Let's you and me bond
Lisa L. Knowles, DDS
The smell of marijuana lingered in the operatory as I entered. "Who is buzzed?" I thought. "Is it my patient or the person with him?" My thoughts continued to wander. My patient, a 24-year-old male with severely decayed teeth and a Class III bite like no other, appeared cognitive, alert, and wide-eyed. His presumed girlfriend appeared supportive and interested.
As I perused my patient's medical history, I saw his indication of medical marijuana usage, so I asked him if he had used marijuana lately. "No," he replied. "Not since yesterday." I had just read an article in the May issue of the Journal of the American Dental Association about gaining consent from patients who are using illicit drugs.1 I could not help but wonder how the legal use of marijuana affects this type of decision making. Nonetheless, consent is consent, and I had my patient's consent today for the restorative and oral surgery procedures he needed. I did recognize our future need for a clearer consent form, and I will verbally prepare my patients for future treatment by reminding them not to use marijuana (if possible) within 24 hours of treatment to avoid the possible breach of consent.
ALSO BY DR. LISA KNOWLES | Microcommunication: Sweating the small stuff
Despite my patient's needs, I found it somewhat difficult to bond with him because of the potent smell of cannabis in the room. Furthermore, I am not sure how I feel about the legalization of medical marijuana. I see the benefits, and I see the problems. Yet, it is my job to treat everyone and bond with everyone from the moment they are in my hands and under my medical watch.
Another patient came to me with an inability to speak English. Her daughter accompanied her and acted as her interpreter. I watched my assistant struggle with the language barrier. She wasn't sure how to communicate with this patient. This inability to communicate led to frustration. "I don't know what else I can ask," she told me privately as she prepped me for the patient exam. She was having trouble bonding as well.
I think many of us have trouble bonding, whether it's with patients or the dental bonding agents we use.
So, when I was asked to try a new bonding agent- All-Bond Universal from Bisco-I viewed it as an opportunity to work on my bonding skills and think about things differently.
ALSO BY DR. LISA KNOWLES | Do you have symbiotic or life sucking relationships in your dental practice?
From a dental standpoint, I enjoy the flexibility All-Bond Universal offers. With composites, I can use it three different ways if I prefer. I can use it without etch and appreciate the self-etching properties it has. I can selectively etch the enamel if I so desire. Or I can opt for the total-etch route and cover the entire tooth with etch. Most doctors like to do things a certain way, and with two doctors in our practice space, we both can use it how we want to without having to purchase two different kinds of bonding agents.
I also appreciate the bond because of its thin viscosity. Some of the bonding agents I have used in the past were pretty thick, and I worried about clogging my proximal Class II boxes with thickened adhesive. That's not a problem with All-Bond. It's thin.
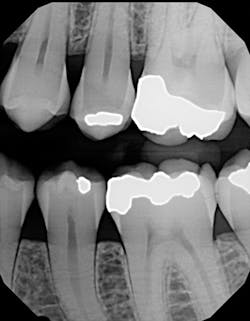
Figure 1: Cracked tooth x-ray
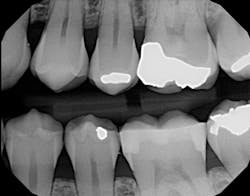
I used it on an elusive cracked tooth case. For once, I could actually see the fracture on an x-ray (figure 1). The noted distal fracture caused a great deal of biting pain for this patient. The one difference I noticed with All-Bond is its application method. Two coats are required and a scrubbing motion is needed during the two-coat process prior to curing. Yes, this is a little more time-consuming, but it did not bother me as much as I thought it might when I initially read the application directions. After I saw the results on the x-ray (figure 2), I knew the thin viscosity did not prohibit any type of condensed end product. The composite material flowed well into the proximal areas, and my patient left with no cracks in No. 19.
Figure 2: Restored cracked tooth x-ray
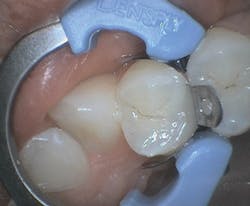
In another case, I used All-Bond Universal to fill a very typical Class II restoration for a female patient (figure 3). By this time, my assistant and I applied the bonding agent with ease and left the instruction sheet behind. Although I did not get to test All-Bond Universal's versatility with other procedures, I look forward to using it for indirect restorations in the future.
Figure 3: All-Bond Universal restoration
All-Bond Universal bonds to everything: metal, composite materials, lithium disilicate, and pretty much everything we need to bond. It truly is universal in nature.
So what about us? Are we able to bond to everything—or should I say everyone?
We are challenged to please so many patients with so many emerging needs. We want superior bonding materials to help us with every problem we encounter; we want a universal solution. We don't want to have to think about every step to get a good result. We want our procedures to be easier. Wouldn't that be wonderful as we encounter patients?
It appears the technology is here to help us solve the bonding of materials problems that we experienced in the past. Now, what about our abilities to bond with the patients we treat? What about those with the smell of marijuana seeping from their clothing? What about patients with special needs and language barriers? How do we manage to bond with all of these different kinds of people universally?
I believe we can look to companies like Bisco and do what they have done . . . evolve. It took several generations of perfecting original products. We may stumble at first, and we may need to observe others who have better ways of doing things. This normal progression to a better end result is equally applicable to how we treat each patient in our care. It may seem strange initially to treat a patient with a different gender identity or a different ethnic background, but with a desire to do no harm to others and a desire to improve our end results, we can intentionally bond with those in need of our services-no matter how they come to us.
The technology is here to respond to a universal need. Are we ready to respond to universal needs? With some practice I think we are, and with products such as All-Bond Universal we can worry less about products bonding properly and focus more on bonding with our patients.
Further reading
• How long does marijuana (THC) stay in your system? Mental Health Daily website. http://mentalhealthdaily.com/2015/10/04/how-long-does-marijuana-thc-stay-in-your-system/. Published October 2015.
• Stogner JM, Miller BL. Assessing the dangers of 'dabbing': mere marijuana or harmful new trend? Pediatrics. 2015;136(1):1-3. doi: 10.1542/peds.2015-0454.
Reference
1. Grafton SE, Huang PN, Vieira AR. Dental treatment planning considerations for patients using cannabis. J Am Dent Assoc. 2016;147(5): 354-361. doi: 10.1016/j.adaj.2015.11.019.
Lisa L. Knowles, DDS, founded IntentionalDental Consulting to help guide others to a more purposeful life. In her 15 years as a dentist, she has lived dentistry, loved dentistry, and loathed dentistry. Her contribution to the profession is an ability to look at the whole picture-from foundational communication needs to clinical provider shortcomings. Dr. Knowles practices in St. Johns, Michigan, and helps teach a communication course at the University of Detroit Mercy School of Dentistry. Contact her at [email protected], and follow her blog at Beyond32Teeth.com.