Pain management without opioids
Ian Shuman, DDS, AFAAID, MAGD
Virtually everyone in the general public and in the health-care profession is aware of the opioid crisis in the United States. Many dentists and physicians have responded by scaling back on the number of prescriptions being written for drugs such as hydrocodone and oxycodone. There was a time when these drugs were widely prescribed, especially for the emergency patient and postoperative minor oral surgery. The commonly used alternatives include 600–800 mg of ibuprofen together with, or alternating with, 325 mg of acetaminophen. These OTC pain medications are adequate for many patients, but not all. However, there appear to be few nonopioid alternatives for patients whose pain level cannot be managed with nonsteroidal anti-inflammatory medications.
Dentistry is substantially a procedure-based profession in which teeth and gums are invasively manipulated on a daily basis. This is very different from the cognitive-based medical profession and the day-to-day activities of the primary care physician (PCP), for instance, in which the doctor diagnoses the patient’s problem and writes a prescription or provides a referral. Very few procedures are performed in the PCP’s office. There is also a significant difference in the types of pain commonly encountered in dentistry and medicine. The dentist deals with patients who are in acute pain of varying severity and duration on a daily basis—not the chronic pain that physicians treat.
With these issues in mind, dentists require nonopioid analgesics to prescribe for patients that provide pain relief at the opioid level. Following are three alternatives that dentists can consider.
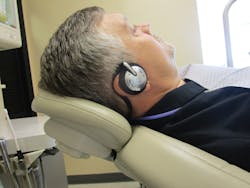
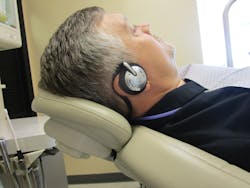
Figure 1: Music delivered through wireless headphones has been shown to be effective in reducing the perception of pain.
Ketorolac tromethamine
One such drug, ketorolac tromethamine (Toradol, Sprix), is an NSAID that was developed and approved by the FDA in 1989. This class of drug does not carry the addiction liability of narcotics, has a rapid onset of action, and is effective for a significant period of time for patients who are experiencing acute pain. It is available in injectable form for IV and intramuscular usage, as well as oral and intranasal forms. It was approved in 2010.
Ketorolac tromethamine is indicated for short-term relief (up to five days) of moderate to moderately severe pain. Intranasal ketorolac is widely used by pain management physicians, anesthesiologists, and surgeons, and is rapidly gaining popularity among dental prescribers.
The full prescribing information, side effects, and drug interactions are available online. Ketorolac tromethamine can be ordered by prescription from a specialty pharmacy, needs to be refrigerated, and must be ordered in advance. When a patient presents in significant pain, a different analgesic would be used. However, the majority of potentially pain-inducing procedures are scheduled, including oral surgical procedures such as extractions and implant placement, endodontic procedures, and periodontal surgery.
Audio-analgesia
Professional interest in the use of audio-analgesia first appeared in the Journal of the American Dental Association in October 1961. In August 2015, the Lancet published a systematic review of more than 4,200 articles, including 73 controlled trials, that concluded: “Music could be offered to help patients reduce pain and anxiety during the postoperative period. Music is a noninvasive, safe, and inexpensive intervention that can be delivered easily and successfully in a hospital setting. We believe that sufficient research has been done to show that music should be available to all patients undergoing operative procedures.”1
This is not simply a matter of providing music or Muzak that will vary in tempo and volume. Patients who bring their own music devices may be distracted during a procedure, but without the benefit of the rhythmic entrainment.2Rhythmic entrainment is “defined by a temporal locking process in which one system’s motion or signal frequency entrains the frequency of another system. This process is a universal phenomenon that can be observed in physical (e.g., pendulum clocks) and biological systems (e.g., fireflies). However, entrainment can also be observed between human sensory and motor systems.”3
In this regard, audio-analgesic music provides a specific beat that is fed directly to the brain through the eighth cranial nerve. A September 2016 study in the Journal of Endodontics describes the use of specific music and its effect on blood pressure and heart rate. In the study, the effects of certain musical frequencies were an invaluable adjunct to prescription medications during endodontic therapy.4
Alice Cash, a PhD musicologist, was granted a patent for having selected specific music, specific tempo, and specific frequencies capable of inducing rhythmic entrainment. This prerecorded playlist has been used in hospitals, including the Cleveland Clinic, Mayo Clinic, and Veterans Administration systems, among others.
In a 2016 clinical study in a VA hospital conducted by a University of Louisville School of Medicine team, the music, delivered through a wireless headphones device (Surgical Serenity Solutions) and measured by the visual analog scale, was effective in reducing the perception of pain by 20% in male patients after abdominal surgery.5
Inducing rhythmic entrainment in this way has been shown to reduce stress, as well as the amount of anesthetic and prescription drugs required before, during, and after surgical procedures, as it synchronizes respiratory and cardiac functions to that of the normal resting heart rate.
The product is offered in a “hospital” model with disposable ear-pad covers, for repeated use in the surgical suite or dental operatory, for overanxious patients, for prolonged procedures such as endodontics, multiple extractions, and longer surgical procedures (figure 1). A patient take-home unit is also available that can be given or sold to patients who will be undergoing repeated treatments and will have a longer recovery period, such as dental implants or periodontal surgeries. Both units are designed to be out of the way of the treatment team.
Ice
The use of ice to reduce pain and swelling has been around for many years, and experience demonstrates that it is very effective for a variety of musculoskeletal injuries and conditions. The reduction of pain and swelling are both achieved when ice is used singularly or serially and with varying durations.
A 2013 study by Kuo et al. suggested that ice pack therapy for 10 minutes effectively reduces pain and partial swelling.6 The authors did indicate that the duration of ice pack therapy should be modified according to the individual. One of the major benefits of ice is the absence of side effects. Ice has been shown to be an effective analgesic in a wide variety of situations, including chronic conditions such as arthritis and acute situations such as sports injuries, slip-and-fall injuries, and postoperative swelling, among others.
References
1. Hole J, Hirsch M, Ball E, Meads C. Music as an aid for postoperative recovery in adults: a systematic review and meta-analysis. Lancet. 2015;386(10004):P1659-P1671. doi:10.1016/S0140-6736(15)60169-6.
2. Prensner JD, Yowler CJ, Smith LF, Steele AL, Fratianne RB. Music therapy for assistance with pain and anxiety management in burn treatment. J Burn CareRehabil. 2001;22(1):83-88; discussion 82-83.
3. Thaut MH, McIntosh GC, Hoemberg V. Neurobiological foundations of neurologic music therapy: rhythmic entrainment and the motor system. Front Psychol. 2014;5:1185. doi:10.3389/fpsyg.2014.01185.
4. Di Nasso L, Nizzardo A, Pace R, Pierleoni F, Pagavino G, Giuliani V. Influences of 432 Hz music on the perception of anxiety during endodontic treatment: a randomized controlled clinical trial. J Endod. 2016;42(9):1338-1343. doi:10.1016/j.joen.2016.05.015.
5. Varbanova MR, Neamtu A, Gaar E, Grigorov MV. Music reduces postoperative pain perception in male patients after abdominal surgery under general anesthesia. Int J Anesth Res. 2016;4(6):272-277. doi:10.19070/2332-2780-1600058.
6. Kuo CC, Lin CC, Lee WJ, Huang WT. Comparing the antiswelling and analgesic effects of three different ice pack therapy durations: a randomized controlled trial on cases with soft tissue injuries. J Nurs Res. 2013;21(3):186-194. doi:10.1097/jnr.0b013e3182a0af12.
Ian Shuman, DDS, AFAAID, MAGD, maintains a full-time general, reconstructive, and esthetic dental practice in Pasadena, Maryland. Since 1995, he has lectured and published on advanced minimally invasive techniques. He has taught these procedures to thousands of dentists and developed many of the methods. Dr. Shuman has published articles on topics including adhesive resin dentistry, minimally invasive restorative dentistry, cosmetic dentistry, and implant dentistry. He is a fellow of the Pierre Fauchard Academy.