Ask Dr. Christensen
Gordon J. Christensen, DDS, MSD, PhD
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an e-mail to [email protected].
For more on this topic, go to www.dentaleconomics.com and search using the following key words: Class II resin-based composites, inlays, onlays, Dr. Gordon Christensen.
Q Class II resin-based composites are the most requested restoration at this time. Although I feel that amalgam or cast gold restorations are the materials of choice for some patients, I’m having a difficult time convincing patients to use metal restorations or crowns. They complain about the cost of indirect restorations and the esthetic challenges. I am not pleased with the longevity I’m seeing with large composites. When should composite be used and when should amalgam be used, if at all? Importantly, should composite be used in large Class II restorations, and if so, how can I make sufficient revenue when doing large posterior composites?A You have asked one of the most important questions facing most restorative dentists today. Resin-based composite restorations are low revenue restorations at best, even when they are small. The current ADA average fee range for these restorations is about $185 for a two-surface restoration, to $226 for a three-surface restoration. If Class II restorations are small, up to one quarter of the cusp-tip-to-cusp-tip distance, and with a small box form, these restorations can be placed in an amount of time that makes them financially feasible. But if placed in a Class II preparation that is one half of the cusp-tip-to-cusp-tip distance, the time involved for the revenue produced is not acceptable for an ongoing active practice if placed on a routine basis. Many dentists report that large composites require about 45 minutes.Limoli and Associates reported in October 2010 that in the last 12 months in the U.S., the ratio of composite placed compared to amalgam placed was two Class II composites for every one Class II amalgam.
The use of composite is more popular than amalgam; however, I have found in my CE courses that two thirds of general dentists are still using amalgam some of the time, and only one third of dentists have eliminated amalgam from their practices.
Additionally, the longevity of Class II composites is reported to be less than the longevity of amalgam in large Class II locations. In our long-term research in CLINICIANS REPORT, we have found that the longevity of small Class II composites is similar to amalgam; however, the larger the composite, the shorter the expected longevity compared to amalgam.
In other words, we have a challenge with the currently available restorations for large Class II situations, the reported average revenue, and patient demands for whiter teeth. I have some suggestions that will potentially reduce the problem for you.
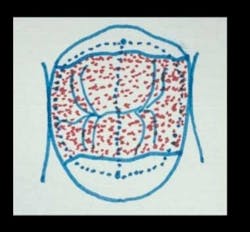
Fig. 1 – Dental carious lesions often do not form on occlusal surfaces, as in the past. The modern-day high use of fluoride has reduced occlusal caries. It has been proven that the grooves of teeth receiving fluoride in their developmental stages fuse more completely than those that have no fluoride. Only a small percentage of dentists placed amalgam in tooth preparations this small. The Class II resin-based composite tooth preparation in this tooth does not have an isthmus cut across the occlusal table.Such minimal preparations are easy to prepare, simple to restore with composite, and easy to finish. Their longevity potential is excellent as shown by long-term clinical research.
Make convincing suggestions to patients for appropriate Class II restorations
The best way to change a person’s behavior on any subject is adequate education. I suggest that patients be educated in depth about the various restorations available for Class II situations, and that dentists strongly encourage them toward the restoration most adequate for their situation. Acknowledging that there are financial constraints, I suggest that with in-depth education, many patients will accept your logical and honest treatment planning suggestions. This is especially true if you can say, "If I were you, I would … fill in whatever treatment you feel is best."
Here are my suggestions for patients with Class II restorative needs:
• Small Class II preparations (Figs. 1 and 2) (Up to one quarter of the cusp-tip-to-cusp-tip isthmus cut or proximal box form only without an isthmus extension.) Resin-based composites have proven to be excellent. When well placed, these restorations provide acceptable longevity and optimum esthetics and tooth conservation.
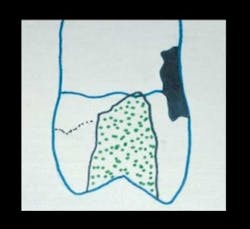
Fig. 2 – This small Class II preparation is about as conservative as most dentists cut a tooth. Today, most dentists place resin-based composite in this preparation. The acceptability of their choice is verified by research to be as satisfactory as amalgam in tooth preparations this small.
• Medium-sized Class II preparations (Fig. 3) (About one third of the cusp-tip-to-cusp-tip isthmus cut or the normal size recognized as "GV Black preps.") Assuming you have a cooperative, well-informed patient, composite can be a viable choice; however, the time involved is often double the small composite. Amalgam is an alternative, but not desirable for most patients. Tooth-colored ceramic inlays (IPS Empress or e.max, either in-office milled or made by a laboratory) are a very good but expensive alternative. Cast gold alloy restorations are the best, if done well; however, they are expensive. Most people will not accept the display of metal unless they are informed about its expected longevity, and you have expertise with cast gold restorations. It has been my experience that when moderate-income patients are informed of all of the alternatives and the expected longevity and esthetic result of each, many choose the more expensive, long-lasting ceramic or gold alloy restorations.
• Large-sized Class II preparations (Fig. 4) (Over half of the cusp-tip-to-cusp-tip isthmus cut.) Patients need to know the liabilities of these large restorations. If these large preparations are restored with composite, they will not serve for long in most situations. Amalgam has a greater longevity in large-sized Class II locations. If they are directly placed intracoronal restorations, cusps often fracture off during service.
Fig. 3 – Deciding what restorative material to put in this moderate-sized tooth preparation frustrates most dentists. Patients want tooth-colored restorations; however, a composite restoration in this tooth preparation requires up to twice the time as the preparations in Figs. 1 and 2, and the average fee does not reflect that extra time.
If indirect extracoronal restorations (onlays) are placed, they are best made of ceramic (in-office milled or laboratory made) or cast gold alloy, which obviously raises the fee about four to five times higher than amalgam or composite.
Fig. 4 – A tooth preparation this large is not a desirable location for either amalgam or composite. The cusps of the tooth often break during normal chewing when the restorative material approaches the cusp tips. Patients should be advised that indirect restorations should be placed in such preparations. However, the cost of indirect restorations is several times more than fees for composite or amalgam. If amalgam or composite must be used for teeth this broken down, covering the cusps, at least the chewing cusp will reduce eventual inevitable breakage. Patients should be warned that direct restorations this large are contraindicated and will serve only for a short and unpredictable period. Indirect restorations should be used.
Unfortunately, only a few dentists are placing onlays. Limoli and Associates reported that only about 1% of posterior tooth restorations placed in the U.S. during the last 12 months were onlays. I would like to see that percentage go up, since well-placed onlays are excellent restorations.
Fig. 5 – Obviously this tooth needs a crown. I strongly suggest telling the patient this is the case. If the patient will not have a crown, advise of the short longevity expected for the large intracoronal restoration. Quite obviously, patching such broken down teeth will eventually result in a failure of the entire restoration.
If large direct intracoronal composite restorations are placed, the average revenue will not support an ongoing practice if done on a continuing basis because of the excess time involved.
Fig. 6 – The conservative resin-based composites placed in these premolars (DO in first premolar and MOD in second premolar) were placed in a few minutes. The effort and time expended will equate to the average fee that is acceptable.
If they are restored with crowns, the longevity is higher than intracoronal restorations, but again the average cost is four to five times higher than direct restorations.
Fig. 7 – The wide and deep preparation in this tooth and its restoration required twice the time as the restorations in Fig. 6. The average national fee for this DO restoration will not equal the time and effort expended to restore it, and it will have limited longevity.
I strongly suggest patients be informed of these liabilities, that the limited longevity expectations of large intracoronal restorations should be noted and recorded for future reference, and that you should tell them with conviction that your choice is the restoration that offers a longer service period.
When such education is accomplished, you and the patient decide, and when a restoration fails, the patient has been informed. I also suggest a higher-than-average fee should be charged for such large intracoronal restorations.
• Teeth with an obvious need for crowns (Fig. 5, see page 52): If more than half of the coronal part of the tooth is missing, there are questionable non-symptomatic horizontal cracks in the tooth, or the tooth has cracked tooth symptoms, a full-crown is usually indicated. Patients should be so advised. If they cannot afford or will not accept a crown, they should know that any attempt to repair or patch the remaining tooth structure will be only a provisional restoration.
Summary of my answer
Find Class II carious lesions and treat them when they are small! Such resin-based composite restorations are simple, easy, long-lasting, and financially feasible (Figs. 6 and 7, see page 44).
I have the same financial frustrations with treatment planning as those presented in your question. Resin-based composite is excellent in small-to-moderate sized Class II restorations. Its value in large restorations is questionable. The time involvement and difficulty of placement make composite financially less feasible and acceptable. But sometimes typical dentists have to use it in these unfortunate situations.
Educate your patients that moderate and larger-sized restorations are usually better treated with metal or ceramic. When a crown is indicated, tell them so, and let them know that patching such teeth will provide only interim service.
Practical Clinical Courses (PCC) has several educational aids to help you with this important "bread and butter" subject:
• Patient education DVDs. Descriptive videos for patients to view. Average length is nine minutes. Several of the 16 titles discuss and compare restorative options offered in most general practices.
• One-hour CE DVD, V3519 "Predictable, Non-Sensitive Resin-Based Composites"
• Two-day hands-on course, "Practical Esthetic Restorative Dentistry"
Visit our Web site at www.pccdental.com or call (800) 223-6569 for more information.
Dr. Christensen is a practicing prosthodontist in Provo, Utah, and a Diplomate for the American Board of Prosthodontics. He is the founder and director of Practical Clinical Courses, an international continuing education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of CLINICIANS REPORT (formerly Clinical Research Associates), which has conducted research in all areas of dentistry since 1976. Dr. Christensen is an adjunct professor for Brigham Young University and the University of Utah.
Past DE Issues