Reducing postoperative sensitivity associated with composite dentistry
Hypersensitivity after the placement of direct resin restorations is an unwelcome outcome for the dental practitioner. It can result in disruptions in a schedule and unhappy patients. Hypersensitivity can cause restoration replacement and the additional loss of tooth structure that happens whenever restorations are removed.1 The prevailing theory concerning the cause of dentin hypersensitivity is based on hydrodynamics and was initially developed by Brännström2,3and further developed by others such as Pashley.4
Procedures that leave dentinal tubules and collagen exposed during restorative treatment increase the risk of dentin hypersensitivity. When these tubules are stimulated with cold, heat, substances that create an osmotic gradient, or mechanical stimuli, the fluid within the dentinal tubules can move and stimulate odontoblasts and nerve fibers found in the tubules near the pulp. Patients can perceive this as pain.
Multiple methods have been used in an attempt to alleviate hypersensitivity symptoms associated with resin restorations, including the use of dentinal desensitizing solutions in conjunction with adhesive placement. It has been claimed that glutaraldehyde-containing solutions have been effective because of glutaraldehyde's ability to denature proteins and thus impact permeability of the dentin.5 Yet, a recent systematic review and meta-analysis showed that postoperative sensitivity remains a potential outcome regardless of whether a self-etch or etch-and-rinse adhesive is used.6
READ MORE | Preventing postoperative tooth sensitivity
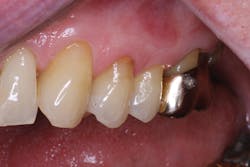
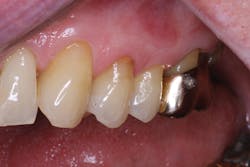
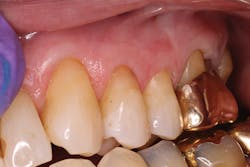
Facial restoration of tooth No. 13 six months after placement.
Facial restoration of tooth No. 13 one year after placement. The tooth demonstrated preoperative sensitivity and showed no sensitivity at recall evaluations.
We recently reported six-month results for a company-supported clinical study at the 2016 Annual Session of the American Association for Dental Research and now have collected one-year follow-up data.7 The study included 81 facial adhesive restorations for noncarious class V lesions (NCCLs) placed with both self-etch and selective-etch techniques. Each restoration was placed using Adhese Universal (Ivoclar Vivadent) with Tetric EvoCeram resin composite (Ivoclar Vivadent) after placement of a rubber dam. An evaluation of hypersensitivity was made prior to placement of the restorations. To do this, a blast of air 1 cm away from the tooth was directed at the NCCL for a period of 1 second. The patient was then asked to rate the sensitivity on a 0- to 10-point scale where 0 was no sensitivity, 1–2 was considered to be mild sensitivity, 3–6 was moderate sensitivity, and 7–10 was severe sensitivity. The initial range of scores was from 0 to 10 where 85% of the teeth showed no or mild hypersensitivity whereas 15% (n=12) of the teeth showed moderate to severe dentinal hypersensitivity. At the time of the six-month evaluation, 100% of the teeth examined showed no or mild hypersensitivity. At that time, no restorations demonstrated moderate or severe hypersensitivity. One year after placement, 97% of the evaluated restorations still reported no more than mild sensitivity. Two restorations were reported to demonstrate moderate sensitivity. The patients who reported a 10 at baseline continued to report a 0 after one year, as they did at six months. It was apparent that the restorations placed with Adhese Universal were effective at eliminating or minimizing postoperative dentinal hypersensitivity.
READ MORE | Suppressing the 'ouch' factor: New desensitizer lasts 3 years
The manufacturer, Ivoclar Vivadent, claims that the successful desensitizing effect of this adhesive occurs because (1) the hydrophilic solvents (water and ethanol) and hydroxyethyl methacrylate (HEMA) optimize wetting, priming, and infiltration of the hydrophilic resin monomers into dry or moist dentinal tubules, and (2) demineralized collagen networks to ensure the formation of a reliable dentinal seal via the formation of a homogenous adhesive layer with defined resin tags. The adhesive contains acidic monomers (10-methacryloyloxy-decyl dihydrogen phosphate, MDP; 7-methylchroman-2-carboxylic acid N-(2-trifluoromethyl) phenylamide, MCAP) that precipitate as insoluble calcium salts in the dentin. The precipitates facilitate mechanical blockage and sealing in the dentinal tubules. Predictably blocking the tubules helps prevent the movement of fluid in the dentin as well as postoperative sensitivity associated with that movement. The formation of a stable, thin, homogenous adhesive layer with a low film thickness is ensured by the optimized thickening agents-fumed silica and methacrylated carboxylic acid polymer.8
References
1. Beck F, Lettner S, Graf A, et al. Survival of direct resin restorations in posterior teeth within a 19-year period (1996-2015): A meta-analysis of prospective studies. Dent Mater. 2015;31(8):958-985.
2. Brännström M. The surface of sensitive dentine. Odontol Revy. 1965;16:293-299.
3. Brännström M. The sensitivity of dentine. Oral Surg, Oral Med, Oral Path. 1966;21:517-526.
4. Pashley DH, Matthews WG, Zhang Y, Johnson M. Fluid shifts across human dentine in vitro in response to hydrodynamic stimuli. Arch Oral Biol. 1996;41(11):1065-1072.
5. Felton DA, Bergenholtz G, Kanoy BE. Evaluation of the desensitizing effect of Gluma dentin bond on teeth prepared for complete coverage restorations. Int J Prosthodont. 1991;4(3):292-298.
6. Reis A, Dourado Loguercio A, Schroeder M, Luque-Martinez I, Masterson D, Cople Maia L. Does the adhesive strategy influence the postoperative sensitivity in adult patients with posterior resin composite restorations? A systematic review and meta-analysis. Dent Mater. 2015;31(9):1052-1067.
7. Rouse MA, Platt JA, Cook NB, et al. Clinical evaluation of a universal adhesive in non-carious cervical lesions. J Dent Res. 2016;95(Spec Iss A):1654.
8. Ivoclar Vivadent. Adhese Universal Scientific Documentation. http://downloads.ivoclarvivadent.com/zoolu-website/media/document/24318/Adhese+Universal?_ga=1.59892589.1729649605.1475700410. Accessed October 5, 2016.
Jeffrey A. Platt, DDS, MS, is a 1984 graduate of the Indiana University (IU) School of Dentistry. After four years of active service in the US Navy Dental Corps, he obtained an MS in dental materials while maintaining a full-time private practice. He accepted the appointment of director of IU's Division of Dental Materials in 2000, is the Ralph W. Phillips Scholar in Dental Materials, and is the chair of the Department of Biomedical and Applied Sciences.