By Dan Bruce, DDS; diplomate, abdsm
Airway trauma, brain damage, or death. Six months ago I found myself sitting in a presurgical room reading over these risk factors on the informed consent. My son was lying in his bed innocently watching cartoons. My wife and I decided to have an adenoidectomy performed to help facilitate his nasal breathing. At five years old, my son had a vague idea about what was going to happen next. Fortunately, he trusts mom and dad completely and knows it will help him breathe better. As a health-care provider, it is easier to tell the parents the minute risks associated with anesthesia and surgery. As a parent, that decision becomes a whole lot more difficult.
Signs and symptoms
My son's symptoms included mouth breathing, halitosis in the morning, excessive movements while sleeping, and occasional mild snoring. He is a very smart and insightful boy, but at times he had trouble concentrating on tasks. (After coaching his soccer team, I found this is a very common occurrence with all 5-year-old boys.) Another pertinent dental finding was a tight lingual frenum that restricted the movement of his tongue. I thought that a child needed his or her frenum released if there was trouble nursing, but this was never a problem with him, so I did not address it. My son did have some difficulty saying certain letter sounds that required the tongue to come up against the front teeth; for example, "L," "6," and "R."
Screening for pediatric sleep apnea
Kids can show different signs and symptoms of sleep-related breathing disorders compared to adults. For example, the Apnea-Hypopnea Index (AHI) threshold for adults to be diagnosed with sleep apnea is five events per hour. For kids, as few as one event per hour is generally a concern and may warrant treatment. In addition, kids can show drastically different signs of sleep disturbances compared to adults. There are several good screening tools for pediatric sleep disorders. For example, the BEARS questionnaire is a simple, effective screening tool for many sleep disorders in a primary care medical setting.1
BEARS stands for:
B = Bedtime Issues
E = Excessive Daytime Sleepiness
A = Night Awakenings
R = Regularity and Duration of Sleep
S = Snoring
Two things to note: Excessively sleepy children can present as either lethargic or hyperactive. A number of studies have linked ADHD symptoms to sleep-related breathing disorders.2,3 Also, any snoring or difficulty breathing in a young child is a red flag and would warrant referral.
In addition to screening questions, oral signs of a sleep disorder may include obstructive tonsils, mouth breathing, venous pooling under the eyes, and a high, narrow palate. If a pediatric sleep disorder is suspected, then referral to a sleep specialist is indicated.
Treatment of pediatric sleep apnea most often consists of removal of the adenoids and/or tonsils. Sometimes rapid palatal expansion is also used. If this is the case, myofunctional therapy may be helpful in maintaining the space gained through expansion (see below).
Effects of mouth breathing and incorrect tongue posture
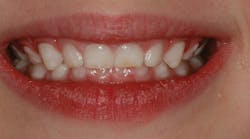
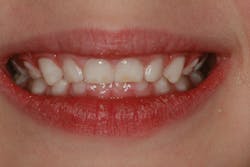
Even if a child does not have sleep apnea, sleep and breathing habits can have a profound impact on the growth and development of the face and airway. We know that the position and strength of the oral musculature can have dramatic effects on the growth and development of the arches and facial structure. When a person breathes through the mouth, the tongue cannot sit up on the roof of the mouth and expand the arches laterally and anteriorly. The results can be seen in the photo below of a 4-year-old patient who is a chronic mouth breather. The primary teeth should have spacing between them. In this case, the teeth have collapsed inward due to perioral muscle pressure and a lack of outward tongue pressure. The tongue is not exerting outward pressure because it is between the occlusal surfaces of the teeth to facilitate mouth breathing. Also note the dry, cracked lips and swollen gingival margins that result from mouth breathing.
Studies by Harvold on primates more than 30 years ago showed that different types of malocclusions were generated from induced chronic nasal obstruction.4 Different tongue postures can also create different types of malocclusions. This is important to assess even in cases of what looks like "genetic malocclusion." Even if a certain phenotype is passed down from parent to child, the cause of this phenotype may be from a shared behavior such as mouth breathing or a shared gene expression resulting from a certain stimulus.
Treatment
For patients who have a habitual mouth-breathing habit, the first step is to determine how significantly the nose is obstructed and why. For my son, the pediatric sleep specialist did not think a sleep study was warranted before assessing the patency of the nasal airway. Therefore, we visited an ENT who performed a nasoendoscopy. This procedure involved spraying an anesthetic in the nose and using a fiber-optic camera to view the nasal passages, airway, tonsils, and adenoid tissue. The ENT felt the first line of treatment was to try nasal saline rinses and a nasal steroid spray. We tried this diligently for about six weeks in addition to elimination of common food allergens in his diet. Unfortunately, my son would get nosebleeds from nasal steroids and rinses, and dietary modifications did not help.
Our next recommendation was to remove the adenoid tissue obstructing the airway. It was not a decision to take lightly for many reasons, but we felt an adenoidectomy would help immensely in the short and long term. There can be a variety of reasons for nasal obstruction, one common one being a deviated septum, so it is important to ensure that a physical obstruction is not blocking the nose. Other alternative therapies to help open the nasal airway and/or shrink the tonsils, which may or may not help, are: treatment for food or environmental allergens, cranial osteothapy to aid in the flow of lymphatic fluid, or nasal strips such as Breathe Right strips. For some patients/parents, these options may be worth exploring before surgery is considered. If the nasal passage is partially open, constant nasal breathing can facilitate further opening.
Next steps
Ultimately we decided to have his adenoid tissue removed. After my son recovered from his surgery, we noticed a significant decrease in nighttime movements and much more peaceful sleep. He was able to sleep most of the night with his mouth closed. He is showing improvement in school. Plus, I felt better because I knew he was getting more oxygen to his brain during sleep.
That was not the end of his treatment, though. My son still had a tight lingual frenum, which limited his ability to place his tongue on the roof of his mouth during rest. This resulted in underdeveloped arches and less room for the tongue. He also still had some trouble saying certain letter sounds, such as "L," "6," and "R."
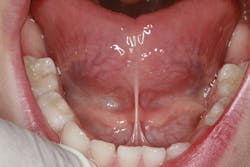
Example of a tight lingual frenum restricting movement of the tongue:
The treatment for these symptoms included myofunctional therapy and a lingual frenulectomy. A myofunctional therapist is typically a speech pathologist or hygienist who has undergone additional training to help correct issues related to mouth breathing, tongue posture, and tongue habits. A listing of myofunctional therapists can be found at www.myoacademy.net, which is the website for the Academy of Orofacial Myofunctional Therapy. There seem to be a lack of trained myofunctional therapists - we need more!
We started my son on some myofunctional exercises to help strengthen and stretch his tongue prior to the frenulectomy. We then used a laser to release the frenum. Oftentimes this needs to extend deep into the fibrous tissue in order to get the necessary functional benefit. Due to the highly vascular nature of the tongue, this is a procedure to be careful with. Directly after the release of his frenum, we did some stretching exercises to help ensure the frenum did not reattach. Again, the degree of tongue-tie can vary. A posteriorly tight frenum can present problems and requires a more technique-sensitive frenulectomy.
The main goals of treatment are threefold: lips together when not speaking or eating, tongue on the roof of the mouth, and breathing through the nose. When in doubt as to whether or not a frenum needs to be released, talk to the myofunctional therapist. These goals (in addition to developing a correct swallowing pattern) are accomplished through training exercises of the tongue, lip, and other oral muscles.
At this time, we are in the myofunctional therapy stage. Training is difficult and time-consuming, but we are making progress. It takes a strong commitment from the whole family to support my son to do his therapy.
What to do now
At a minimum, I think every dentist should be able to spot pediatric sleep-related breathing disorder symptoms, mouth breathing, and a tight lingual frenum. As mentioned above, children should not snore habitually! Snoring alone has been linked to poor academic performance and an increase in ADHD symptoms,5 among other problems. Early detection and treatment can make a huge change for these kids and save significant amounts of medical and dental treatment in the future. Also, the earlier mouth breathing or poor tongue posture is assessed and corrected, the more likely the patient will have better arch development.
The financial impact
There are many questions this article is not meant to answer. For example, what is the etiology of adenotonsillar hypertrophy? If a tight lingual frenum creates so many problems, why does it occur? I encourage you to find the answers to these questions and more. The answers will help dentistry integrate more with medicine and will improve the lives of our patients.
I am very proud of the quality and longevity of my restorative dentistry, but in the current business environment, patients want more. When you screen for obstructive sleep apnea and sleep disturbances in your practice, you can differentiate yourself. My only warning is that some patients do not think they have a problem and do not want to hear a solution to something they do not perceive as a problem. Know your patients, know the science, and make education the primary goal. There is an exciting new concept in the dental field called "airway centric dentistry." Children and adults will sacrifice teeth, gums, and joints to be able to breathe. Keeping this concept in mind will greatly improve the diagnostic and treatment skills of the dental clinician in all areas of dentistry.
Acknowledgement:I would like to thank Dr. Steve Carstensen and Dr. Barry Raphael for enlightening me on some of the concepts presented in this article. Thank you for being progressive leaders in the profession!
Dan Bruce, DDS, is a diplomate of the American Board of Dental Sleep Medicine. He practices in Boise, Idaho. His credentials include: general dentist, educator, volunteer, husband, and father. He can be reached at [email protected].
References
1. "A Clinical Guide to Pediatric Sleep: Diagnosis and Management of Sleep Problems" by Jodi A. Mindell and Judith A. Owens; Lippincott Williams & Wilkins.
2. Chervin RD, Archbold KH. Hyperactivity and polysomnographic findings in children evaluated for sleep-disordered breathing. Sleep. 2001;24(3):313-320.
3. Chervin RD, Archbold KH, Dillon JE, Pituch KJ, Panahi P, Dahl RE, et al. Associations between symptoms of inattention, hyperactivity, restless legs, and periodic leg movements. Sleep. 2002;25(2):213-218.
4. Harvold EP, Tomer BS, Vargervik K, Chierici G. Primate experiments on oral respiration. Am J Orthod. 1981 Apr;79(4):359-372.
5. Prevalence of habitual snoring and associated neurocognitive consequences among Chilean school aged children. Int J Pediatr Otorhinolaryngol. 2012 Sep;76(9):1327-1331. doi: 10.1016/j.ijporl.2012.05.028. Epub 2012 Jun 27.