HOW TO PROFIT FROM...digital radiography
How can digital radiography fit into your practice?
V. Kim Kutsch, DDS
Digital radiography was first introduced to the dental profession in 1989. From the beginning, digital radiography has been a technology that has drawn and maintained dentists? interest, but also has maintained a very slow rate of adoption and acceptance. While the interest levels are understandable, the slow movement of the profession to adopt this technology is puzzling. Radiographs remain a primary source of diagnostic data for most dental pathologies.
Therefore, logic dictates that any advancement in this technology would have widespread appeal to the profession. In addition, more than 30 years of fluoridation have resulted in a new model of disease for dental caries, which is becoming increasingly harder to diagnose with conventional radiology.
Improvements in digital radiography offer solutions to current diagnostic dilemmas. Yet, the profession appears slow to embrace this technology.
As with any emerging technology, a small percentage of Oearly adoptersO and thought-leaders quickly accept the technology. They are often responsible for its developing role in clinical practice. This is generally followed by a period of intense competition from manufacturers leading to predictable confusion amongst the consumers. For technologies that have merit and improve patient outcomes, this gradually gives way to a period of slow adoption by the majority of clinicians. As information slowly accumulates, the clinician?s apprehension is replaced with knowledge and understanding. Ultimately, the new technology becomes Ostandard of care.O
At the heart of digital radiography for today?s practicing dentist is a lack of good clinical and sound financial information. Selecting new technology is one thing; integrating it into an existing practice system and having it be financially successful requires a great deal of thought.
Historically, the principle diagnostic tools for identifying dental caries have been visual examination, sharp explorers, and radiographs. As the nature and progression of caries has changed, these tools have become less diagnostic and less effective. There also has been a growing concern in the population regarding unnecessary exposure to X-ray irradiation. From a clinical standpoint, the improvement of radiography technology solves some diagnostic issues. Many authors have examined the growing role of digital radiography in improving diagnosis and patient outcomes, raising the standard of care. The often-dramatic reduction in radiation requirements and providing better diagnostic images have been repeatedly discussed and are generally well-accepted as fact. The real remaining issues with this technology involve long-term digital integration, practice-management platforms and systems, and return on investment.
Several digital-radiography systems currently are available in the dental market. Each has its own unique features and characteristics. A practitioner really needs to examine why he/she is integrating this technology into his/her practice, how he/she plans to use it, what his/her long-range goals are, and how it will integrate with other technologies. Unfortunately, dentists often only look at the cost side of the buying equation. They purchase equipment based on impulse and emotion, rather than investing in new technology based on strategic planning and return on investment.
The current systems can be divided into two primary variations of the technology, which lead to significantly different paths for integration and management. One basic type of the technology (phosphorous plate) employs reusable film packets that mimic film. This version requires the least amount of paradigm shift for the practice and allows for virtually complete replacement of traditional X-rays in the practice. It also requires the most strategic planning, as going totally OfilmlessO or OdigitalO leads to an incredible amount of digital data that must be stored and archived. The dentist will need a practice-management software platform capable of managing all of the images, coupled with enough hardware storage capability and back-up systems. The system needs to allow retrieval of images for future viewing and is dependent at all times on an operable computer platform. Imagine the practice with four hygienists seeing 400 new patients per year, taking an annual total of perhaps 22,000 radiographic images. If the dentist also has an intraoral camera, the accumulated data adds up to a lot of gigabytes.
The dentist also needs to consider long-term integration with other software and hardware items. Ideally, the practice-management platform would have its own image-manipulation software and the ability to store the digital data directly in the patient?s folder, with no written software Obridges.O The film packets tend to be less expensive than direct-wired sensors, but the overall cost of the system is significantly more expensive. Another disadvantage of phosphorous-plate technology is that the film packets need to be Odeveloped,O or scanned in to the system, so there is no time-savings from instant viewing. The wrapping, exposing, unwrapping, and then erasing the sensor packets also is time-consuming. However, there is no requirement for a darkroom or development chemicals. One system even offers the capability of panoramic radiography as well.
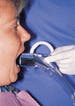
The other iteration of this technology is the direct-wired sensor. Specifically, these sensors are categorized as CCD, CID, or CMOS. CCD was the first system developed, CID is the most robust in a radiation environment (Figure 1), and CMOS features the least-expensive manufacturing process. The primary advantage of the direct sensor is the real-time viewing of instantaneous images. Not waiting for developing results in significant time-savings for the practice, particularly during emergency exams, root canal treatments, or implant location.
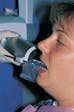
In addition, these systems are much less expensive than the phosphorous-plate technology. Considering long-term strategic planning for integration of this version of digital radiography, the system ideally would provide a universal signal that is compatible with all practice-management platforms. With open architecture, the dentist could begin with this technology and ultimately continue to integrate it into a practice management platform with its own image-manipulation software, allowing image storage directly in the patient?s folder, with no written software bridges. This version provides a slightly larger paradigm shift for practitioners, as the sensors are hard-wired to a monitor or computer and are thicker, less flexible, and less like X-ray film (Figure 2).
The sensor is isolated with a disposable sleeve (Figure 3) and placed in position with the Rinn alignment system or similar holding brackets (Figure 4).
Hard-wired sensors are not really designed to totally replace traditional X-ray film in the practice, but rather to allow the dentist to incorporate digital technology for those instances where it improves clinical results.
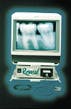
Considering the different digital X-ray technologies, additional considerations need to be examined. Does the practice currently have computers in each operatory? Does the current practice-management software platform have the capability of image manipulation and storage without software bridges? Is there enough hardware storage space? Does the digital-radiography system have open architecture? Will it integrate successfully with future changes in computer equipment (Figure 5)? Does the practice plan to go filmless now, or is it looking for a system that will offer the technology now and then will successfully transform into total integration in the future? Total digital integration is on the horizon for dentistry. Is the system the practice is considering on the pathway, or is it a cul-de-sac, or a dead end? Will the system provide a return on investment that justifies the purchase? As with any new technology, digital radiography is rapidly changing. Dentists planning on purchasing digital radiography should examine not just the features of the product, but the company itself, the after-sale service, and support. Will the company be able to service the product two years from now?
It is not unusual for a dentist to purchase a digital-radiography system and then purchase additional computer hardware, a new software platform, and backup system. If the system is computer-based, a computer will need to be in each operatory. The practice also may find it necessary to have two monitors in the operatory as well ? one for the assistant and one for the doctor and patient to view. The practice may find it more practical to install a computer network with a large file server.
A careful analysis of existing computer technology in the practice is important before purchasing digital radiography. Then the question becomes: Will the practice integrate the technology slowly into the practice or attempt to leap directly to filmless? Gradual integration often is the best route when integrating new technologies, allowing everyone in the practice to comfortably go through the learning curve.
Digital radiography has many recognized advantages: improved diagnostic quality, real-time viewing of magnified images, reduced radiation, the ability to manipulate and store or even transfer electronic digital data, improved communication, enhanced practice image, and proactive marketing. All of these advantages affect profitability and must be considered when calculating return on investment. Improved diagnostic quality of images results in more accurate and complete diagnosis of the patient?s conditions. It also typically results in the diagnoses being made earlier, when conditions can be treated with more conservative and less-invasive procedures ? e.g. microdentistry. More procedures end up being performed, but at an earlier stage of the disease, which benefits the patient. Real-time viewing of magnified images results in time-savings, improved diagnostic quality, and better communication with the patient. Using a direct-wired sensor 8-10 times per day could result in savings of up to one hour of chairtime. Real-time savings result in real increases in revenue directly proportional to the normal productivity of average chairtime. The improved diagnostic quality and magnified images improve communication with the patient.
It is much easier for a patient to identify and understand his/her dental conditions on an image viewed on a 20-inch monitor rather than a 1-inch X-ray film. With better identification and understanding of their oral conditions, patients always exhibit increased acceptance and pursuit of treatment.
The ability to manipulate images further enhances the diagnostic capabilities and communication with the patient. Often, the dentist will find conditions not apparent at first examination by enhancing the image. Typical image manipulation consists of altering brightness or contrast, measuring root canal lengths, sharpening, magnification, colonizing, or highlighting areas of concern. If the image has poor quality or misses a root tip, a new image can be captured in seconds. Additional films for measurement or angulation during root canal therapy improve the quality of care. While the manipulation is certainly a direct advantage, it also is time-consuming. Saving five minutes of developing time to spend 20 minutes manipulating an image results in less profitability. In fact, most dentists who use digital radiography typically spend very little time manipulating the image.
Storing digital data becomes more of an issue as digital radiography is integrated more and more into the practice. At first, many dentists use the technology for diagnostic purposes and communication, and do not intend to store the image in the patient?s electronic folder. Transferring the electronic data also will become more important in the future, as more practitioners and dental insurance companies convert to this technology.
The reduced radiation and enhanced practice image help improve profitability as well. Digital radiography gives the practice the image of being Oleading edge,O and also allows for proactive marketing. The dentists can take a pre-op image as a marketing piece to help patients understand their own conditions and also promote the practice as a whole. High-tech modalities, such as digital radiography, send a clear message to consumers that the practice is definitely Oleading edgeO and improve the practice image. The ability to send images home with the patient helps to market the new technology and the
Figure 1
Figure 2
Figure 3
Figure 4
Figure 5