Ask Dr. Christensen
In this monthly feature, Dr. Gordon Christensen addresses the most frequently asked questions from Dental Economics® readers. If you would like to submit a question to Dr. Christensen, please send an e-mail to [email protected].
For more on this topic, go to www.dentaleconomics.com and search using the following key words: preradiation therapy, patient education, dental caries, restorations, fluoride trays, tooth condemnation, casts, Dr. Gordon Christensen.
Q I had a very unfortunate experience in my practice recently. A patient I had not seen for many months came in for a recall appointment. Since I last saw him, he had been diagnosed with several squamous cell carcinomas on his face and neck. He had undergone 60 radiation treatments for the cancers in addition to some disfiguring surgeries on his face and scalp. The cancer clinic responsible for his radiation treatments had not placed him on any dental preventive treatments during his radiation therapy or told him of the dental risks produced by the radiation therapy. What should have been done before starting the radiation therapy to prevent the gross dental caries I observed, and what can I do for him now that he has extensive dental caries all over his mouth?
A I am sorry to hear of the severe dental caries problem present in your patient. The cancer center that provided the radiation therapy for your patient apparently was not informed about the necessity for preventive oral care during and subsequent to the radiation therapy. I will describe the current preventive oral therapies that should be prescribed for those persons receiving intense radiation therapy for cancer, and I will suggest some remedial restorative therapy for your patient.
• Preradiation therapy communication to the dentist from the oncology practice. The oncologist or a staff person from that office should contact the patient's dentist in advance of the beginning of radiation therapy. The dentist should be informed of the nature of the therapy that is being planned, the exact location of the radiation therapy in the patient's body, the dosage of the treatments, and the expected number of treatments. The saliva of patients receiving radiation therapy soon becomes minimal in volume, sticky, and thick — an ideal media for initiation and advancement of dental caries. After receiving notification of the patient's radiation therapy treatment, the dental office should treat this patient as an emergency appointment and schedule the following therapy immediately and prior to the patient beginning radiation therapy treatment.
• Oral hygiene during and after radiation therapy. The patient should be warned that highly conscientious oral hygiene must be practiced during the radiation therapy and for an indefinite period afterwards.
• Preradiation patient education and oral examination. When the preradiation therapy patient is referred to the dentist, an appointment should be scheduled immediately for a thorough oral examination, scaling and root planing, radiographs, and education about the risks of radiation therapy that may affect the jaw.
• Tooth condemnation. Any teeth that appear to be questionable relative to their long-term service potential should be removed. When teeth are removed before radiation therapy, healing is usually uneventful. When teeth are removed after radiation therapy, the chance of osteoradionecrosis is high and hyperbaric oxygen usually must be delivered to promote healing. These treatments can cost more than $1,000 per session, and usually multiple treatments are required. In the event of osteoradionecrosis, bone is left exposed and healing is delayed or does not occur, unless the oxygen treatments are accomplished.
• Areas of radiation that may affect the jaw. The areas where radiation is likely to include the jawbone are: the cranium (head and/or brain), nasopharyngeal, oropharyngeal, supracravicular, neck or spine, and the underarm and chest areas (www.survivorshipguidelines.org).
• Restoration of carious teeth. When the condemned teeth have been extracted, restorations should be placed in any remaining carious teeth. I suggest cariostatic materials such as Ketac™ Nano (3M ESPE), Fuji II LC, or Fuji IX (GC America) for the deeper and more caries-prone areas. When the patient goes for radiation therapy, any suspect teeth should already have been extracted or restored, and the mouth should be infection- and caries-free. After successful eradication of the cancer, the teeth can be restored with any material selected to satisfy the functional and esthetic desires of the patient and the dentist.
• Fluoride trays. Trays for fluoride therapy should be made for the radiation patient, and instruction on how to use the trays should be provided before radiation therapy is started. These trays can be made easily by a qualified dental assistant or dental hygienist as described below. The appointment usually requires about one-half hour:
- Make alginate impressions of the maxillary and mandibular teeth.
- Pour the impressions in fast-setting dental stone. An example of such a product is Snap-Stone (Whipmix) that sets within five minutes.
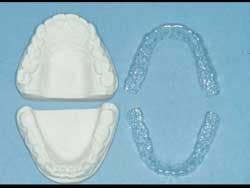
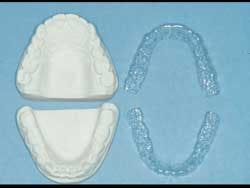
- Fabricate vacuum-formed clear plastic trays about 0.020“ thick.
- Trim the trays to extend about 1 mm apical to the free gingival line. This allows the seated trays containing fluoride gel to be relatively sealed around the soft tissue, thus retaining the fluoride in place during the therapy (see Fig. 1).
- Show the patient how to use the trays.
- Brush and floss the teeth before use of the trays, thus removing the major portion of the accumulated biofilm and food debris.
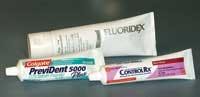
- Place about six drops of 5,000 ppm fluoride gel in the trays, spaced equally around the inside of the trays. Well-known products are PreviDent 5000 Plus (Colgate), Fluoridex (Discus Dental), and ControlRx™ (3M OMNI) (see Fig. 2).
- On placing the trays in the mouth, the fluoride gel is forced into a thin film thickness around each of the teeth.
- The excess fluoride should be expectorated.
- Leave the trays in the mouth for five minutes.
- On removal of the trays, the actions that follow differ depending on whether or not the patient lives in a fluoridated area: a. If the radiation patient is living in a fluoridated area where the drinking water contains 1 ppm fluoride and the patient drinks tap water, the patient should rinse vigorously with water and expectorate the fluoride residue when the trays are removed. This eliminates the chance that the patient may be receiving more fluoride than advisable.b. If the patient does not drink fluoridated water or receive any other significant source of fluoride, the excess fluoride gel should be expectorated and the residue of the fluoride left in the mouth when the trays are removed.
- Fluoride application in trays should be accomplished at least once per day, just before going to bed in the evening. If the patient appears to be a high-risk patient for future dental caries, the tray application can be increased to two applications, one after breakfast and one just before going to bed.
Fluoride administered in trays is an invaluable service to patients who are facing severe systemic health challenges during and after their radiation treatment. What is this appointment worth in revenue for the dental office? Please consult the benefit codes that cover preventive services, and you will find fluoride application in trays to be Code D5986.
Evaluate how much time is required for your staff to accomplish the appointment, and you can easily determine the financial value of the appointment and the necessary income needed to make the appointment financially acceptable. This fee is usually readily accepted by radiation patients, since the alternative is potentially rampant dental caries after the radiation therapy, removal of carious teeth, hyperbaric oxygen therapy, potential osteoradionecrosis, and the discomfort and cost accompanying these conditions.
I have treated many patients on a preradiation therapy basis over several decades. I have yet to treat a patient with fluoride in trays as described who had to have postradiation therapy tooth extraction, hyperbaric oxygen, or who formed osteoradionecrosis. It is a very successful therapy for these unfortunate patients.
I suggest informing the oncologists in your area about the risk of osteoradionecrosis of the jaw, since many oncologists still provide radiation without warning patients of the postradiation challenges.
You also should be making radiographs to determine the presence of dental caries in radiation patients. Practical Clinical Courses recently made a video on “Maxillofacial Radiography — Simplified“ (Video No. 1135). This video shows how to make adequate radiographs in spite of the large rigid digital sensors that are currently available. Included is information about extraoral bitewings and panoramic radiographs, which are especially related to this article.
Of immediate importance to many dental practices is a special PCC video on how to survive in the recession, based on my experiences helping initiate practices. Ask for Video No. 4738, “Creative Management for Increasing Practice Activity.“ For more information, contact PCC at (800) 223-6569 or visit www.pccdental.com.
Dr. Christensen is a practicing prosthodontist in Provo, Utah, and Dean of the Scottsdale Center for Dentistry. He is the founder and director of Practical Clinical Courses, an international continuing-education organization initiated in 1981 for dental professionals. Dr. Christensen is a cofounder (with his wife, Rella) and senior consultant of CLINICIANS REPORT (formerly Clinical Research Associates), which since 1976 has conducted research in all areas of dentistry.