When should teeth be removed?
Q: I am a relatively new practitioner, and the past five years of practicing dentistry have been exciting and challenging. I have a question that continues to frustrate me. I have a difficult time deciding when to place a liner or base in a tooth preparation and restore it, accomplish endodontics on a tooth, or remove the tooth. Are there some finite suggestions you can provide for me?
A: Your question is difficult to answer, since there are many variables that relate to making the decision to remove teeth. Some of them are: the age of the patient, occlusion, location of the tooth in the mouth, oral hygiene, how much supra-bone tooth structure is present, presence of moderate-to-severe periodontal disease, extreme caries involvement on most of the remaining teeth, and the financial status of the patient. I will provide information on some of the major characteristics that will help you decide the answers to your questions.
The patient should receive thorough informed consent about any of the following conditions and the chances for successful treatment. The patient should be included in making the decision on whether or not to retain the teeth. If teeth are questionable, a joint decision made by the dentist and the patient should be agreed upon before deciding to retain or remove the teeth.
Related reading:
Age of the patient
This is an important consideration that relates to numerous other limiting factors. Consider the following examples: If the affected tooth is a second or third molar in an older person, and the patient’s financial situation is not good, removal of the tooth is probably indicated. If a tooth is symptomatic and the root canals are almost nonexistent, endodontic treatment may be contraindicated, and an apicoectomy or tooth removal could possibly be indicated. Additionally, if the carious lesion is large and close to the pulp, the tooth may or may not be nonvital, and a base or liner in the deepest portion of the tooth preparation may do no good because of a nonvital pulp. Determination of tooth vitality should be accomplished before treatment. In all of the previous situations, a candid discussion with the patient about the negative and positive characteristics of the tooth is in order.
Occlusion
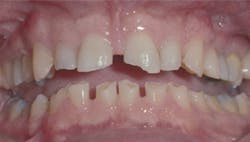
This factor is related to almost every clinical procedure we accomplish (figure 1). Heavy bruxing or clenching causes excessive tooth wear, tooth and restoration breakage, tooth mobility, and places extreme forces on the teeth and restorations. If the involved tooth is compromised in any other way, heavy occlusion can be an extremely negative factor concerning whether or not to retain the tooth.
Figure 1: This clenching bruxer is not a good candidate for conservative restoration of teeth. Heavy occlusion is almost always a negative condition for retention of suspicious teeth.
Oral hygiene
Questionable oral hygiene with other significant compromising factors may also indicate that the tooth should be removed. In such cases, a successful attempt to improve oral hygiene may allow salvage of the tooth.
Amount and condition of remaining supra-bone tooth structure
This factor is an extremely important one related to long-term survival of the tooth. Well-recognized and research-supported conclusions among dentists follow relative to how this factor influences whether to remove or retain a tooth.
Teeth with no tooth structure coronal to the gingiva are poor candidates for retention without endodontic treatment, a post and core, probably some titanium anti-rotation retentive pins, and a crown. Even when these procedures are carried out, the long-term viability of this compromised tooth is suspect.
Teeth with no tooth structure coronal to the bone level are definitely not good candidates for retention. With only a few exceptions, I recommend removal of such teeth. If the teeth have long roots, orthodontic extrusion may be accomplished, but that technique is seldom accomplished in real-world practice.
Large, previously placed defective restorations on either vital or endodontically treated teeth that comprise half or more of the remaining supra-bone tooth structure may or may not allow predictable tooth restoration with either a large direct restoration or a crown.
Cracked teeth are commonly encountered. For both physiologic and esthetic reasons, a painful crack that extends subgingivally can compromise your ability to save the tooth. It is nearly impossible to determine if the crack extends beneath the bone until the soft tissue is lifted away from the bone. If the crack extends below the bone on the facial surface, the restoration will be compromised esthetically because surgical crown lengthening will be necessary. A crack into the pulp or segregation of the tooth into two segments almost always condemns the tooth. Careful evaluation of cracked teeth is necessary before deciding upon tooth retention or removal.
Endodontically treated, heavily restored teeth require careful evaluation of the endodontic acceptability before keeping or removing them. If the endodontic procedure is questionable, redoing treatment is sometimes successful. A waiting period of several weeks to determine the acceptability of the redo is suggested. In such cases, removal of the previously placed restoration and placement of a buildup or post and core are recommended. A crown is usually necessary to provide predictable service expectations for such teeth. They are usually only fair candidates for long-term success.
Teeth with a cusp or cusps broken off often do not have enough tooth structure remaining to allow predictable restoration without endodontic treatment. In such cases, placement of a post and core followed by a crown is needed. However, sometimes placement of an onlay or crown will provide adequate strength and retention without endodontic treatment. Many patients cannot afford this relatively expensive treatment, necessitating tooth removal.
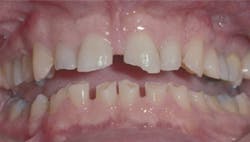
Figure 2: This patient has periodontal pockets that are 6 mm and more in depth. Gross carious lesions are also present. Salvage of his teeth is probably not a viable alternative.
Periodontal disease
Patients with moderate-to-severe periodontal disease and teeth mobility require thorough education about periodontal disease and its ongoing, consistent destruction of the periodontal structures (figure 2). If the patient accepts the necessity of having periodontal therapy, some of the teeth can be saved. If not, tooth removal is probably the best alternative.
Caries present in most of the teeth
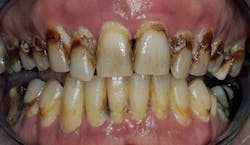
Often, patients are examined who have severe caries on most of their teeth (figure 3). This type of patient needs in-depth education about the reason for the extreme caries, the necessity for a major behavior change if the teeth are to be retained, the potential restoration possibilities and expense involved, and the requirement for close follow-up and recare appointments upon completion of treatment. In most cases, removal of the teeth is the most responsible decision. Drastic changes in human behavior are almost impossible to accomplish.
Patient financial status
If the patient has extremely limited financial resources, teeth that are adequate for salvage often must be removed. This is an unfortunate situation, and I suggest that dentists attempt to encourage patients to find the finances for tooth retention if possible. The following procedure is often successful if the patient is really motivated to retain the teeth:
• Diagnose and treatment plan the patient.
• Determine which teeth need immediate restoration.
• Depending on financial availability, restore the most severely involved teeth first, allowing the patient to recover financially before proceeding with the less-involved teeth.
• If the patient cannot afford long-term treatment, place glass ionomer restorations in the most severely involved teeth. New, improved conventional glass ionomer restorative materials—such as 3M Ketac Universal, GC Equia Forte, or Voco IonoStar Plus—are indicated for an interim period until final restorations can be completed.
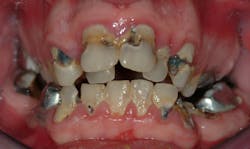
Figure 3: This young patient has severe caries, malocclusion, and moderate periodontal disease. He is not a good candidate for retention of teeth.
Summary
Despite the popularity of implants, many fail, and there is nothing like a tooth. I suggest retaining teeth for as long as your clinical expertise and the patient’s behavior allow. This article shares my experience about retaining teeth for as long as possible. Of course, there are many times when that cannot be done, and tooth removal becomes necessary.
Author’s note: The following educational materials from Practical Clinical Courses will offer you and your staff more insight on the topic of when teeth should be removed.
One-hour videos:
- Treating the Aging Population—A Frustrating Challenge (Item No. V4777)
- Class II Composite Resins Can Be Practical, Non-Sensitive, and Profitable (Item No. V3554)
Two-day hands-on course:
- Restorative Dentistry 2—Fixed
Prosthodontics with Dr. Gordon
Christensen
For more information about these
educational products, call (800) 223-6569
or visit pccdental.com.
Gordon J. Christensen, DDS, PhD, MSD, is a practicing prosthodontist in Provo, Utah. He is the founder and CEO of Practical Clinical Courses, an international continuing education organization founded in 1981 for dental professionals. Dr. Christensen is cofounder (with his wife, Rella Christensen, PhD, RDH) and CEO of Clinicians Report.
About the Author

Gordon J. Christensen, DDS, PhD, MSD
Gordon J. Christensen, DDS, PhD, MSD, is founder and CEO of Practical Clinical Courses and cofounder of Clinicians Report. His wife, Rella Christensen, PhD, is the cofounder. PCC is an international dental continuing education organization founded in 1981. Dr. Christensen is a practicing prosthodontist in Provo, Utah.