GROWING Case Acceptance with the right words
Cathy Jameson, Ph.D.
You can say something one way and get a positive result. Put it another way and get a negative result. No matter what your role in the practice may be, your success depends on the way you communicate.
In most practices worldwide, there is more dentistry waiting to be done in the charts than most dentists actually do in their practicing lives, according to decades of data gathered by Jameson Management consultants.
Gallup Polls published by the American Dental Association found the No. 1 reason people don't accept proposed dental treatment is a lack of dental education or no perceived need. So, your greatest commission as dental professionals is to become good educators.
People communicate by reading, writing, speaking, and listening. To be an effective communicator who gains high levels of case acceptance, you must be cognizant of all communication means. Focus all communication efforts to meet the recipient's needs. Keep things positive, constantly affirming your purpose and mission to provide the best dental care possible. Focus on the end result and benefits, remembering that people always filter what they hear or read through the question, "What's in this for me?"
Written communication must be clean, clear, and reflect the practice's image. Concentrate on consistency and short, straightforward statements that are true to your marketing or branding goals.
When communicating face-to-face, be aware of your image and body language. Be well dressed and well groomed. Lean slightly toward the person to whom you are presenting to show him or her how alert and interested you are. Think about your tone of voice. Are you monotonous, or is your voice interesting, dynamic, and convincing?
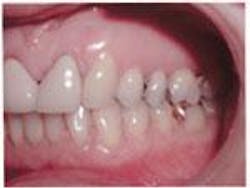
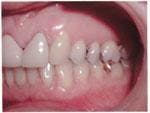
Since 83 percent of learning is visual, 11 percent by hearing, and the rest by other senses, visual aids are vital for effective communication. By visual aids, I mean before-and-after photos and other patient-education resources. Remember, people follow your focus, so when you want them to look at a visual aid such as a computer monitor, look that way too. Look at the patient only to assess his or her interest level, and make eye contact. Involve as many of the senses as possible, emphasizing sight above all else.
As for case presentation, the most important aspect of effective communication is focusing on patient needs and wants through listening, reading their forms and paperwork, writing their treatment plans, and presenting the case.
When it comes to verbal communication, remember the Boy Scouts motto, "Be prepared." Treatment planning is one thing, but presentation planning also is critical. Follow these three guidelines:
• Introduce — Tell patients what you are going to tell them.
• Present — Tell them what you are there to tell them.
• Summarize — Tell them what you told them.
The key to learning is repetition. Speak in layman's terms and repeat yourself to help patients feel comfortable with what they hear. Questions help you understand patients' goals and how you can meet and exceed expectations. When asking questions, keep patients involved while affirming your interest in their well-being. Questions may uncover objections or areas of insecurity or concern. Face objections head-on so patients trust you and understand your intentions. Take objections as signs of interest. If a person objects, he or she is interested and thinking about your proposal. When preparing, identify a few common objections and determine effective responses.
I recently spoke with two doctors whose practice is doing well. They're focusing on going from a good practice to a great one and beyond. They know some goals are being met and their team is skilled, but there's always room for improvement.
The doctors told me about a potential patient who asked their business administrator if appointments usually run on time. The administrator quickly answered, "We usually run about five to 10 minutes behind." The doctors asked how I would coach this team member for a more effective response.
It's common to answer a question before understanding what is being asked. Sometimes people answer questions without knowing the core issues behind the questions. In this example, the business administrator needed to find the patient's key motivator in order to address her concern with their commitment to respecting a patient's time.
Challenge yourself to think about patients' needs and motivators not only as you present a formal case, but in all your communications, even as you listen. Listen carefully to everything they say as you think about what motivators may be underlying questions and messages. This idea seems obvious but most often is overlooked. Asking appropriate questions will convey that you're listening and caring, but don't answer questions with questions to the point of frustrating a potential patient. Let patients know you're hearing them and you're trying to answer them with the most accurate, thorough, insightful, and caring responses possible.
I suggest a response similar to this: "It sounds like being on time is important to you." Then, allow the person to explain his or her reasons for such a concern. Understanding the situation better and thinking you can accommodate that need, say, "We'll do everything we can to make that happen for you."
Many dental professionals are afraid to ask, "How do we close the sale?" or "How do we get even better?" Professionals hesitate talking about "closing" or asking patients for commitments because they don't want to seem pushy or high-pressure. Using effective verbal skills to schedule an appointment for someone who needs dental work to meet their goals will not be perceived as pushiness. You're a dental professional, and part of your job is to educate patients about dentistry, and then eliminate barriers until that dentistry is completed.
Here's how it works. First, ask questions. Then, listen for the motivators. Opening questions such as "How can I help you?" "What are your goals for your teeth, your mouth, and your smile?" "What do you like most about your teeth?" "What do you like least about your teeth?" "If there were anything you could change about your smile, what would it be?" are effective in identifying motivators and helping patients think through their goals.
For example, the doctor asks, "If there were anything that you could change about your smile, what would that be?" The patient responds, "I really don't like the stains on my teeth. They're so embarrassing and I just hide my teeth as much as I can — even when I laugh or smile." After listening carefully and being conscientious of his or her body language, the doctor says something such as, "So you are uncomfortable with the discoloration of your teeth, and you are interested in getting a whiter, brighter smile. Is that right?" The doctor needs to make sure all the patient's concerns or goals (which usually fall within appearance, comfort, function, keeping teeth for a lifetime, time, or money) have been heard.
Once the patient confirms your understanding, the trust between the two of you grows and, if you've heard all of his or her concerns, you know the motivators around which to build your treatment plan.
Then, present the case by covering the following key areas.
• What's going on now? Tell the patient exactly what the current situation is in comparison to the goals he or she communicated to you in step one.
• What are your expert recommendations? Tell the patient what your proposed treatment plan is, whether that is restoring a mouth to health or changing a smile to be more beautiful. Tell the patient exactly what to expect.
• What are the benefits? Explain how the proposed treatment will satisfy the patient's initial intention.
• What are the disadvantages if the patient chooses not to proceed? When appropriate, bring any long-term considerations to the patient's attention to help him or her understand both sides of the decision.
• Then, close! Use closing statements to identify barriers and objections. These questions call for a commitment. They give you a chance to address any areas of concern or alleviate reservations so the patient can commit to making his or her dream smile a reality.
Here's an example using the aforementioned system. Note the constant focus on the patient's needs and goals.
• Last week you indicated ______ is important to you. I've been able to design a plan of treatment around those valid needs and wants. Your current situation, as you see on these photographs taken during your last visit, is ________. As you see in these other "before" photos, this patient had a similar situation to the one you're in now.
• Just look at the amazing difference in these photos after a procedure called _______. I'm confident these results are realistic for your initial goal, and this could be accomplished by (number of appointments, any key factors in the decision based on the patient's initial goals).
• The benefits include (a more beautiful smile you've described as ideal with no gaps or yellowing, crooked teeth, a healthy, disease-free mouth that can be easily maintained for a lifetime, any specifics regarding their situations).
• So, is there any reason not to schedule your appointment today? (If the patient indicates a barrier, you'll have a chance to address that thoroughly.) Is this the treatment that will work for you? Do you have enough information to make a decision, or do I need to clarify something further?
All of the aforementioned advice follows the "Six Steps of Case Presentation:"
Step one: Build the relationship. Before a person will say "yes" to your recommendations, you must first build a relationship of confidence and trust.
Step two: Establish the need. Ask the opening questions so you may deeply and accurately understand the patient's attitude toward dental health or toward the appearance of his or her smile so you have an accurate grasp of the patient's perceived need.
Step three: Instill the desire. Educate the patient about what is and what can be so he or she understands the potential positive end results.
Step four: Ask for commitment. It is appropriate to ask for a commitment from the patient. For example, ask, "Have I explained the treatment so that you are comfortable with my explanation?" If the patient responds with something such as, "Yes, I'm clear on what needs to be done," then ask, "Then do you have any further questions?" If the patient does not, say, "Then is there any reason why we shouldn't go ahead and schedule an appointment to begin your treatment?" Once your patient is ready to schedule the appointment, you're ready to move on.
Steps five and six: Financial arrangements and appointment scheduling. There is no exception to this order. Financial arrangements always precede appointments. We recommend the treatment coordinator join the doctor while presenting the case. That way, the treatment coordinator can support the doctor and answer questions the patient may have.
In addition, the treatment coordinator can confidently present financial options to the patient. The doctor may say, "OK, then I am going to have Jan, my treatment coordinator, discuss the financial responsibilities. She will schedule your first appointment. I look forward to working with you." The trust has been reaffirmed and validated, and you're on your way to a strong doctor-patient relationship. There's another case that didn't land in your charts! No matter how your office is organized, careful team planning before the consultation will result in greater case acceptance.
In summary, consider these when using verbal skills to increase case acceptance:
• Identify the patient's needs and goals. Then focus on those throughout all treatment planning and communication.
• Get to the point using patient language and visual aids for maximum comprehension.
• Stress the benefits of proceeding and, as appropriate, the disadvantages of not proceeding.
• Be clear, direct, and confident in your expert recommendations, and confirm patient commitment.
Get the dentistry out of the charts and into the mouths of your patients. Remember — communication is the way to success.