An eye-opening experience that patients love!
What is the best way to conduct a new-patient exam and present the appropriate treatment plan effectively? The recommendations of experts, especially from those who are not dentists or who are not practicing clinical dentistry full-time, often promote a variety of complex processes. At one extreme is the high-end, comprehensive examination that involves several lengthy appointments with the doctor and the dental team. This approach requires considerable time spent espousing office philosophy to ensure a good fit between the patient and the office. At the other extreme is a basic system in which the initial exam is completed by the hygienist followed by a quick exam by the doctor. There is no universal agreement between dental practitioners on this subject since no single method is appropriate for every dentist or patient.
The old adages of “a picture is worth a thousand words,” “seeing is believing,” and “to see is to understand” are certainly true when it comes to communication in dentistry in the 21st century. It is necessary to take the voodoo or mystery out of dentistry for the patient - to remove the obscurity and let a patient see what the dentist sees. This allows a patient to understand much more quickly, and helps to build trust and understanding. This results in a better relationship between a patient and the doctor. Traditionally, a dentist has looked and poked in a patient’s mouth, then viewed small radiographs on a light box. Upon announcing his or her findings, the dentist has expected patients to understand and agree to proposed treatment immediately. Today, there is a much better way. By effectively using modern technology, a patient now can see what is in his or her mouth, understand what the dentist is talking about, and even ask intelligent questions about what has caused a problem as well as possible solutions.
The advantages of using digital technology in new-patient exams are numerous and priceless. Often, they are viewed as necessary for the maintenance of a practice. However, new-patient exams are time-consuming procedures for a dentist, and often are considered the least productive time of the day. Thus, they are delegated to the hygiene department. Giving a patient the ability to see exactly what the dentist sees is a key to effective communication and treatment acceptance. The digital new-patient exam not only reduces the time necessary for the dentist to conduct a comprehensive exam, it also leads to increased treatment acceptance. This increases the profitability of a practice, and reduces stress in the office.
The digital new-patient exam involves most of the steps that traditionally have been done. Dental and health histories are reviewed, hard-tissue and soft-tissue exams with oral cancer screenings and occlusal analysis are completed, and necessary radiographs are obtained as well as study models and photographs when indicated. But with the digital new-patient exam, most of these steps are completed more effectively since they are recorded digitally and entered only once in a patient’s record.
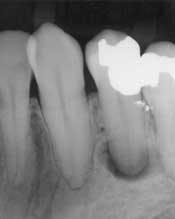
At first glance, the most obvious difference between the traditional patient exam and the digital new-patient exam is in the size of the radiographs. It is now possible to take a bitewing, a periapical film, or a panorex and show it on a large computer monitor that is visible to both the dentist and the patient (Fig. 1). With a laser pointer, it is possible to demonstrate normal or pathologic bone level, periapical pathology, tartar on teeth, the pulp chambers, and dental caries. Frequently, after just a few explanations, patients are able to detect other cavities, calculus, or areas of bone loss. When this happens, the level of ownership and responsibility taken by the patient increases significantly.
A second area that leads to effective patient communication is the consistent use of a good digital intraoral camera. Intraoral cameras are not new. But a digital camera enables uncomplicated viewing on a computer screen, saving a photo in a patient’s file without having to print it. In addition, the dentist can retrieve the photo so that it can be reviewed during a future treatment consultation, or the photo can be used for the electronic submission of an insurance claim.
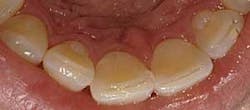
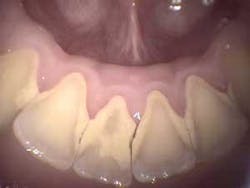
What should be photographed and reviewed with a patient? Items that should be documented in the digital patient record fall in this category. These include areas of visible pathology such as bruxism (Fig. 2), abfractions, attrition, caries, broken teeth, failed restorations, failed sealants, fracture lines, periodontal conditions including plaque, calculus (Fig. 3), root exposure, irregular or infected gum tissue, and soft-tissue lesions. It also is beneficial to take photos of normal teeth and tissue to show a patient the difference. A full-face portrait and full-smile photo also should be taken with a digital extraoral camera and imported into a patient’s file. These are helpful when discussing esthetic concerns, to have a baseline to compare to in the future, or for reconstruction in the unfortunate event that a patient loses part of his or her smile in an accident.
A third important difference is the incorporation of digital patient-education modules such as the CAESY server system. This allows for simple, short, yet complete video clips - organized in visible, understandable modules - about dental conditions ranging from understanding periodontal disease or occlusal problems to implants and equilibrations. When a patient views the appropriate segment(s) with the dentist or designated team member, it opens any concerns to relevant questions and immediate dialog.
Many other technologies such as the DIAGNOdent, electronic bite registration, or electronic probes also can be incorporated into the exam, when necessary. But, for simplicity, I will discuss only three technologies.
How does one use the digital radiographs, the digital photos, and the digital patient-education system effectively in the new-patient exam? The best way to illustrate this is with an example of a relatively simple, but frequent, scenario in which the exam can be used. A female patient in her mid-40s, with limited financial resources, has been seeing a dentist twice a year for as long as she can remember. The bitewing radiographs forwarded from a former dentist are unreadable copies that are more than one-year-old; no FMS or panorex are available. She presents with no chief complaints other than she has noticed that through the years her front teeth appear to be getting flatter and shorter. Besides this, the visit was for a routine teeth cleaning. The former dentist told her that flatter and shorter teeth were merely a part of growing older. In observing her smile, while reviewing her medical and dental history, it was obvious the patient was a chronic bruxer. When asked if she had been told that she might have gum disease, or whether she had ever ground her teeth, the patient responded that she had not. However, she did note that the dentist had performed a “deep cleaning,” and she had been encouraged to floss more regularly and visit the office more frequently for cleanings. Upon examination, it was observed that the patient had occlusal wear into the dentin on all upper and lower anterior teeth as well as many wear facets on posterior teeth. In addition, she had deep abfractions on upper bicuspids and two molars (No. 30 and No. 3), and had failed, large amalgams with recurrent decay and large fracture lines. She indicated that these two teeth occasionally were sensitive to chewing, especially with chips and pickles. Two- to three-millimeter recession was noted around several of the patient’s posterior teeth. Spot periodontal probing revealed pocket depths of four to six millimeters in both the upper and lower molar areas. The radiographs revealed calculus spurs on the molars, and lower anteriors with generalized two to three millimeters of bone loss evident. A large radiolucency also was visible around the root of No. 20.
The diagnosis was really quite basic: bruxism, perio ADA Class 2, deep abfractions on the upper bicuspids, devital No. 20, and fractured tooth/caries on Nos. 3 and 30. The phase one treatment plan to restore her to basic health: four quadrants of scaling and root planing combined with oral hygiene instruction, RCT No. 20, followed by a post and core, then full-coverage crowns on Nos. 20, 3, and 30. The deep abfractions on the upper bicuspids also should be restored. A bite splint, and possibly an equilibration, should also be done minimally. In addition, a conversation should take place about the possible future restoration of the anterior teeth if the wear continues, or if the patient wants to improve the esthetics of her smile.
How do you convey this to the patient in a quick, yet effective manner? The digital way is the quickest and most effective. It could take hours to explain the conditions and treatment as well as build the relationship and rapport for a patient to accept the recommended treatment. Even so, patients usually do not realize there is a problem that needs to be addressed. It is easy to forget that patients have no dental background. If they do not understand a problem, they cannot understand the need for the presented treatment. The result is that a dentist is often looked at suspiciously, and patients wonder if the dentist can be trusted or if they are being cheated.
The most effective scenario is for a presentation to be divided into several categories by discipline: periodontal conditions, bruxism-occlusion, endodontics, basic restorative, and crown and bridge. A dentist or staff member might begin by watching a short video clip on periodontal disease with the patient. Following this, the patient can view intraoral photos showing the recession, tartar, and infection of his or her teeth and gums plus radiographs showing bone loss and tartar spurs. After seeing these problems in his or her mouth, the patient might be mortified initially. But soon the patient understands the situation, and is willing to discuss treatment. Once a patient understands the problem, he or she becomes concerned, and wants to know if the condition can be treated. The scaling and root planing now make sense, and the patient wants the treatment performed as quickly as possible.
Next, tackle the bruxism and abfractions issue. Showing the patient photos of his or her worn teeth and abfractions usually communicates the message. If you observe that the patient still is confused, show another video presentation on bruxism and abfraction formation. At this point, the patient usually gets a grasp of the issue, and then it is much easier to discuss treatment options. When patients see, they understand. When they understand, they want treatment.
Similarly, address the issues of the devital tooth and large failed amalgams. Again, if the issues are divided into understandable bites - aided with visuals from his or her mouth and appropriate educational presentations - a patient begins to understand. At this point, patients begin to view situations as dentists see them. They ask questions. They understand. Treatment acceptance then increases significantly. How long does this take? Not nearly as long as just using words does. How effective is it? Much more than using just words. In most cases, other than the very complex, once an examination is completed, the case presentation also is completed and usually accepted. All that remains is a visit with the financial coordinator. Treatment is scheduled, and payment is arranged.
A word of caution. Do not overwhelm a patient with too much information. Once a patient sees X-rays or photos of any condition, he or she most likely will understand the situation. Once this happens, move on to the next area of concern. Be very observant of a patient’s body language during this process. A patient’s body language will tell you more than he or she ever will tell you in words. The patient might become discouraged. So, it is essential to give the patient positive encouragement, pointing out any good aspects about his or her oral condition. Do not rely strictly on technology to do the selling; verbal skills and relationship-building skills also must be used. Be positive and give the patient a reason for optimism.
In summary, digital technology presently available enables a dentist to complete comprehensive dental examinations and treatment presentations in a quicker and more effective way than traditionally has been the case. In this new paradigm, a patient can see conditions in his or her mouth. The ultimate outcome is that these examinations are comprehensive, the problems are understood by patients, and treatment plans are accepted by patients. In turn, the patient receives better dental care while the dentist experiences increased profitability and less stress.
Since 1978, Dr. Bradley Dykstra has practiced clinical dentistry full-time in Hudsonville, Mich. His interest in practice management led him to earn his MBA degree. In the process, he learned to apply general business principles to dentistry in a practical and profitable way. Besides work at his practice, he does limited speaking and consulting work through his company - Anchor Dental Consulting - on practice management, integrating technology into the dental office, and integrating the dental laser into everyday practice. He can be contacted by phone at (616) 669-6000, or by e-mail at [email protected].