Laser-assisted restorative dentistry: Can we afford not to use it?
Marina Polonsky, DDS, MSc
Running a private dental practice presents many challenges, but also provides us with numerous benefits. The challenges include keeping up with new technology and postgraduate educational requirements in order to stay current and to provide the best and latest treatment options to our patients. Decisions as to which are the best technologies to invest in, which we often make early in our careers, determine the way we practice during our formative and most productive years. It is because of these decisions that we create our loyal and happy patients. They are the cornerstone of any successful dental practice, from their referrals and web-based reviews to the revenue they bring to help our practices grow. Their smiles and gratitude following a painless procedure make the effort worthwhile.
Since the invention of the first laser in the early 1960s, this technology has slowly but surely infiltrated most fields of medicine and dentistry. Although erbium lasers have been approved for surgical and restorative procedures on teeth and bone since the 1990s, their penetration into dental practices remains at around 5%.1 This low number is a result of little to no introduction of this technology in dental school curricula, as well as the significant financial investment and the lengthy learning curve, which leaves a lot of dentists frustrated. However, if we had the drive to learn how to use this technology to its fullest potential, and if the investment could be justified by guaranteed patient satisfaction, it would inevitably lead to increased practice growth. Every office would have an all-tissue laser in every operatory.
The positive patient experience rests on the elimination of the “4 S” anxiety triggers: sight, sound, sensation, and smell.2 The sight is seeing the drills and local anesthetic syringes with needles; the sound is the high-pitched noise of the drills; the sensation is the vibration of the dental drill, in particular the slow-speed turbine. The smell is the only sensation we were successful in eliminating by using high-volume suction and water spray. The all-tissue dental laser system, like the Waterlase iPlus or Express by Biolase, can remove hard tissues (e.g., enamel, dentin), with minimal thermal side effects, which is similar to the performance of a high-speed dental turbine with water spray.3 Unlike the conventional high-speed bur preparation, this type of laser system has been shown to produce 400 times less vibration,4 achieving an improved patient experience, as evidenced by a number of pediatric studies.5–9
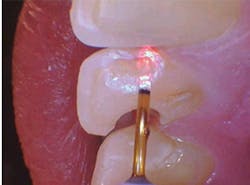
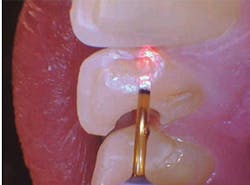
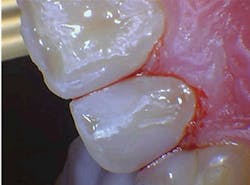
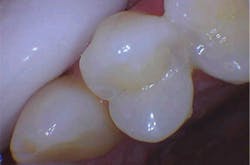
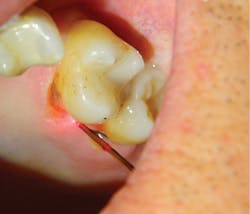
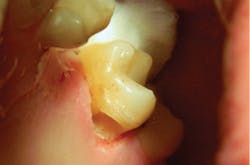
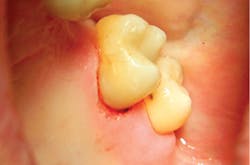
The depth of penetration (at only 25 microns in hard tissues) allows for precision with respect to the safety of the surrounding healthy tissues, adjacent teeth, and gingiva, and insurance against unexpected patient movements. While the drill will continue to spin if the patient moves, creating possibility of unintended injury, the same slight movements by the patient will bring the laser tip out of focus, rendering it harmless (figures 1a and 1b).
Figures 1a and 1b: A Class III anterior cavity preparation
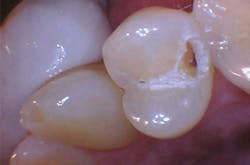
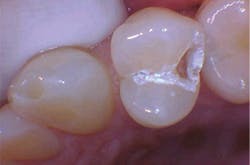
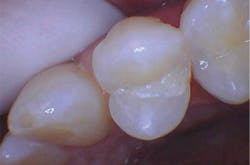
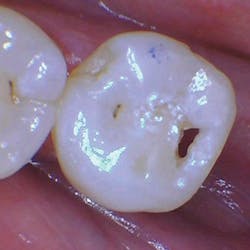
The removal of dental hard tissue is accomplished by what is known as thermomechanical photon-induced water-mediated ablation, which is a process in which the micro-explosive force of photons on water droplets results in the selective removal of carious dentin (figures 2a–2d). The laser energy seeks out tissue with higher water content, such as a carious lesion, and evaporates it without contact, vibration, or the introduction of microfractures, leaving the surrounding healthy enamel and dentin intact.
Figures 2a–2d: A Class II posterior cavity preparation
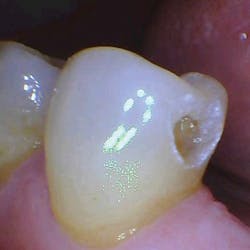
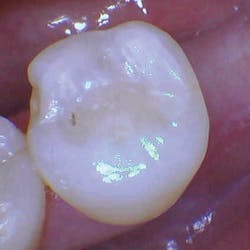
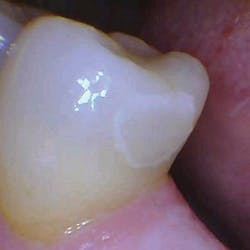
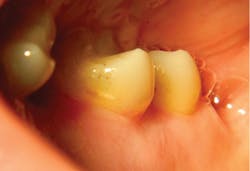
With the help of magnification, we are able to prepare small Class II lesions without sacrificing the marginal ridge, ensuring the longevity of our restoration and maximizing the remaining tooth structure with this minimally invasive approach (figures 3a–3d).
Figures 3a–3d: Minimally invasive Class II preparation with marginal ridge preservation
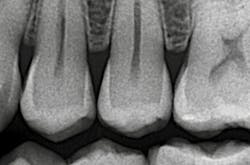
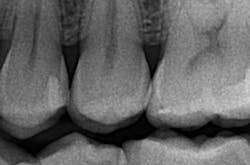
Although the radiographic appearance of these restorations is somewhat unfamiliar, they show long-term success (figures 4a–4b).
Figures 4a and 4b: Radiographic appearance and four-year follow-up of minimally invasive Class II tunnel cavity preparation on tooth 12D
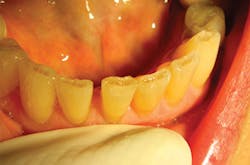
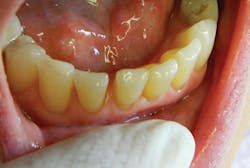
The noncontact technique enables restoration of delicate areas, such as worn incisal edges of lower anteriors, which often absorb stain over time and cause cosmetic concerns for many patients. The lack of collateral damage when using a laser (unlike the microfractures created by the vibration of a drill), and the ability to create convergence toward the incisal simply by changing angulation of the laser tip from buccal to lingual, provide both macro- and microretention, and hence, the longevity of these restorations (figures 5a and 5b).
Figures 5a and 5b: Class VI anterior incisal attrition restoration
In the last 10 years, numerous studies have been published showing reduced pain perception and improved patient acceptance of laser cavity preparations with Er,Cr:YSGG pulsed laser systems.10,11 A recent clinical study that included 400 cavities prepared in over 300 patients reported an overall 85% pain-free experience during laser cavity preparation using an Er,Cr:YSGG laser system.12 Anterior teeth prepared with lower power settings are successful without anesthesia in over 95% of the cases.12 Although the speed of laser-assisted hard tissue removal is slower, this time is made up because no time is spent waiting for the onset of anesthesia. The lack of collateral soft-tissue numbness, often lasting for hours after completion of the procedure, turns your patients into your greatest fans.
Lastly, it is very important to consider a laser’s water absorption. By providing plenty of water on the tooth surface, we can safely remove hard tooth structure with great visibility and precision. The flip side is that by reducing water supplied at the soft-tissue surface, we are able to sculpt gingival tissue while maintaining coagulation without deep thermal penetration—the laser penetrates only 2.3 microns in soft tissues. This results in a clear surgical field and also enables us to perform subgingival Class V restorations and gingival recontouring in the same appointment, with minimal postoperative discomfort. Restoring difficult clinical scenarios, such as external resorption (figures 6a–6d) is no longer a problem.
Figures 6a–6d: Gingival recontouring and restoration of Class V external resorption lesion in the same appointment
References
1. Internal data from Biolase.
2. Hmud R, Walsh LJ. Dental anxiety: causes, complications and management approaches. J Minim Interv Dent. 2009;2(1):67-78.
3. Cavalcanti B, Lage-Marques J, Rode S. Pulpal temperature increases with Er:YAG laser and high-speed handpieces. J Prosthet Dent. 2003;90(5):447-51.
4. Takamori K, Furukawa H, Morikawa Y, et al. Basic study on vibrations during tooth preparations caused by high-speed drilling and Er:YAG laser irradiation. Lasers SurgMed. 2003;32(1):25-31.
5. Olivi G, Genovese MD. Laser restorative dentistry in children and adolescents. Eur Arch Paediatr Dent. 2011;12(2):68-78.
6. Daneswari V, Nandlal B. Restorative dentistry for children using a hard tissue laser - a review. J Int Oran Health. 2011;3(3):1-8.
7. Liu JF, Lai YL, Shu WY, Lee SY. Acceptance and efficiency of Er:YAG laser for cavity preparation in children. Photomed Laser Surg. 2006;24(4):489-493.
8. Eren F, Altinok B, Ertugral F, Tanboga I. The effect of Er,Cr:YSGG laser therapy on pain during cavity preparation in paediatric dental patients: a pilot study. Oral Health Dent Manag. 2013;12(2):80-84.
9. Boj J, Galofre N, Espana A, Espasa E. Pain perception in pediatric patients undergoing laser treatments. J Oral Laser Applications. 2005;5(2): 85-89.
10. Matsumoto K, Hossain M, Hossain I, Kawano H, Kimura Y. Clinical assessment of Er,Cr:YSGG laser application for cavity preparation. J Clin Laser Med Surg. 2002;20(1):17-21.
11. Eren F, Altinok B, Ertugral F, Tanboga I. The effect of Er,Cr:YSGG laser therapy on pain during cavity preparation in paediatric dental patients: a pilot study. Oral Health Dent Manag. 2013;12(2):80-84.
12. Polonsky M, Gutknecht N, Franzen R. Review of possible predictors for pain perception with class 1-5 cavity preparations using Er,Cr:YSGG laser: a retrospective clinical in vivo study. Laser Dent Sci. 2017;1(1):9-21.
Marina Polonsky, DDS, MSc, is a gold-medal University of Toronto 1999 graduate and maintains a private general practice in Ottawa, Canada, with a focus on multidisciplinary treatment utilizing lasers of different wavelengths. She holds a mastership from World Clinical Laser Institute, and a master of science in lasers in dentistry from RWTH Aachen University. She is the founder of the Canadian Dental Laser Institute. Dr. Polonsky is a key opinion leader and clinical mentor for Biolase.