veneers were bonded to place using a self-adhesive light-cured luting composite (Fusion-Zr Veneer Cement, Taub Products). The four incisors were isolated with thin metal strips and an enamel etching gel was placed on the prepared enamel surfaces (figure 7). The etching gel was rinsed thoroughly and the teeth were air dried. The etched enamel surfaces can be seen in Figure 8.
Figure 7: Etching gel placed on isolated incisors
Figure 8: Enamel surfaces after etching
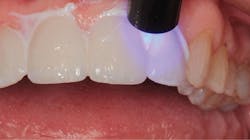
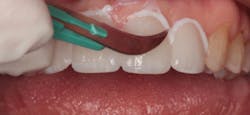
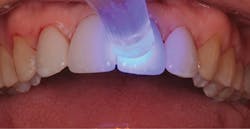
No bonding agent is needed for the enamel and no silane is needed for the ceramic with this self-adhesive cement. The “opal white” shade was chosen and placed on the intaglio surfaces of the veneers (figure 9). The four veneers were placed on the teeth and lightly seated. The marginal cement was spot cured for two seconds using a LED curing light (figure 10). The marginal cured cement was teased away using a number 12 surgical blade (figure 11). Interproximal resin was removed with dental floss. Light curing was then completed by using the LED curing light for 20 seconds on the facial and lingual surfaces of each veneer (figure 12). Excess cured resin was removed with a small carbide finishing bur (figure 13) and the margins were polished using a polishing cup (Enhance finishing cups, Dentsply Sirona).
Figure 9: Cement being placed on the intaglio surface of a veneer
Figure 10: Cement under a curing light
Figure 11: Marginal cement removal
Figure 12: Light curing during completion
Figure 13: Removal of excess cured resin
Practice management considerations: It’s not just a recall
The patient described in Dr. Nash’s case was a 19-year follow-up. That’s a long time for a patient to remain loyal to a practice. How does an office ensure the longevity of patients and enroll them in treatment? And how does the office avoid the “it’s just a recall” trap? Turning ordinary recare visits into extraordinary ones is the key to building a strong hygiene department and gaining additional treatment acceptance from existing patients.
It’s critical to allow enough time during the hygiene visit to have a treatment discussion with the patient. How that time is used to engage the patient in discussion about treatment is vital to gaining treatment acceptance. Social conversation is important to build rapport with the patient, but it should not overrun the appointment. Remember, he or she came for a dental appointment, not a social visit, although both are important components of the patient experience in your office.
Avoid an attitude of assumption or apathy toward discussing additional treatment for the patient during the hygiene visit. I’m referring to the approach that the patient is not interested (e.g., “I’ve told them about this before.”). If the hygienist doesn’t place importance on treatment diagnosed but not accepted, how can the office expect the patient to place importance on proceeding with care?
At the beginning of the visit, remind patients where they were when they started in your office and advise them of where they are currently. Then open the conversation about future treatment: “Let’s talk about where your dental health will be or where you want it to be three to five years from now.” This is a great opportunity to discuss treatment that has been previously recommended but is yet to be completed “Tell me what has prevented you from proceeding with your treatment?” is an open-ended question that invites conversation with patients about their outstanding treatment. Open the appointment with this discussion. This will prevent running out of time or the patient feeling the urge to get up and check out without these questions being asked. Waiting until the end of the visit is too late.
There is excellent patient engagement technology that can help the practice keep the patient connected to the practice through reactivation notices and newsletters. Working with companies such as Solutionreach, RevenueWell, and others can increase patient retention and reactivation efficiently and effectively for the office.—Debra Engelhardt Nash
The final result
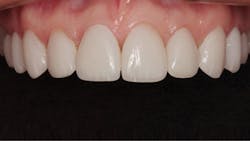
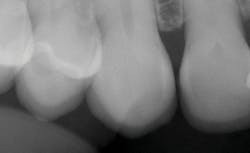
The new veneers are shown from the facial view in Figure 14 and incisal view in Figure 15. In the radiograph in Figure 16, the thin veneers can be seen in place. This case illustrated to me that thin veneers bonded to enamel have the potential to last for many years.
Figure 14: Facial view of the completed restoration
Figure 15: Incisal view of completed restoration
Figure 16: Radiographic view of the veneers in place
Ross W. Nash, DDS, maintains a private practice in Huntersville, North Carolina, where he focuses on esthetic and cosmetic dental treatment. He is an accredited fellow in the American Academy of Cosmetic Dentistry. Dr. Nash lectures internationally on subjects in esthetic dentistry and has authored chapters in two dental textbooks. He is cofounder of the Nash Institute for Dental Learning in Huntersville, North Carolina.
Debra Engelhardt-Nash is a trainer, author, presenter, and consultant, and has presented workshops, nationally and internationally, for numerous study groups and organizations. She is currently the vice-president/president elect for the National Academy of Dental Management Consultants, where she is a founding member and has served as president in the past. She was a contributing editor for Contemporary Esthetics and Restorative Practice magazine, Contemporary Dental Assistant magazine, and has written for a number of dental publications.