Clinical case studies: A streamlined dental cementation protocol for low-retention restorations
Indirect restorations, including porcelain veneers, crowns, and fixed dental prosthetics (FDPs), have endured with great success as one the most prevalent modalities for individuals seeking to correct functional and cosmetic intraoral conditions.1 Resistance to dislodgment remains a key objective for full-coverage tooth preparations;2 however, the frequently encountered overreduction of tooth structure when replacing existing dental restorations presents less-than-ideal situations in obtaining maximum retention. Achieving clinical success when presented with limited natural tooth anatomy may be aided by self-adhesive resin cements (SACs). These bonding agents combine the benefits of additional working time with the mechanical properties of light-cure and chemical-cure resin cements.3 The high bond strength, fracture toughness, low solubility, and simplified application protocols of contemporary SACs makes their utilization in the cementation of compromised indirect restorations an appealing treatment option for clinicians.4
The gamut of currently available SACs on the market may pose a daunting decision-making task for the practitioner.5 To address the practical need for a streamlined material inventory and simplified cementation protocol, a newly developed SAC and accompanying Adhesive Enhancing Primer (G CEM One + AEP, GC America) were developed. The following four case studies demonstrate the variety of day-to-day applications this novel SAC/primer combination possesses for a variety of indirect restorations in wide-ranging clinical scenarios.
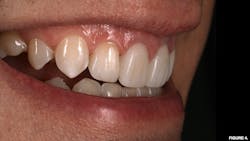
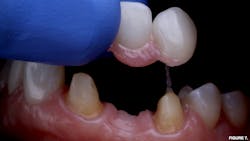
Case no. 1: Emergency recementation of debonded feldspathic veneer
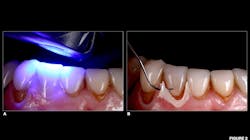
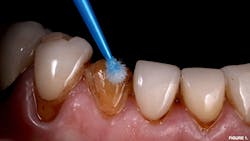
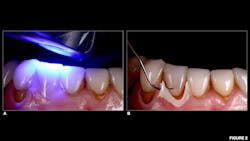
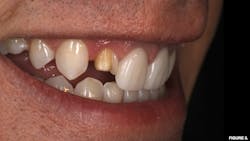
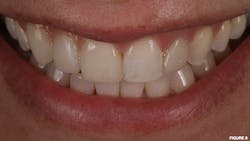
A 67-year-old female presented for emergency care regarding a dislodged feldspathic veneer on tooth no. 27. An intraoral examination revealed that the veneer had fully debonded with no fracture to the restoration, and an aggressively prepared mandibular right canine was devoid of enamel.
Case no 2: Full-coverage lithium disilicate crown
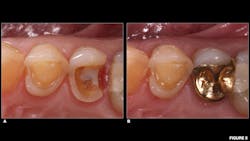
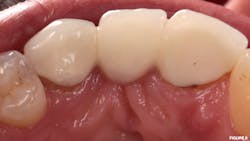
Case no. 3: Cast-gold onlay
A 55-year-old male presented with a fractured restoration and recurrent decay under tooth no. 13. The patient has a history of bruxism coupled with extrinsic dietary chemical erosion. A treatment plan was made to replace the failing amalgam with a partial-coverage cast-gold onlay, which would aid in the preservation of tooth structure and provide a good long-term prognosis. Metal-ceramic crowns and restorations composed of cast-metal alloys are unable to form a trueAll existing restorative material and recurrent decay were removed from tooth no. 13. The axial walls and pulpal floor of no. 13 were then refined with fine diamond burs in a high-speed handpiece to ensure a single path of draw and to maximize retention for the definitive cast-gold restoration (figure 5). To ensure maximum adhesion of the resin cement to the underlying tooth structure, an identical protocol was followed from the previous case studies in which an SAC was used in conjunction with an AEP. Following delivery of the cast-gold restoration, the patient’s occlusion was evaluated, and all adjustments were made with rubber polishing points. The patient was satisfied with the fit and function of the final restoration and dismissed without issue.
Case no. 4: Three-unit layered zirconia FDP
Conclusion
These four case studies have demonstrated that the use of SACs in combination with a unique AEP can aid in the predictable delivery of many types of indirect restorations with limited tooth structure by providing the following clinical advantages: reduced need for fricative macroretention,12 avoidance of composite buildups, and elimination of unnecessary endodontic therapy for post and core placement.13
Clinicians who choose to utilize SACs in their clinical practice will appreciate the ease of application and cleanup as well as a peace of mind in knowing that a strong, reliable bond with reduced microleakage14 and high retention has been achieved for their patients.15
Editor's note:This article appeared in the August 2021 print edition ofDental Economics.References
- Vinnakota DN. Effect of preparation convergence on retention of multiple unit restorations – An in vitro study. Contemp Clinc Dent. 2015;6(3):409-413.
- Blair FM, Wassell RW, Steele JG. Crowns and other extra-coronal restorations: Preparations for full-veneer crowns. Br Dent J. 2002;192(10):561-564, 567-571.
- Mendes M, França FMG, Basting RT, Turssi CP, do Amaral FLB. Long-term bond strength of fiber posts cemented to dentin with self-adhesive or conventional resin cements. J Adhes Sci Technol. 2017;31(9):977-987.
- Ferreìra-Filho R, Ely C, Amaral R, et al. Effect of different adhesive systems used for immediate dentin sealing on bond strength of a self-adhesive resin cement to dentin. Oper Dent. 2018;43(4):391-397.
- Borges MHR, Barroso CG, Dias T, Alencar C de M, Silva CM, Esteves, RA. Evaluation of physical-mechanical properties of self-adhesive versus conventional resin cements. Braz J Oral Sci. 2020;19(1):e208204.
- Campos F, Almeida CS, Rippe MP, de Melo RM, Valandro LF, Bottino MA. Resin bonding to a hybrid ceramic: effects of surface treatments and aging. Oper Dent. 2016;41(2):171-178.
- Ady AB, Fairhurst CW. Bond strength of two types of cement to gold casting alloy. J Prosthet Dent. 1973;29(21):217-223. doi:10.1016/0022-3913(73)90116-9
- Norlander J, Weir D, Stoffer W, Ochi S. The taper of clinical preparations for fixed prosthodontics. J Prosthet Dent. 1988;60(2):148-151. doi:10.1016/0022-3913(88)90304-6
- Principles of tooth preparation. In: Shillinburg HT, Hobo S, Whitsett LD, Jacobi R, Brackett SE, eds. Fundamentals of Fixed Prosthodontics. 3rd ed. Quintessence. 1997;335-353.
- Della Bona A, Northeast SE. Shear bond strength of resin bonded ceramic after different try-in procedures. J Dent. 1994;22(2):103-107. doi:10.1016/0300-5712(94)90012-4
- Yun J-Y, Ha S-R, Lee J-B, Kim S-H. Effect of sandblasting and various metal primers on the shear bond strength of resin cement to Y-TZP ceramic. Dent Mater. 2010;26(7):650-658. doi:10.1016/j.dental.2010.03.008
- Burke FJT. Fracture resistance of teeth restored with dentin-bonded crowns: The effect of increased tooth preparations. Quintessence Int. 1996;27(2):115-121.
- Bindl A, Richter B, Mörmann WH. Survival of ceramic computer-aided design/manufacturing crowns bonded to preparations with reduced macroretention geometry. Int J Prosthodont. 2005;18(3):219-224.
- Sorensen JA, Kang SK, Avera SP. Porcelain-composite interface microleakage with various porcelain surface treatments. Dent Mater. 1991;7(2):118-123.
- el-Mowafy O. The use of resin cements in restorative dentistry to overcome retention problems. J Can Dent Assoc. 2001;67(2):97-102.
Miles R. Cone, DMD, MS, CDT, FACP, a graduate of Tufts University School of Dental Medicine, completed a three-year prosthodontic residency program while serving in the US Army. He later earned his designation as a certified dental technician. Dr. Cone is the owner of Nuance Dental Specialists, a private practice dental clinic limited to prosthetic dentistry in Portland, Maine, and a key opinion leader and educator for GC America. An international lecturer, he has been published extensively in peer-reviewed journals.
About the Author

Miles R. Cone, DMD, MS, CDT, FACP
Miles R. Cone, DMD, MS, CDT, FACP, a graduate of Tufts University School of Dental Medicine, completed a three-year prosthodontic residency program while serving in the US Army. He later earned his designation as a certified dental technician. Dr. Cone is the owner of Nuance Dental Specialists, a private practice dental clinic limited to prosthetic dentistry in Portland, Maine, and a key opinion leader and educator for GC America. An international lecturer, he has been published extensively in peer-reviewed journals.